
![]() Contributed by Daniel D. Rhoads, MD; A. William Pasculle, ScD
Contributed by Daniel D. Rhoads, MD; A. William Pasculle, ScD
PATIENT HISTORY
A man in the seventh decade of life lives independently and has end stage liver disease. He presented to the ED with complaints of increasing gait disturbances over the past several weeks and new onset diplopia and blurry vision. He also complains of persistent headaches, body aches, and intermittent confusion. He had nausea and vomiting, which had impaired his ability to take his lactulose as prescribed. Recently, he had been admitted to the hospital multiple times for what was diagnosed as hepatic encephalopathy. The patient was admitted to the hospital and neurology was consulted.
Neurology identified a focal cranial nerve deficit, and an MRI revealed restricted diffusion, which was suspicious for small acute infarcts and revealed diffuse leptomeningeal enhancement suggestive of meningitis.
Hematology findings were similar to the patient's baseline:
Plasma chemistry findings were mostly similar to the patient's baseline:
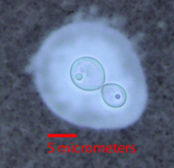
 Cerebrospinal fluid (CSF) analysis identified an elevated opening pressure (>40 cm water [reference range 10-20 cm water]) elevated protein, elevated lactate, and low glucose. WBCs were 21/mm3 and were 90% lymphocytes (some atypical) and 10% monocytes. The following images were collected from the CSF using 1000x oil-immersion magnification. Figure 1 is a Gram stain that was prepared from concentrated, centrifuged CSF; and Figure 2 was prepared with India ink and CSF.
Cerebrospinal fluid (CSF) analysis identified an elevated opening pressure (>40 cm water [reference range 10-20 cm water]) elevated protein, elevated lactate, and low glucose. WBCs were 21/mm3 and were 90% lymphocytes (some atypical) and 10% monocytes. The following images were collected from the CSF using 1000x oil-immersion magnification. Figure 1 is a Gram stain that was prepared from concentrated, centrifuged CSF; and Figure 2 was prepared with India ink and CSF.
What is the diagnosis and what are the methods which the laboratory can use to identify this infection?