Final Diagnosis -- Suspicious for Non-Hodgkin Lymphoma
DIAGNOSIS Suspicious for Non-Hodgkin Lymphoma
IMMUNOHISTOCHEMISTRY

On immunohistochemical staining of the cell block, the cells are positive for CD20, CD23 and CD5. The cells are also positive for lymphoid-enhancer-binding factor 1 (LEF1), a recently characterized marker for CLL/SLL (1). A smaller population of associated, benign T lymphocytes demonstrates staining for CD3 and CD5 (Figure 7, Immunohistochemistry).
FLOW CYTOMETRIC STUDIES
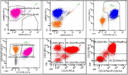
The flow cytometric immunophenotype of the B lymphocytes matches what is seen on immunohistochemical staining of the cell block, with a monotypic, lambda light chain restricted population that is positive for CD20, CD19, CD5, and CD23 and negative for CD10 and FMC-7, representing approximately 67% of total events (Figure 8, Flow cytometric studies). These characteristics are consistent with a diagnosis of chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL).
MOLECULAR AND CYTOGENETIC STUDIES

Molecular studies demonstrate that, as expected, the FNA specimen is negative for molecular markers of thyroid carcinoma, including mutations in BRAF, NRAS61, HRAS61, KRAS12/13, and RET/PTC1, RET/PTC3 and PAX8/PPARΥ rearrangements. On fluorescence in situ hybridization (FISH), 92.2% of cells demonstrate deletion of 13q14.3, the most frequent cytogenetic abnormality seen in CLL (Figure 9, Deletion of 13q14.3 by fluorescence in situ hybridization (FISH) ) (2).
DISCUSSION
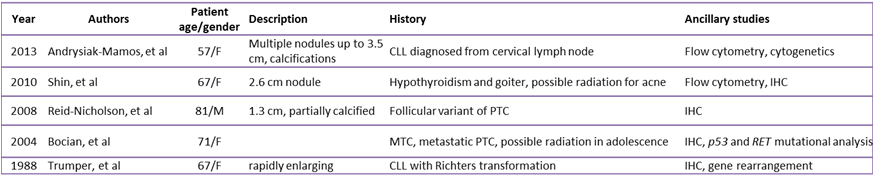
- The thyroid gland does not contain lymphatic tissue. Therefore, lymphoma involving the thyroid is quite rare (1-8). The most common lymphomas to involve the thyroid gland are diffuse large B cell lymphoma (DLBCL), comprising approximately 50% of cases, and mucosa-associated lymphoid tissue (MALT) lymphoma that sometimes occurs in association with chronic lymphocytic (Hashimoto's) thyroiditis, comprising 23% of thyroid lymphoma (3). Only 4% of lymphomas involving the thyroid are CLL/SLL, which is otherwise one of the most common B cell lymphomas (3). 5 cases of CLL/SLL involving the thyroid have been previously reported (4-8). Two were in patients previously diagnosed with CLL/SLL. Interestingly, two were in patients who were concurrently diagnosed with thyroid carcinoma, both papillary and medullary. Two cases were discovered in patients with a reported history of prior radiation to the face/head and neck. Table 1 summarizes the five reported cases of CLL/SLL involving the thyroid.
- One diagnostic pitfall regarding diagnosis of thyroid lymphoma is the much more common occurrence of chronic lymphocytic (Hashimoto's) thyroiditis that can mimic lymphoma and vice versa, particularly CLL/SLL whose cells are small and can be confused with benign lymphocytes. Features more consistent with chronic lymphocytic thyroiditis include Hurthle cell change among the thyroid follicular cells as well as a heterogeneous-appearing population of lymphocytes. Immunohistochemical stains and flow cytometric studies can be very helpful in distinguishing these entities.
- In a 2011 study performed by Tandon et al(1), LEF1 staining was found to be positive in 100% of 92 CLL specimens tested. Other lymphomas with small cell morphology, including mantle cell lymphoma, low grade follicular lymphoma and marginal zone lymphomas were all negative for this marker. However, the LEF1 stain was found to be positive in subsets of high grade follicular lymphoma and diffuse large B cell lymphoma.(1)
TABLE 1: Summary of reported cases of CLL/SLL involving the thyroid
This case has been contributed, as July 2013 Case of the Month, to the International Academy of Cytology (IAC)
REFERENCE
- Tandon B, Peterson L, Gao J, Nelson B, Ma S, Rosen S, et al. Nuclear overexpression of lymphoid-enhancer-binding factor 1 identifies chronic lymphocytic leukemia/small lymphocytic lymphoma in small B-cell lymphomas. Mod Pathol. 2011;24:1433-43.
- Gardiner AC, Corcoran MM, Oscier DG. Cytogenetic, fluorescence in situ hybridisation, and clinical evaluation of translocations with concomitant deletion at 13q14 in chronic lymphocytic leukaemia. Genes Chromosomes Cancer. 1997;20:73-81.
- Thieblemont C, Mayer A, Dumontet C, Barbier Y, Callet-Bauchu E, Felman P, et al. Primary thyroid lymphoma is a heterogeneous disease. J Clin Endocrinol Metab. 2002;87:105-11.
- Andrysiak-Mamos E, Becht R, Sowinska-Przepiera E, Poblocki J, Syrenicz J, Zdziarska B, et al. Case report: rare case of infiltration of small lymphocytic B-cell lymphoma in the thyroid gland of female patient with B-cell chronic lymphocytic leukemia (CLL-B/SLL-B). Thyroid Res. 2013;6:1.
- Bocian A, Kopczynski J, Rieske P, Piaskowski S, Sluszniak J, Kupnicka D, et al. Simultaneous occurrence of medullary and papillary carcinomas of the thyroid gland with metastases of papillary carcinoma to the cervical lymph nodes and the coinciding small B-cell lymphocytic lymphoma of the lymph nodes--a case report. Pol J Pathol. 2004;55:23-30.
- Reid-Nicholson M, Moreira A, Ramalingam P. Cytologic features of mixed papillary carcinoma and chronic lymphocytic leukemia/small lymphocytic lymphoma of the thyroid gland. Diagn Cytopathol. 2008;36:813-7.
- Shin J, Chute D, Milas M, Mitchell J, Siperstein A, Berber E. A rare case of chronic lymphocytic leukemia/small lymphocytic lymphoma presenting in the thyroid gland. Thyroid. 2010;20:1019-23.
- Trumper L, Matthaei-Maurer DU, Knauf W, Moller P. Centroblastic lymphoma of the thyroid supervening long-lasting chronic lymphocytic leukemia (B-CLL) demonstration of biclonality by immunohistochemical and gene rearrangement analysis. Klin Wochenschr. 1988;66:736-42.
 Contributed by Rebecca Leeman-Neill, MD, PhD and Walid Khalbuss, MD, PhD
Contributed by Rebecca Leeman-Neill, MD, PhD and Walid Khalbuss, MD, PhD






![]() Contributed by Rebecca Leeman-Neill, MD, PhD and Walid Khalbuss, MD, PhD
Contributed by Rebecca Leeman-Neill, MD, PhD and Walid Khalbuss, MD, PhD