DIAGNOSIS
Intradural, extramedullary granular cell tumour.
DISCUSSION
Granular cell tumor (GCT) is a rather uncommon neoplasm. In 1926, Abrikossoff, a Russian pathologist, described GCT on the basis of five reported cases under the name of "myoblastenmyome" (5). Its histogenesis remains speculative. The initial specification of myoblastoma was prompted by the resemblance of the granular cells to skeletal muscle cells in paraffin sections, and it received some support from tissue culture observations; however, the development of electron microscopy and immunohistochemical studies ruled out this possibility and a relationship to Schwann cell neoplasms became the favored hypothesis (5).
GCTs are often benign soft tissue mass, most commonly found in the skin, head and neck region (especially the tongue), ovaries, and breast tissue. In the CNS, the neurohypophyseal region is most often involved (5, 7). Malignant GCTs are very uncommon, representing around 1% of all GCTs (7, 11). Malignant GCT features include rapid growth, larger size, necrosis, metastasis, and involvement of adjacent tissue (7, 11). A large number of malignant GCTs have benign histological features (5). So far, no malignant form has been described in the pediatric population (7). Mucosal tumors are occasionally challenging to diagnose histologically, as they are repeatedly associated with overlying surface epithelial pseudo-epitheliomatous hyperplasia (7,11).
GCTs are typically present in patients between the third and sixth decades, with a female-to-male ratio of 2:1 (4, 5, 7, 11). They have predilection toward African-American ethnic group (7). GCTs are typically solitary soft tissue lesions; however, about 10% found to be multiple (5).
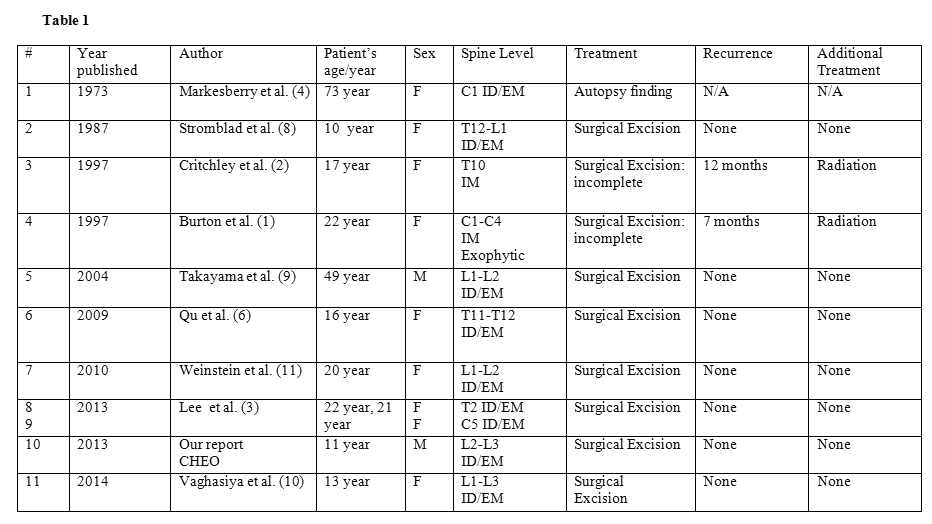
Spinal intradural GCTs are exceptionally rare, with only ten other cases in the literature (see Table with references). The current case included, they are localized evenly throughout the spinal canal: three cases in the cervical region, three cases in the thoracic region, four cases in the lumbar region and one case in the thoraco-lumbar region. We report the clinical, MRI, histological and immunohistochemical findings of an intradural extramedullary GCT. This report highlights these features in the context of a review of the literature.

Abbreviations: F: female; M: male; ID: intradural; EM: extramedullary; IM: intramedullary
Although GCTs are benign histologically, spinal intradural location can cause serious neurological deficits if not diagnosed early and treated correctly due to the anatomic limit of the canal. Clinical symptoms can include backache, radicular pain, and slowly progressive neurological findings, such as weakness, paresthesia, gait abnormality, impotence, and bowel and bladder function problems. Rarely, headaches due to subarachnoid hemorrhage may be seen (11).
The commonest intradural extramedullary tumors are schwannoma, neurofibroma, myxopapillary ependymoma, meningioma, paraganglioma, and intradural disseminations. For many of these, the imaging features may be indistinguishable (11). Schwannoma is typically hypo or iso-intense compared to the spinal cord on T1-weighted images and hyper-intense on T2-weighted images. After administration of contrast material, it shows marked and homogeneous or target-like enhancement (7). Intradural extramedullary meningioma shows the same appearance as schwannoma on MRI (6). In the cauda equina region, myxopapillary ependymoma, which arises from the filum terminale, may also show similar MR findings (7). Our case was indistinguishable from those tumors on MRI.
Histologically, GCT is composed of large, round, or polygonal cells with small dense nuclei. Cytoplasm contains abundant eosinophilic granules, which are variably positive with the periodic acid Schiff (PAS). These histological features are different from those of schwannoma. Schwannoma is composed of densely packed, highly ordered spindle cells or more loosely textured myxoid stroma (7). By immunohistochemistry, GCT cells are positive for NSE and S-100 protein, which suggest that GCT originates from a Schwann cell (5, 7). Interestingly, in our case, TTF-1 is negative. This is a different expression that the one initially reported by Lee and al. (3) in sellar region tumors. This suggests a different cell of origin, and, in our view, reinforces the likely Schwann cell origin of the non-sellar GCTs. The closest differential diagnosis histologically would be granular cell astrocytic tumors which are GFAP positive and would be unusual in an extramedullary nodular shaped presentation (7). One intramedullary GCT was however reported (2).
The treatment of choice for a symptomatic or malignant GCT is a surgical excision; however, benign and small asymptomatic GCT may not require surgery. Incomplete resection of the tumor may result in local recurrence even with a benign GCT (7, 11).
REFERENCES
![]() Contributed by Sarmad Al-Karawi MD, Michael Vassilyadi MD and Jean Michaud MD
Contributed by Sarmad Al-Karawi MD, Michael Vassilyadi MD and Jean Michaud MD
 International Society of Neuropathology
International Society of Neuropathology