NEUROPATHOLOGICAL DIAGNOSIS:
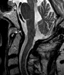
Primary Wegener's granulomatosis of the meninges.
DISCUSSION
Wegener's granulomatosis (WG) is a systemic disease of unknown origin characterized by necrotizing granulomatous vasculitis which involves primarily the respiratory tract and the kidney. Recently, the disease has been associated with the HLA-DPB1 locus (5). The onset of the disease is typically in the 4th decade of life. WG involves the nervous system in 20-54% of cases, predominantly as mononeuritis multiplex, while manifestation in the central nervous system (CNS) is less common (2% - 8%) (6). Primary manifestation in the nervous system is rare. Several case reports demonstrated patients suffering from palsies of multiple cranial nerves without pulmonary manifestations (3,9). Atypical cases of WG presented as ischemic stroke (10) as subarachnoid hemorrhage (2) or pituitary disease (9). In one patient a Wegener's lesion formed around the cervical spinal cord similarly to the case presented here (7). This patient, however, had elevated c-ANCA which resolved after high dose corticosteroid therapy. A number of reports demonstrated secondary spread of WG to the meninges. In these cases inflammatory thickening and fibrosis of the dura mater is usually associated with headaches, whereas cranial nerve lesions, cerebellar symptoms or epileptic seizures occur only rarely (1,4,7). In addition, a case of diffuse involvement of the meninges from Wegener's granulomatosis followed by chronic aseptic meningitis with communicating hydrocephalus and papillary edema was reported (8). Differential diagnosis in the case presented here included tuberculosis which was excluded microbiologically and sarcoidosis for which the histology was not typical.
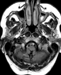
This is the first case of WG presenting as thickening of the dura in the area of the medulla oblongata, followed by cranial nerve palsy (VI and XII), ataxia, headache, personality changes and hydrocephalus.
In the woman presented here, it is noteworthy that serological tests for p- and c-ANCA, ANA, DNA, ENA were negative over the complete observation period of 1.5 years. The improvement of neurological symptoms and complete regression of the lesion in MRI 1.5 years after surgery (Figures 11, 12) after low dose medication with prednisolone (10 mg p.d.), however, support the histological diagnosis.
REFERENCES
![]() Contributed by Malgorzata Kolodziej, Ludwig Benes, Christopher Nimsky, Hans-Eckart Schaefer, Axel Pagenstecher
Contributed by Malgorzata Kolodziej, Ludwig Benes, Christopher Nimsky, Hans-Eckart Schaefer, Axel Pagenstecher