
![]() Contributed by Kelly Garner, MD and Bruce Rabin, MD
Contributed by Kelly Garner, MD and Bruce Rabin, MD
PAST MEDICAL HISTORY
Patient is a 57 year old male with a medical history of hypertension who was evaluated by a rheumatologist in 1996 for sinus congestion and the presence of lung nodules. Initially, he refused a lung biopsy so he was placed on Cytoxan based on a presumptive diagnosis. From January 2009 till July 2010 he was taking Cytoxan and steroids for his pulmonary disease. At that time, he developed cytopenia and his medications were discontinued. He had one of his lung nodules biopsied which showed a granulomatous vasculitis with alveolar hemorrhage (see Figures 1 and 2). Due to the side effects of his past medicine regimen, he was going to be switched to a new oral agent but was not started on that medicine yet.
CLINICAL PRESENTATION
The patient presented to an outside hospital with left sided weakness and headache. A head and maxillofacial CT was obtained revealing a right basal ganglion hemorrhage (see Figure 3) and right maxillary mucosal thickening with bony erosion (see Figure 4). Subsequently, a brain MRA/MRI was obtained and revealed no vascular malformations. An angiogram was also performed and it did not reveal any signs of vasculitis. His blood pressure on arrival was 170/110.
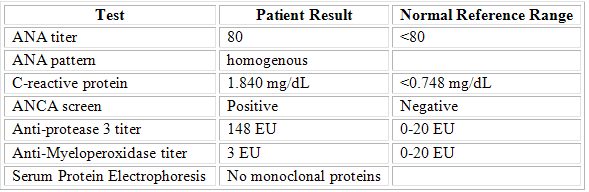
Because of his underlying pulmonary disease, rheumatology was consulted and a number of laboratory studies were ordered (Table 1). LABORATORY STUDIES
Table 1: Immunology studies revealing a positive ANCA Screen with positive Anti-PR3 titers
Figures 5a and 5b: ANCA Screen showed neutrophils with fine granular cytoplasmic staining (Ethanol-Fixed) [Ref: Autoimmune Cd.]