FINAL DIAGNOSES
Thin Prep Cervical Screening Test:
This case illustrates the significance of endometrial cells in symptomatic postmenopausal women. In the Bethesda System for Reporting Cervical Cytology 1991, cytologically benign endometrial cells in a post menopausal woman were classified as an epithelial cell abnormality with the reasoning that the presence of endometrial cells in a postmenopausal woman not on hormonal therapy must be explained. They may be associated with vigorous sampling of the lower uterine segment, endometrial polyps, hormonal therapy, IUD, endometrial hyperplasia, or endometrial carcinoma.[1] However according to the Bethesda System for Reporting Cervical Cytology 2001, these cells are no longer classified as an epithelial cell abnormality but as other, endometrial cells in a woman ≥40 years of age. This was based on arguments that an individual's risk factors for endometrial carcinoma are often unclear, inaccurate, or unknown to the laboratory (symptoms, menstrual history, hormone therapy, menopausal status) and the prevailing view that cervical cytology is primarily a screening test for squamous lesions. It is unreliable for the detection of endometrial lesions and should not be relied on to detect suspected endometrial abnormalities.[2] At Magee, we still classify endometrial cells in postmenopausal women as an epithelial cell abnormality to alert the clinician to this finding for which guidelines require clinical follow-up. In this particular cytology case, one could argue that atypical glandular cells should have been reported. Fortunately due to the Magee reporting method, the patient had subsequent diagnostic procedures.
Kapali, M et al reported on patients with normal endometrial cells on Pap test and the subsequent tissue sampling. Six patients had significant pathology, out of which four were postmenopausal. Three of the four postmenopausal women were asymptomatic. The two premenopausal patients presented with bleeding. [3] Siebers, AG et al found that the finding of normal endometrial cells on cytology in postmenopausal asymptomatic women increased the (pre) cancerous endometrial lesions from 0.2% to 6.5%. [4] Li, Z et al found endometrial neoplastic lesions in these patients increased significantly with age with 2.7% in the age range of 50-54 years old, 2.8% in the age range of 55-59 years old, and 10.0% in more than 60 years old. [5] Another study reported significant endometrial pathology in 11.6% of postmenopausal patients (14 cases) with normal endometrial cells found on cytology. Of the 14 cases, only three were symptomatic. [6] These studies provide evidence that symptomatic premenopausal women and all postmenopausal women with benign endometrial cells on Pap test should have sampling which can impact patient care.
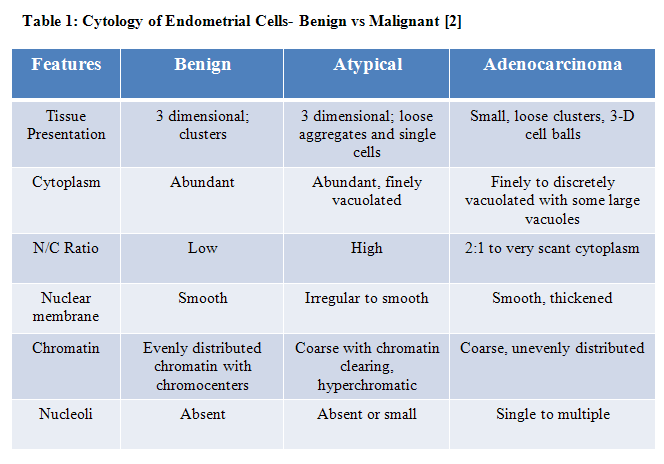
According to the 2006 Consensus guidelines, benign appearing endometrial cells in woman 40 years and older are found in 0.5 - 1.8% of cervical cytology specimens. According to the 2006 and 2012 Consensus guidelines, the BII recommendation is endometrial assessment regardless of symptoms in postmenopausal women. BII recommendation is characterized as "moderate evidence for efficacy or only limited clinical benefit supports recommendation for use and evidence from at least one clinical trial without randomization, from cohort or case-controlled analytic studies (preferably from more than one center), or from multiple time-series, or dramatic results from uncontrolled experiments". [7 and 8] It is important to differentiate benign endometrial cells from atypical and adenocarcinoma (Table 1).

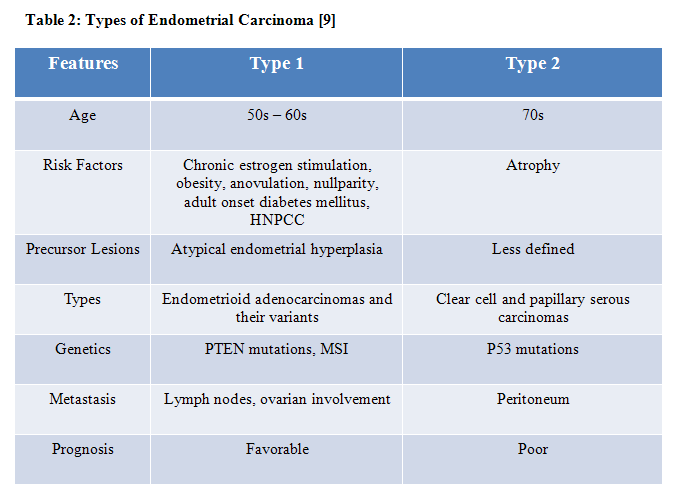
Endometrial adenocarcinoma is the most common cancer of the female genital tract and usually occurs in postmenopausal women. The average age is 60 years old and over 80% present with bleeding. Approximately ten percent or less occurs in women under 40 years old. Endometrial adenocarcinomas are divided into type 1 and 2 (Table 2). Type 1 endometrial carcinoma is present in 40-70% of women with Hereditary Nonpolyposis Colonic Cancer Syndrome (HNPCC); however, they only represent 2% of all endometrial carcinomas. MSH6 is most likely affected in Lynch syndrome patients. [9]
Our case was an endometrioid adenocarcinoma which is graded by the International Federation of Gynecology and Obstetrics (FIGO) system. Grading is based on solid growth, with grade 1 less than five percent, grade 2 with 5- 50% and grade 3 over 50% solid growth. The tumor can be upgraded due to nuclear enlargement or atypia. [9]
Endometrioid adenocarcinomas represent 90 % of endometrial carcinomas. Microscopically, endometrioid adenocarcinomas form endometrioid tubules at least focally. Most express pan-cytokeratins, CK7, and vimentin. [10] ER and PR are positive in most FIGO grade 1 and 2 and 50% of FIGO grade 3 adenocarcinomas. Only a minority of FIGO grade 2 and 3are diffusely positive (more than 75% of cells) for p53. P16 staining is dependent on grade; occasional grades 1 and 2 may stain scattered tumor cells while grade 3 can have diffuse and strong staining. Carcinoembryonic antigen (CEA) is expressed rarely and when expressed, it stains the apical membranes. CEA is more likely to be expressed in endocervical carcinomas.[10] Endometrial adenocarcinomas with mucinous differentiation can express CDX2 and have more diffuse staining for CEA. DNA mismatch repair proteins are lost in 33% by immunohistochemical staining method. Most sporadic non-familial cases this is due to hypermethylation of the MLH1 promoter.[10]
REFERENCES
![]() Contributed by Lisa Radkay, MD and R. Marshall Austin, MD
Contributed by Lisa Radkay, MD and R. Marshall Austin, MD