![]() Contributed by Sahr Syed, MD, Amir Ali Borhani, MD and Sheldon Bastacky, MD
Contributed by Sahr Syed, MD, Amir Ali Borhani, MD and Sheldon Bastacky, MD
CLINICAL HISTORY
A middle aged male with an abnormal digital rectal exam with imaging consistent with a seminal vesicle mass. The most recent serum PSA level was 0.75 ng/mL. Due to clinical suspicion about the mass originating from the prostate gland, the patient underwent a core needle biopsy procedure. Core fragments were received from the patient and were labeled as 'prostatic tissue' which showed a malignant spindle cell neoplasm with focal staining for cytokeratin AE1/AE3, with a morphologic differential diagnosis which included carcinosarcoma and high-grade sarcoma (prostatic stromal sarcoma, solitary fibrous tumor with high-grade sarcomatous transformation). Due to paucity of tissue, further classification was not possible and therefore the patient underwent a radical prostatectomy.
IMAGING STUDIES
MRI studies showed a large nodule within the distal seminal vesicle lumen and in the distal ejaculatory duct, measuring 1.8 x 1.7 x 1.3 cm, which showed abnormal early enhancement.
GROSS EXAMINATION
The patient's radical prostatectomy specimen showed a firm yellow-white area with focal cystic spaces, 2.5 x 2.0 x 2.0 cm, on the cut surface of left seminal vesicle.
MICROSCOPIC PATHOLOGY
The left seminal vesicle was largely replaced by a biphasic neoplasm composed of a stromal proliferation of pleomorphic malignant spindled and epithelioid cells with eosinophilic to focally clear cytoplasm. The epithelial component did not appear malignant. There was varying degree of nuclear pleomorphism with some of the neoplastic cells showing more than one nucleus, and focal moderate-sized nucleoli. In the areas showing a lower grade component, there was a fibromyxoid stroma which appeared to cause expansion of the subepithelial stroma. There were also entrapped seminal vesicle glands present. Additionally, in the higher grade areas, there was a loss of seminal vesicle epithelium with the seminal vesicle stroma replaced by high-grade malignant cells (malignant spindle cells with a vaguely fascicular architecture and malignant epithelioid cells with variably clear cytoplasm and a solid architecture). Mitotic activity was present (up to 5 mitoses per 10 hpf) but only rare foci necrosis were identified, constituting less than 1% of the tumor.
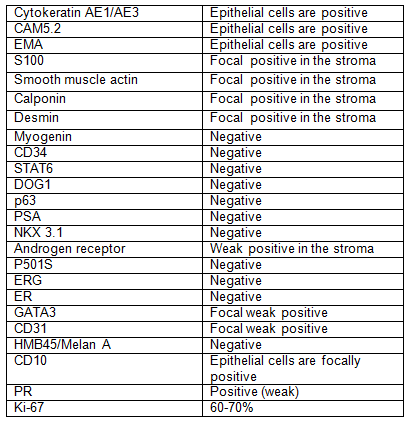
IMMUNOHISTOCHEMISTRY