
![]() Contributed by Michelle Stram, MD, ScM and Bruce Rabin, MD, PhD
Contributed by Michelle Stram, MD, ScM and Bruce Rabin, MD, PhD
CLINICAL HISTORY
A 30-year-old woman presented to her GP with complaints of intermittently occurring joint pain in her wrists and ankles. Further questioning revealed that she had been experiencing occasional morning stiffness and a tingling sensation in her extremities. She denied any headache or constitutional symptoms beyond mild fatigue. She stated that she had been tested for ANA and rheumatoid factor in the past and they were both negative. Additional inquiry revealed that the patient has a positive family history for rheumatoid arthritis. On physical exam, the patient expressed mild tenderness at both wrists. The rest of the exam was non-contributory. The GP was concerned about a potential autoimmune disease process and ordered an erythrocyte sedimentation rate (ESR) and an antinuclear antibody (ANA) test. The results are listed in table 1. The GP then referred the patient to rheumatology.
Table 1. Initial laboratory tests
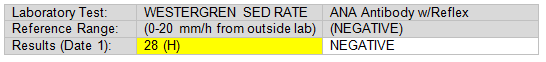
Several weeks later, the patient met with the rheumatologist. The rheumatologist elicited further details in the patient's history. The patient relayed that she had been experiencing pain in multiple joints, worse in her hands and feet; more recently, the paint had begun to involve her neck and knees to a lesser extent. She stated that her pain and stiffness were significantly worse in the morning, but that her symptoms diminish over time. When asked about pain medications, the patient stated that she had been taking ibuprofen and other non-steroidal anti-inflammatory drugs (NSAIDs) with only a minor improvement in her symptoms; furthermore, her pain and stiffness seemed to be getting worse since her initial visit with her GP. On exam, the rheumatologist noted mild synovitis in several proximal interphalangeal (PIP) joints of the hands, including the 2nd PIPs bilaterally and the right 3rd PIP. The patient expressed tenderness to palpation on many of the proximal and distal interphalangeal joints, as well as the metacarpal joints bilaterally. No rashes or skin lesions were seen; the rest of the physical exam was non-contributory. The rheumatologist ordered additional laboratory tests, as seen in Table 2.
Table 2. Further laboratory workup
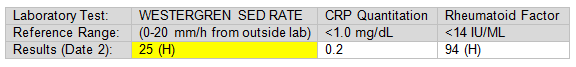
Upon receiving the laboratory results which showed a markedly elevated rheumatoid factor (RF) and mildly elevated ESR, the rheumatologist placed the patient on methotrexate with concurrent prednisone until the methotrexate became therapeutic.
The patient's joint pain and stiffness improved after starting the methotrexate and prednisone; however, the patient experienced side effects including weight gain secondary to the prednisone and chose to discontinue the medication. Despite continuing her methotrexate as prescribed, the patient presented to her rheumatologist again with worsening symptoms of joint swelling and stiffness, mainly localized to the hands and wrists. Physical exam showed markedly inflamed joints with synovitis identified in the MCP, PIP joints of the hands as well as the wrists. Additional laboratory tests were ordered (Table 3.) and a PPD was placed in anticipation that additional medication might be required to gain control over the disease.
Table 3. Additional laboratory test results

What is the diagnosis?