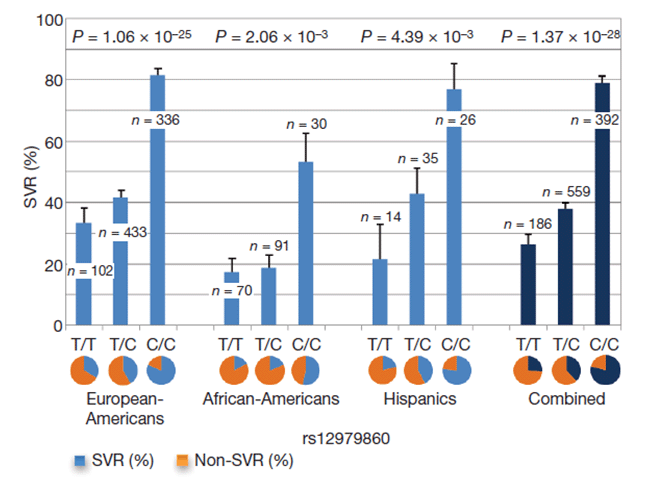
Figure 2. Percentage of SVR by genotypes of rs12979860 (Ge et al. Nature, 2009 [7]).
FINAL CONCLUSION
IL28B genotype is a strong predictor of response to standard therapy (pegylated interferon-α and ribavirin) among patients with chronic hepatitic C genotype 1 viral infection, although it must be considered in the context of other clinical and pathological factors, i.e. race, hepatic fibrosis, hepatic necrosis and inflammation, viral load, body habitus, comorbid conditions, and prior history of treatment response. At the current time, IL28B genotype should NOT be used as the sole criterion in the decision to treat with standard therapy, however, with the advent of direct acting anti-viral (DAA) agents it may play a role in choosing the duration of treatment and optical treatment regimen.
DISCUSSION
Background: IL28B genotype is the strongest predictor of SVR to standard treatment for HCV genotype 1-infected patients (pegylated interferon-α and ribavirin).
IL28B, also known as IFN-λ3, was first described in 2003 [2] and encodes a type 3 interferon (IFN). It is clustered with the IFN- λ1 and IFN- λ2 genes on chromosome 19q13.13 and is present in 2-4 copies in humans. IL28B interacts with a heterodimeric class II cytokine receptor consisting of IL-10Rβ and an orphan class II receptor chain IFN-λRα . It induces intracellular signaling pathways using JAK/STAT1 as well as MAPK, leading to interferon-sensitive response element (ISRE)-driven transcription, gamma-activated sequence-driven transcription, and STAT-independent events in the nucleus. IFN-λs have been shown to upregulate MHC class I antigen expression, lead to dose- and time-dependent inhibition of viral replication of HCV genotypes 1 and 2, enhance the anti-viral efficacy of IFN-αs, and result in the steady increase of known interferon-stimulated genes (ISGs)[3]. IL28B has been induced in various human cell lines by dsRNA, encephalomyocarditis virus, and vaccinia virus (in vivo), particularly in peripheral blood mononuclear cells and monocyte-derived dendritic cells. IFN- λ1 and IFN- λ2 have been induced in primary hepatocyte lines. However, expression of the IFN-λRα receptor seems to be limited to epithelial cells including primary hepatocytes in normal liver. [4]
A genome-wide association study in 2009 showed that IL28B genotype is associated with SVR to HCV, as well as higher baseline viral load. The study used the Illumina Human610-quad BeadChip to perform genome-wide SNP genotyping in 1,615 treatment-naďve patients with chronic HCV genotype 1 who underwent 48 weeks of treatment with pegylated interferon-α and ribavirin (PegIFN/RBV). SVR was defined as undetectable serum HCV RNA 24 weeks after cessation of treatment at 48 weeks, or undetectable viral levels at 12 weeks of treatment if no further follow-up occurred. The analysis identified a g.12007005C/T polymorphism (rs12979860) located 3,018 bp upstream from IL28B (thought to be outside its regulatory region [5]), that when present as CC over TT, conferred a 2-fold greater rate of SVR in Europeans (95% CI 1.8-2.3), 3-fold greater rate of SVR in African Americans (95% CI 1.9-4.7), and 2-fold greater rate of SVR in Hispanics (95% CI 1.4-3.2) (see Figure 2). The study results also showed that this allele (CC or TT) had a higher odds ratio in association with SVR compared to baseline viral load (< or >600,000 IU/mL), baseline fibrosis (scored 0-2 or 3-4), or race (European American or African American). IL28B genotype accounted for approximately half of the difference in SVR between European Americans and African Americans. Interestingly, the C allele was paradoxically, statistically significantly associated with higher baseline viral load (p=1.08x10-10) which has been replicated in other studies. However, based on a study showing that ISG expression may modulate the response to PegIFN [6], the authors suggested that patients with high baseline viral levels (and presumably the CC genotype) had low basal levels of hepatic ISG expression, and therefore when stimulated with PegIFN showed greater upregulation of ISGs and hence better treatment response. Conversely patients with high basal levels of hepatic ISG expression reaped no further benefit from treatment with PegIFN and were poor responders. [7]

Figure 2. Percentage of SVR by genotypes of rs12979860 (Ge et al. Nature, 2009 [7]).
