![]() Contributed by Huina Zhang, MD, PhD and Esther Elishaev, MD
Contributed by Huina Zhang, MD, PhD and Esther Elishaev, MD
CLINICAL HISTORY
A teenage female presented with secondary amenorrhea. The patient had 1 menstrual cycle 3 years ago and has had no menses since. Laboratory work-up was negative for pregnancy test, mildly increased calcium level (11.7 mg/dL, normal range: 8.5-10.2 mg/dL) and CA 125 (43 Units/ml, normal range: 0-20 Units/ml). Prolactin, TSH, AFP, Inhibin A, Inhibin B and CEA were normal. Imaging revealed a 13 x 11.8 x 8.6 cm, predominately cystic left pelvis mass, with multiple internal septations. Her past medical history was not contributory. Patient underwent left salpingo-oophorectomy, omentectomy and tumor debulking with intraoperative frozen section consultation.
GROSS EXAMINATION
The 930.9 g tubo-ovarian complex consisted of a 20.0 x 16.0 x 8.0 cm large mass, with no recognizable normal ovarian parenchyma grossly and an unremarkable fallopian tube. The cut surface was gray, "fish-flesh", soft with foci of hemorrhage and necrosis.
MICROSCOPIC EXAMINATION
Microscopically, the majority of main tumor was growing in large nests, sheets and cords with focal follicle-like structures and geographic areas of necrosis. It was predominantly composed of small cells with hyperchromatic nuclei, round to oval nucleus with irregular nuclear contour, inconspicuous to occasional conspicuous nucleoli and minimal cytoplasm. This component was variably admixed with a population of larger cells, which as the name implies composed of cells with abundant eosinophilic cytoplasm, with central or eccentric round to oval nuclei, pale chromatin and prominent nuclei. Both, the small and large cell components demonstrated brisk mitotic activity. All staging biopsies and omentectomy were composed of large cell component.
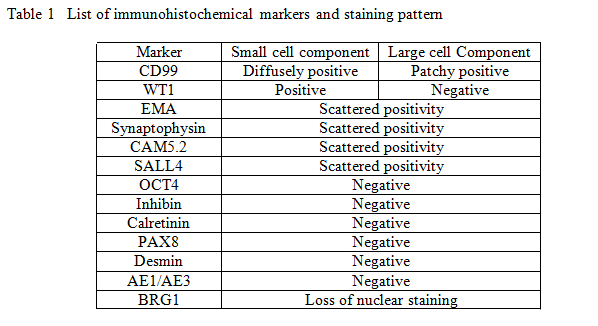
An extensive panel of immunohistochemical stains was performed. Overall, the staining pattern was strong and diffuse in small cell component compared to patchy weak staining pattern in the large cell component.