![]() Contributed by Eumenia Castro, MD, PhD and Lydia Contis, MD
Contributed by Eumenia Castro, MD, PhD and Lydia Contis, MD
CLINICAL HISTORY
The patient is a 10 year old female, who underwent liver transplantation at the age of 2 for Alagille syndrome-related end-stage liver disease. Prior to transplantation, she received 36 mg of thymoglobulin followed by 24 mg post transplant, and tacrolimus 2 mg twice daily. Her immediate post transplant course was complicated by a pulmonary thromboembolism and acute cellular rejection which were treated with corticosteroids and antibiotics. Approximately one year after transplant, the patient presented with flu-like symptoms that included fever, rhinorrhea, body aches and an EBV titer of 30 million copies/ml. She was admitted for ganciclovir and CytoGam administration with EBV surveillance. An abdominal CT scan demonstrated a liver lesion along with cervical and axillary adenopathy. A liver biopsy demonstrated a hepatic Epstein-Barr virus-associated smooth muscle tumor. A lymph node biopsy revealed a CD20 positive infectious mononucleosis-like post transplant lymphoproliferative disorder (PTLD). Immunosuppression was suspended, and she was treated with ganciclovir, CMV-IGIV and rituximab. Despite the reduction in immunosuppression, her liver lesions increased in size. Chemotherapy was felt to be of no additional benefit in treating the CD20 negative liver lesion. The liver lesions were monitored with scans She received 4 doses of rituximab with decrease in size of her lymph node PTLD. At the age of 8 she was no longer receiving immunosuppression and her liver masses remained stable in size by CT scan evaluation. At 10 years of age, she presented to the hospital with abdominal pain. A CBC demonstrated the following:
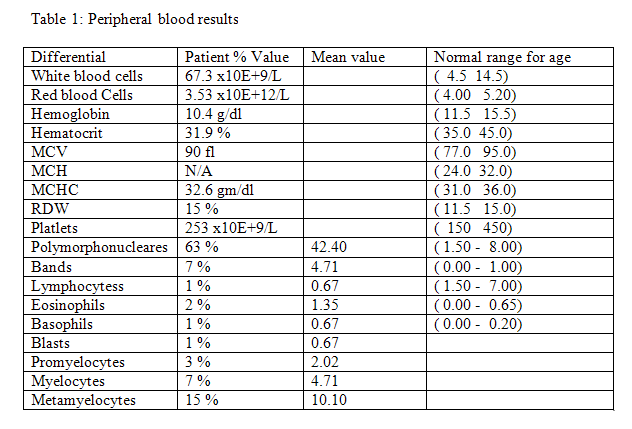
A bone marrow biopsy and aspirate were performed along with flow cytometry studies, cytogenetic and genotypic studies.
PATHOLOGY
The peripheral blood demonstrated a normochromic, normocytic anemia with a leukocytosis and myeloid left shift with 1% blasts (Figure 1). The bone marrow aspirate differential demonstrated a myeloid hyperplasia with a myeloid: erythroid ratio of 6.2:1 with 2.3% blasts by manual differential count of the aspirate (Table 2). The bone marrow aspirate was very cellular with increased myelocytes and metamyelocytes (Figure 1). The bone marrow biopsy was hypercellular for age. Megakaryocytes included few monolobate forms (Figure 3). Reticulin stain performed on the biopsy demonstrated mildly increased reticulin fibrosis (Figure 4). Bone marrow Flow cytometry studies performed on the bone marrow revealed 2% myeloblasts and no aberrant B or T-lymphoid populations. Conventional cytogenetic studies performed on the bone marrow demonstrated the t (9;22)(q34;q11.2) in all cells examined with no other additional abnormalities. FISH studies demonstrated that 196 (78.4%) of the cells were positive for a BCR/ABL fusion signal. FISH performed for del (5), EGR-1, del (7), trisomy 8, del (13q),and del(20q) were negative. Molecular analysis showed BCR-ABL fusion transcript with a normalized copy number of 67.8% by RT-PCR. The blood tests revealed a albumin of 4.1 g/dl (rv:3.4-5.2); total bilirubin of 0.3mg/dl (rv:0.0-1.2), direct bilirubin of < 0.1mg/dl (rv:0.0-0.3); alkaline phosphatase of 252u/l (rv:55-400); Alanine transaminase of 37 u/l (rv:7-54), aspartate aminotransferase of 29 u/l (rv:10-60) and total protein of 6.6g/dl (rv:6.4-8.2). EBV qPCR performed on the blood was negative.