The frequency of the IL28B C allele in the general population is 90% in East Asians, 75% in Caucasians, 70% in Hispanics, and 50% in African Americans.
Has the IL28B genotype been shown to predict endogenous (spontaneous) clearance of HCV in addition to exogenous clearance (SVR)?
Yes. Studies have shown the rs12979860 CC genotype to be associated with natural clearance of HCV (OR 0.33, 95% CI 0.25-0.45, p-value 3x10-13) [8].
Are any other loci within or near the IL28B gene locus linked to treatment response for HCV?
Yes. Studies have demonstrated 5 other SNPs near or involving the IL28B gene locus (2 outside the flanking putative regulatory regions, 1 within the upstream regulatory gene, 1 within an intron, and 1 within an exon) to be in association with SVR to HCV infection (see Figure 3) [5]. Currently, commercial laboratories are only offering analysis of the rs12979860 and rs8099917 polymorphisms. The rs8099917 polymorphism site is located 8.9 kb upstream from the IL28B start codon, and its GG genotype has been associated with a higher rate of failure to achieve SVR compared to the TT genotype (OR 2.39, 95% CI 1.16-4.94)[9,10]. The patient's IL28B CT genotype was based on rs12979860 only, and this is the "IL28B genotype" that will be referred to henceforth in this report.
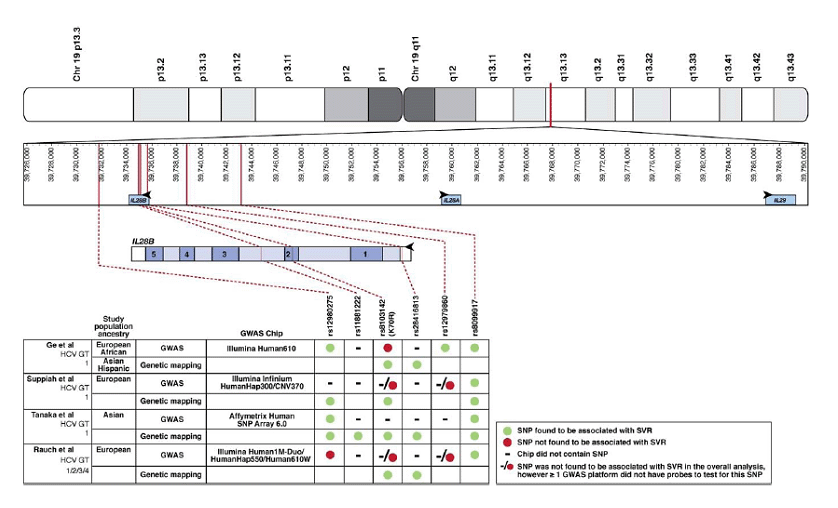
Figure 3. SNPs in IFN-λ gene cluster associated with HCV control (Balagopal etal. Gastroenterology, 2010 [5]). The IFN- λ gene cluster is shown in the top panel (chromosome 19). The positions of the relevant SNPs corresponding to published data are indicated in the second panel. The genomic structure of IL28B is depicted in the third panel, including its 5 exons, intervening introns, and flanking putative regulatory regions. The bottom panel shows which SNPs were associated with treatment response.
Has the exact mechanism of response to PegIFN/RBV treatment for HCV attributable to IL28B genotype been elucidated?
