![]() Contributed by Stephen Hastings, MD and Mohamed A. Virji, MD, PhD
Contributed by Stephen Hastings, MD and Mohamed A. Virji, MD, PhD
Chief Complaint
I feel awful.
HPI
The patient is a 22 year old female with no significant past medical history. Four months prior to admission, she started to notice weight gain, fatigue, facial swelling, increased thirst, and increased frequency of urination. She was seen at an outside institution where she was found to have hypokalemia and an elevated morning cortisol of 54 µg/dL. Additional workup revealed an elevated urinary free cortisol (greater than 1000 µg/day) and an elevated morning cortisol (56 µg/dL) after a 1 mg dexamethasone suppression test. Abdominal CT revealed a liver mass 6 cm in greatest dimension that was thought to be a hemangioma. She was started on amiloride and potassium and referred to endocrinology at UPMC. When she presented at the clinic a few days later, she was found to be unstable and transferred to the Emergency Department, then subsequently admitted to the hospital.
Family History
Non contributory
Vital Signs
Temperature: 36.8 °C
Blood pressure: 132/72 mm Hg
Pulse: 166 per minute
Respiratory rate: 28 per minute
Physical Exam
Notable for central adiposity, Cushingoid facies, a large dorsal fat pad, hirsutism, striae, and proximal muscle weakness.
Initial Studies
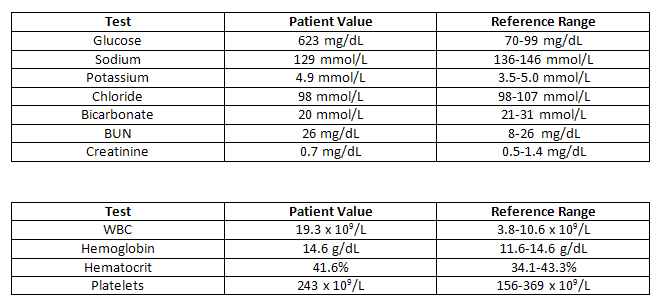
Interim Hospital Course
The patient was initially treated with IV fluids and insulin. The patient's pulse decreased to 110 per minute and her blood glucose improved. The patient also noted that she was feeling much better. Next, the following tests were performed:
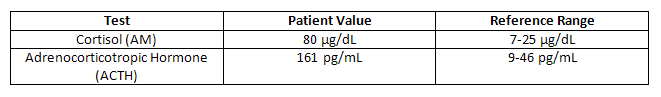
She had an MRI of the pituitary, which revealed an equivocal hypodense area on the left side, suggesting a possible microadenoma.
A high dose (8mg) dexamethasone suppression test was performed and cortisol was found to be 116 µg/dL in the morning, indicating non-suppressible cortisol production.
Imaging Studies
MRI Abdomen
A large (6.0x5.4x4.0cm) enhancing liver mass (Image 1) and bilateral adrenal hyperplasia.
Interim Hospital Course
On the second day, she developed emesis with a coffee ground appearance and melena. Her hemoglobin dropped from 14.6 g/dL to 5.1 g/dL. She underwent emergent esophagogastroduodenoscopy (EGD) to evaluate the source of the bleeding and was found to have multiple non-bleeding cratered duodenal ulcers (Image 2).
The patient required multiple blood transfusions, but was eventually stabilized. Additional workup revealed the following results:
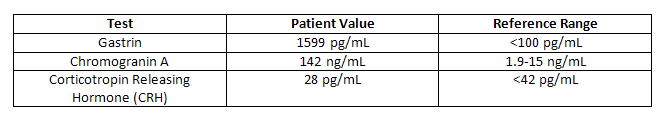
Endoscopic Ultrasound
Mass in the pancreatic body measuring 13 mm by 13 mm in maximal cross-sectional diameter with the endoscopic appearance of a neuroendocrine tumor (Image 3). The lesion was biopsied.
Cytology Report for the Biopsy
Diagnosis: Neuroendocrine Neoplasm
Comment: The specimen is focally cellular and comprised of intermediate to large sized cells with high N:C ratio and granular chromatin pattern. A panel of immunohistochemical studies performed on the cellblock material reveals the following results with regard to the neoplastic process:
Synaptophysin: Positive
ACTH: Positive in rare isolated cells
AE1/AE3: Positive
CEA-m: Negative
Octreotide Scan
1. 1.4x1.7cm pancreatic body lesion demonstrating increased radiotracer uptake and mild enhancement on the diagnostic CT compatible with neuroendocrine tumor
2. Heterogeneously enhancing hepatic dome mass with increased radiotracer uptake compatible with metastatic lesion
CRH Stimulation Test
Pre-stimulation: ACTH 108 pg/mL
Post-stimulation: ACTH 148 pg/mL (37% increase)
Pre-stimulation: Cortisol 45 ug/dL
Post-stimulation: Cortisol 68 ug/dL (51% increase)
Inferior Petrosal Sinus Sampling (IPSS)