![]() Contributed by Michelle Stram, MD and Jeffrey Nine, MD
Contributed by Michelle Stram, MD and Jeffrey Nine, MD
CASE PRESENTATION
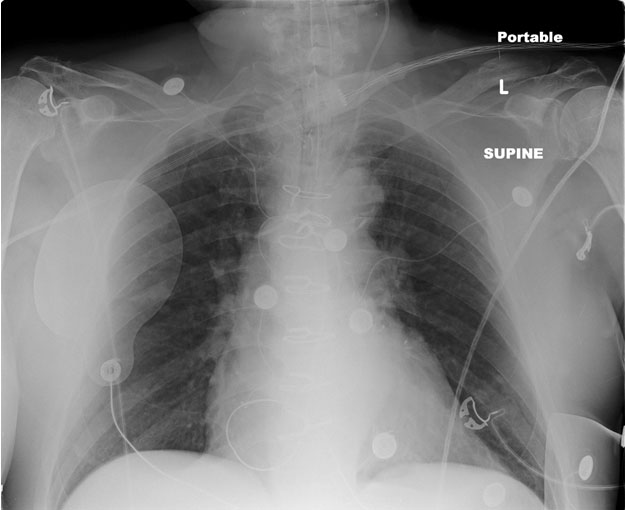
A Caucasian man in his 70's was visiting his neighbors when he had a witnessed syncopal episode. Shortly after, he had a second episode and an ambulance was called. The patient became unresponsive before EMS arrived and required CPR. EMS was able to restore the patient's circulatory function en route to the hospital. Upon arrival in the emergency department, a chest x-ray was obtained.
Figure 1. Chest x-ray revealed bilateral hilar lymphadenopathy and increased pulmonary markings.
The patient had an extensive past medical history including significant three vessel coronary artery disease status-post coronary artery bypass grafting. He also had mildly diminished pulmonary function secondary to COPD.
Labs drawn in the ED showed that the patient's troponin I was 0.50 ng/mL (reference range: <0.1 ng/mL), and an EKG revealed both right bundle branch and left anterior fascicular block. Despite the efforts of the clinical team, the patient had another cardiac arrest and could not be revived. The patient's family was consented and an autopsy was performed.
Autopsy showed severe atherosclerotic cardiovascular disease with three saphenous bypass grafts from the aorta to the left anterior descending artery, the diagonal branch of the left anterior descending artery and the marginal branch of the left circumflex artery. There was greater than 90% occlusion of the left main coronary artery by calcified atherosclerosis. A subendocardial scar was identified in anterolateral aspect of the heart consistent with a prior myocardial infarction. Multiple calcified atherosclerotic plaques were identified throughout the abdominal and thoracic aorta. Bulky bilateral hilar and subcarinal lymphadenopathy was identified. There was mild pulmonary fibrosis with both a subpleural and perivascular distribution. Upon sectioning, small noncaseating and scarred foci suggestive of granulomas were seen in the lung parenchyma as well as in the hilar lymph nodes. Histochemical staining with ziehl neelsen, grocott, and PAS demonstrated that the granulomas were negative for organisms.
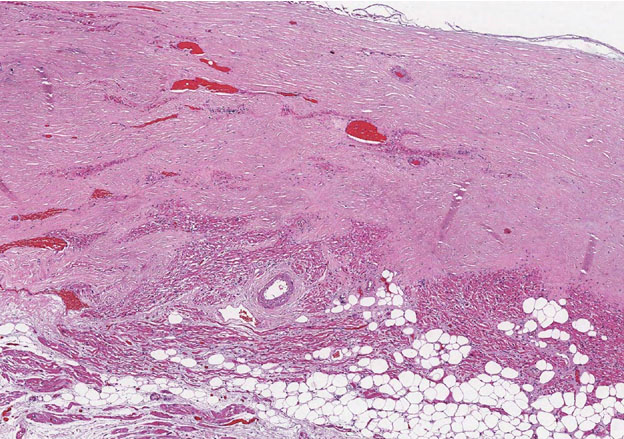
Figure 2. Histologic section of the myocardial conduction system revealed focal microscopic epithelioid granulomas near the AV nodal tissue (H&E).