No, it has not been elucidated at the current time (also see Background). In light of the association between favorable IL28B genotype and high baseline viral load, the theorized impact of IL28B on SVR is intimately linked to its effect on the expression of ISGs in the liver (see Figure 4). Most, but not all subsequent studies have found the IL28B polymorphism to correlate with the expression of ISGs in the liver [11-14]. For example, one study demonstrated the differential expression of >150 genes in the liver in patients with the poor response CT/TT IL28B genotypes compared to CC patients; this list was dominated by canonical ISGs including MX1, OAS1/2/3, IFIT1/2/3, IFI6/27/44 and ISG15, and all were up-regulated >1.5-fold in CT/TT patients compared to CC patients [14]. These genes were previously shown to be among the main effector pathways of the IFN-mediated antiviral response. However, another study showed that ISG expression was significantly increased in nonresponders compared to responders across IL28B genotypes, indicating a lack of linkage between IL28B and ISGs [11].
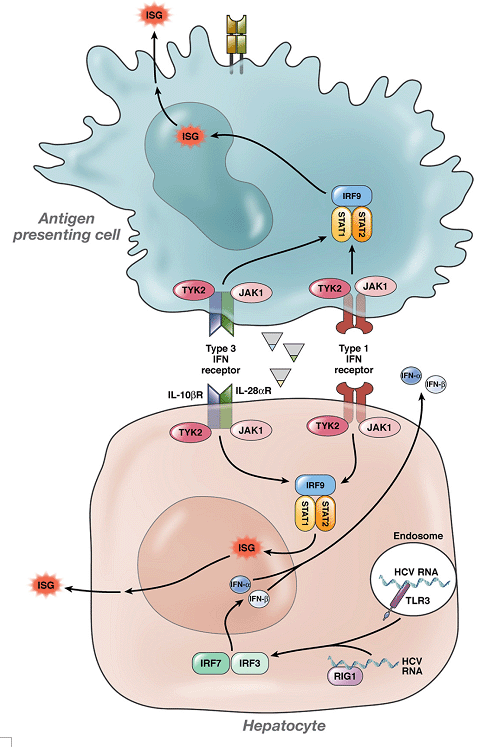
Figure 4. IFN-λ , -α , and -β signaling in response to HCV (Balagopal etal. Gastroenterology, 2010 [5]). HCV RNA is sensed by pattern recognition receptors such as RIG-I and TLR3, which signal using IFN-regulatory factor 3 and 7 and along with the transcription factor nuclear factor κB (NF-κB) induce expression of IFN -λ (plasmacytoid dendritic cells), IFN-α, and IFN-β (plasmacytoid dendritic cells and hepatocytes). When these factors bind their receptors, IFN -λR and IFN-α receptors 1 and 2, they induce Jak-STAT signaling, which results in the formation of IFN-stimulated gene factor 3, the transcription factor that upregulates hundreds of ISGs. Adapted and reprinted with permission by Balagopal et al. (Thio et al. Gastroenterology, 2010).
Is the role of IL28B in predicting response to standard HCV therapy limited to patients infected with HCV genotype 1?
Studies show that associations between IL28B genotypes and SVR are comparable between HCV genotype 1 and 4 patients [15]. Favorable IL28B genotype is associated with a ~2-fold increase in SVR among these patients.
Due to the poor prognosis predicted by HCV genotype 1 alone, even genotype 1 patients with favorable IL28B genotype experience lower rates of SVR than HCV genotype 2 and 3 patients. The data are conflicting in recent studies analyzing IL28B genotype and standard treatment response for HCV genotype 2 and 3-infected patients, and among these patients, it can only be concluded that IL28B genotype may be weakly associated with treatment response. A study of 268 patients with HCV genotypes 2 and 3 patients who were treated with PegIFN/RBV for 24 or 12 weeks (12 weeks only if achieved rapid virological response (RVR)) showed that rs12979860 was not associated with SVR in patients who achieved RVR regardless of treatment duration; however, in patients who did not achieve an RVR and who received 24 weeks of treatment, rs12979860 was significantly associated with SVR [16]. On the other hand, a different study of 267 patients with HCV genotypes 2 and 3 found an association of rs12979860 with RVR and also with SVR in patients who achieved RVR [17]. This latter study, however, included a much larger proportion of HCV genotype 3 over genotype 2 patients, and treatment regimens were more heterogeneous. Several other studies have yielded mixed results, but most studies have failed to show a significant association of IL28B genotype with SVR in HCV genotype 2 and 3 patients. [18]
Does donor and/or recipient IL28B genotype predict response to PegIFN/RBV for recurrent HCV after liver transplantation?
