DIAGNOSIS
Clear cell papillary renal cell carcinoma
DISCUSSION
Clear cell papillary renal cell carcinoma (CCPRCC) is a type of renal cell neoplasm recently included in the new 2016 WHO classification of renal tumors [1]. Although first described in patients with end stage kidney disease [2], it was later identified in patients with normal renal function [3]. Microscopically the tumor is composed of clear cells arranged in papillary, solid or cystic areas. Despite the overlap with clear cell renal cell carcinoma (usual type) and papillary renal cell carcinoma, this entity has unique morphological, immunohistochemical and molecular features [4].
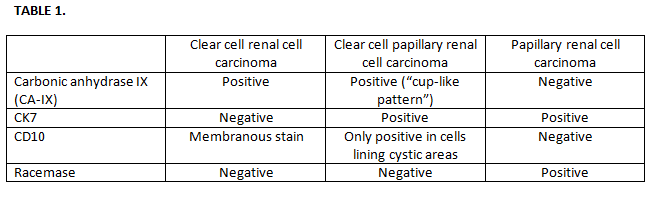
By morphology, this tumor can be solid or cystic and exhibit a variety of architectural arrangements. The neoplastic cells typically have clear cytoplasm and low nuclear grade. The most distinguishable feature is the presence of papillary or tubular structures lined by a single layer of clear cells with the nuclei characteristically arranged away from the basement membrane [3]. A careful microscopic inspection of the tumor is required, as sometimes this feature is found focally and can be easily missed. By immunohistochemistry, clear cell papillary renal cell carcinoma is positive for both carbonic anhydrase IX (CA-IX) and CK7 [5). Carbonic anhydrase IX (CA-IX) shows a unique staining pattern that helps to differentiate this neoplasia from clear cell renal cell carcinoma, stain positive in the basolateral lining of cells and is absent in the luminal aspect (cup-like pattern). CD10 is negative except in cystic areas where highlight the cyst lining cells exclusively. Racemase is negative [6] (Table 1).

Genetically this tumor diverges from clear cell renal cell carcinoma by lack of chromosome 3p deletion or Von Hippel-Lindau (VHL) gene mutations and from papillary renal cell carcinoma by lack of polysomy of chromosomes 7 and 17 [7, 5].
The prognosis for this type of renal tumor is excellent; no cases of lymph node or distant metastasis had been reported in patients diagnosed with pure clear cell papillary renal carcinoma. Consequently, some pathologists are currently advocating changing the name for "clear cell papillary neoplasm of low malignant potential" [8].
In summary, clear cell papillary renal cell carcinoma is a neoplasia recently included in the WHO classification of renal cell tumors that exhibits unique morphological, immunohistochemical and molecular features. Being able to recognize this entity is important because of the low malignant potential and excellent prognostic implication for patients.
REFERENCES
![]() Contributed by Angela Sanguino Ramirez MD, MPH; Thu Tran MD and Rajiv Dhir MD
Contributed by Angela Sanguino Ramirez MD, MPH; Thu Tran MD and Rajiv Dhir MD