FINAL DIAGNOSIS
Neurenteric Cyst
DISCUSSION
Neurenteric cysts (also called endodermal, enteric or enterogenous cysts) are benign cysts lined by columnar or cuboidal ciliated and/or goblet cell epithelium (1). Squamous metaplasia is commonly seen and some cysts show more complex forms with seromucinous glands, lymphoid tissue, and smooth muscle (2).Their exact etiology is unknown, however they are thought to result from a failure of the separation of the neurenteric canal, resulting in primitive endodermal cells incorporated into the notochord (3).
Neurenteric (NE) cysts occur at all ages, with a slight male predominance, and are most commonly seen in the spinal intradural-extramedullary compartment, most frequently in the cervical region (1, 2). Although they rarely present intracranially, the posterior fossa is the most common intracranial site and they are usually anterior to the brainstem (4).
Radiologically, NE cysts are typically sharply demarcated and show varied MR signal intensity depending upon the protein content of the cyst fluid. The cyst fluid is usually iso- to hyperintense compared to CSF on T1 and hyperintense on T2 weighted images. If inspissated, they can be hypointense. Most cases do not enhance in post-contrast images, with only rare cases showing rim-enhancement (5). In the current case, the radiology was unusual with the enhancement seen, which may be due to an adjacent brainstem inflammatory reaction/infection.
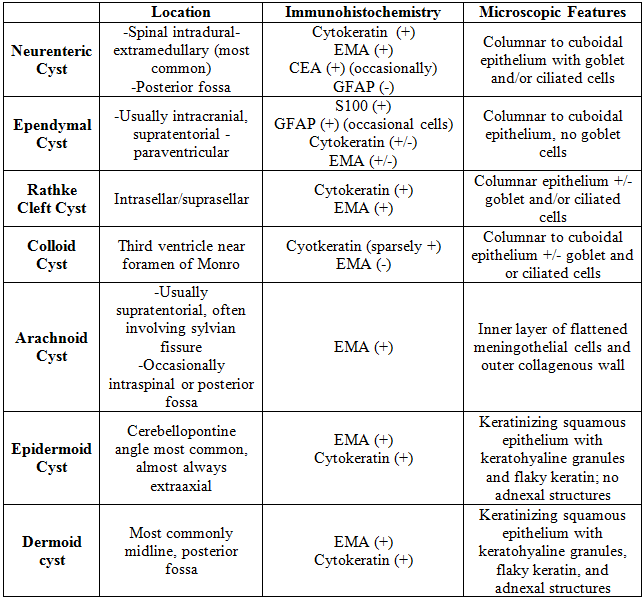
The differential diagnosis for an intracranial neurenteric cyst includes ependymal cyst, Rathke cleft cyst, colloid cyst, epidermoid/dermoid cyst, and arachnoid cyst. Microscopically, the diagnosis can often be made based on the location and presence of goblet or ciliated cells. Additionally, immunohistochemistry can be helpful as neurenteric cysts are positive for Cytokeratin, EMA, and occasionally CEA and are negative for GFAP. The presence of goblet cells in the epithelium helps distinguishes NE cysts from ependymal cysts, which are typically intracranial. Additionally, ependymal cysts are positive for S100 with occasional GFAP-reactive cells. Rathke cleft cysts and colloid cysts may be histologically identical to NE cysts, but Rathke cleft cysts are seen in the intrasellar/suprasellar location and colloid cysts are seen in the rostral dorsal third ventricle near the foramen of Monro (2). Epidermoid/dermoid cysts show a keratinizing squamous epithelium with keratohyaline granules and flaky keratin. Adnexal structures are only present in dermoid cysts (1). Arachnoid cysts are filled with CSF and are composed of an inner layer of flattened meningothelial cells and an outer collagenous wall (2). See the table below for the differential diagnosis summary:

Treatment involves excision, however recurrence is possible. Very rarely, malignant transformation to adenocarcinoma can occur (6). In the current case, the patient was discharged on steroids and antibiotics and subsequent imaging showed decreased enhancement in the medulla with no new lesions seen.
REFERENCES
![]() Contributed by Anne Shepler, MD and Julia Kofler, MD
Contributed by Anne Shepler, MD and Julia Kofler, MD