Yes, both donor and recipient IL28B genotypes are associated with response to PegIFN/RBV for recurrent hepatitis C after liver transplantation.
Retrospective studies have shown that both donor and recipient IL28B genotypes are associated with response to PegIFN/RBV for recurrent HCV, independently and in combination[19]. In addition, IL28B genotype may also predict treatment outcome after recurrent HCV in HCV genotypes 2 and 3- infected patients compared to non-transplanted patients. Lastly, IL28B genotype associates with the natural course of recurrent HCV, when described as fibrosis on graft biopsies, as it does in primary HCV. In turn, if prospective studies illustrate an effect of IL28B genotype on survival of liver-transplanted patients with recurrent hepatitis C, this could suggest a role for IL28B genetic testing in the allocation of liver grafts to HCV-infected patients. [18]
How will the role of IL28B genotype in predicting treatment response change with the advent of direct-acting antiviral (DAA) agents such as protease and polymerase inhibitors?
Several protease inhibitors (PIs) targeted against HCV genotype 1 are currently in phase 3 clinical trials, such as telaprevir (TVR) and boceprevir (BOC). Considering the added side effects of these agents and difficulty of complying with triple therapy, studies analyzing IL28B genotype in patients treated with PegIFN/RBV/PI triple therapy could potentially lead to its use in treatment strategy, for example assigning (1) standard PegIFN/RBV only x 24-48 weeks or (2) triple therapy x 12 weeks if RVR is achieved in CC patients. Conversely, CT or TT patients could be treated with triple therapy for 24-48 weeks, or standard PegIFN/RBV therapy for 48-72 weeks if PIs are contraindicated. Of course, the aforementioned clinical trials have been limited to investigating HCV genotype 1 patients. [18]
Other DAA agents in advanced clinical development include HCV NS5B polymerase inhibitors, HCV NS5A inhibitors, or the cyclophilin A inhibitor Debio-025 (alisporivir). Preliminary data from a Japanese study analyzing 72 HCV genotype 1 patients who were either treated with triple therapy PegIFN/RBV/TVR) x 12 weeks or the same plus an additional 12 weeks of PegIFN/RBV showed that overall SVR rates of 45% after 12 weeks and 67% after 24 weeks of total therapy Additionally, both rs809917 TT genotypes and rs12979860 CC genotypes were associated with a > 2-fold chance of achieving SVR after triple therapy[20]. In contrast, viral kinetics during treatment with PI TMC435 in combination with PegIFN/RBV were only slightly influenced by IL28B genotype [21]. Since IL28B genotype is associated with differences in early treatment viral kinetics during standard treatment, this suggests a higher risk of resistance development to DAA agents in patients with unfavorable IL28B genotypes, although DAA agents vary in their defenses against resistance development. Thus far, IL28B genotype seems to play a lesser role during triple therapy, although additional research is required to elucidate this relationship. [18]
Consequences for the patient
This patient has HCV genotype 1a infection, and the IL28B CT (intermediate) genotype. His liver biopsy showed mildly active chronic hepatitis C, therefore he could be theoretically cleared for renal transplant. Should he decide to pursue treatment with PegIFN/RBV again, as an African American he would be predicted to have an 18% chance of SVR solely based on IL28B genotype (see Figure 2)[7]. However, this information alone is not sufficient to make a clinically-sound decision to either initiate or withhold standard therapy, especially considering that the positive predictive value of IL28B genotype for SVR is <100%. The patient's IL28B genotype must be considered in the context of other clinical factors predicting response to standard therapy, including his HCV genotype, race, renal function, and history of nonresponse after 12 weeks of standard therapy. These factors likely outweigh any potential treatment benefit attributable to his low viral load and thin body habitus. He has not yet returned for follow-up with the gastroenterology and hepatology team.
Summary: What clinically useful information can be gleaned from the IL28B genotype of a patient infected with HCV?
![]() Contributed by Rashi Singhal, MD, MPH, and Marie DeFrances, MD, PhD
Contributed by Rashi Singhal, MD, MPH, and Marie DeFrances, MD, PhD