![]() Contributed by Sarmad Al-Karawi MD1, Michael Vassilyadi MD1, Jean Michaud MD2
Contributed by Sarmad Al-Karawi MD1, Michael Vassilyadi MD1, Jean Michaud MD2
![]() Divisions of 1Neurosurgery and 2Anatomical Pathology, Children's Hospital of Eastern Ontario, University of Ottawa, Ottawa, Canada
Divisions of 1Neurosurgery and 2Anatomical Pathology, Children's Hospital of Eastern Ontario, University of Ottawa, Ottawa, Canada
CLINICAL HISTORY AND IMAGING
An 11-year-old boy presented with a 10 month history of lumbar back pain and paresthesia in his thighs to the knees bilaterally, left greater than right. This pain exacerbated two weeks after falling out of a pickup truck directly onto his back. The pain was 8/10 in severity, worse at night and while supine, and typically lasted 20 minutes in duration. Relieving factors included warm baths, massage, and acetaminophen or ibuprofen. The pain was not exacerbated with physical activity and no appreciable motor weakness. There was no bladder or bowel incontinence. Since the accident, he noticed the pain was worsening in intensity and duration. Neurological exam did not reveal any objective sensory deficit.
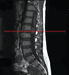
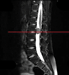
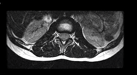
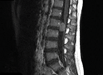
 Lumbar spine x-ray was only significant for spina bifida occulta at the L5 level. Magnetic resonance imaging (MRI) of the spine (Figures 1a, 1b, 1c and 1d) demonstrated a 1.4 x 2.3 x 1.8 cm moderately contrast-enhancing, intradural extramedullary mass at L2-L3. This mass was located immediately below the conus medullaris and compressed the cauda equina posteriorly and laterally. There were no intracranial abnormalities on MRI of the brain.
Lumbar spine x-ray was only significant for spina bifida occulta at the L5 level. Magnetic resonance imaging (MRI) of the spine (Figures 1a, 1b, 1c and 1d) demonstrated a 1.4 x 2.3 x 1.8 cm moderately contrast-enhancing, intradural extramedullary mass at L2-L3. This mass was located immediately below the conus medullaris and compressed the cauda equina posteriorly and laterally. There were no intracranial abnormalities on MRI of the brain.
The patient underwent a L1 to L3 laminectomy and excision of the spinal canal mass (Figure 2). Post-operatively, he developed 3/5 motor weakness in left foot dorsiflexion and mild left leg numbness both of which resolved by his 5 week follow-up.
GROSS AND MICROSCOPIC PATHOLOGY
Gross appearance of the intradural, extramedullary specimen demonstrated an ovoid mass with a homogenous, bright yellow surface (Figure 2). Intraoperatively, the smears suggested an astrocytic lesion but both the smears and the frozen section, showed a granular eosinophilic appearance. There was no significant atypia or aggressive features (Figures 3a and 3b).
Light microscopy (Figure 4) showed compact round, polyhedral, and fusiform shaped cells surrounded by a thin pseudocapsule with focal chronic inflammation. They were arranged in small nests or sheets with delicate stroma. The nuclei were generally round and uniform with a few demonstrating hyperchromasia or hypertrophy with unusual contour. The cytoplasm was abundant and characterized by a uniform granularity occasionally admixed with larger eosinophilic globules (Figures 5a, 5b, 5c, 5d, and 5e). Mitoses were rare and necrosis was absent. A peripheral nerve root was seen penetrating into the mass.
The periodic acid-Schiff (PAS) staining was positive in the globules and less obvious in the fine granularity (Figure 6). Some cells had minute ovoid, crystalloid and angulated PAS positive inclusions (Figure 7). The Grimelius stain showed generalized brown granular positivity with axons staining black (Figure 8). Iron and von Kossa stains were negative.
By immunohistochemistry, vimentin was positive in all cells. Dense staining of the nuclei and cytoplasm by S-100 protein was present (Figure 9). A moderate number of CD-68 positive macrophages were admixed with the large granular cells (Figure 10). EMA stained only the perineurium of the noted peripheral nerve root. Neurofilament (Figures 11a, 11b, 11c, 11d, and 11e) and synaptophysin confirmed the presence of axons in the mass, predominantly at the periphery. Collagen IV antibody was seen underlining the lobules at a thickness of 2-3 cells (Figure 12). Chromogranin, GFAP, TTF-1 and progesterone receptor antibodies were negative.
The ultrastructure showed numerous cells with variable interdigitating projections. The cytoplasm of these cells contained numerous pleomorphic secondary lysosomes of various types: autophagosomes, residual bodies, multivesicular bodies. A second type of cells with fibrohistiocytic features showed membrane bound structures, the so-called angulate bodies (Figure 13). Basement membrane was present around nests of cells but not around each one individually. What is the diagnosis?
 International Society of Neuropathology
International Society of Neuropathology