
![]() Contributed by Stell Patadji, MD and Lirong Qu, MD, PhD
Contributed by Stell Patadji, MD and Lirong Qu, MD, PhD
PATIENT HISTORY
The patient is a 55-year-old man who presented to the ED with gradual worsening of weakness. The patient reports that he had been fatigued for one month, having to rest constantly after work, and feeling exhausted with minimal exertion. He also reported feeling lightheaded with rising, as well as having epigastric abdominal pain, which was not associated with food. Four days prior to the presentation, the patient began to have black, tarry stools. He was evaluated in his primary care physician's office the day prior, and was found to have hemoglobin of 6.5 g/dL. His prior baseline from two weeks ago was 15.3 g/dL. He was subsequently referred to the ED.
The patient has a history of pancolonic ulcerative colitis diagnosed in 1979 and now in remission. He has not been on medication for 17 years, but he did receive treatment with prednisone around time of diagnosis, then sulfasalazine. He had undergone recent surveillance EGD and colonoscopy a month ago, which was unchanged from previous studied. He also has gastroparesis, not symptomatic for several years. He is on ASA 81 mg. He takes a PPI for GERD which is well-controlled.
In the ED, his vital signs were: pulse: 121, blood pressure: 127/85, respiratory rate: 20, and oxygen saturation: 99% on room air. Physical examination was remarkable for generalized pallor, mild tachycardia, and diastasis of rectus (also known as abdominal separation). Nasogastric lavage was negative, but the fetal occult blood test was positive. Pertaining labs are listed below:
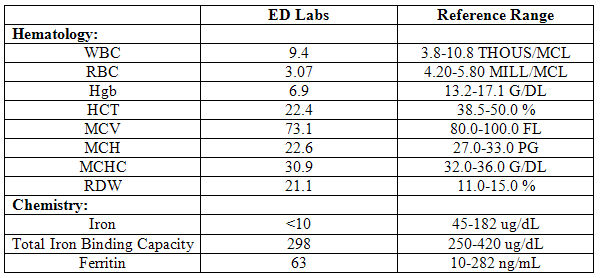
Following examination and GI consult, he was admitted on to the floor for further work up of his GI bleeding. Packed red blood cells were ordered for transfusion with goal hemoglobin of greater than 8 g/dL. Seventy milliliters within the transfusion of the first packed red blood cell, the patient became hypotensive and diaphoretic with chill/rigor and dyspnea. Pre and post vital signs were:

A condition C was called.