FINAL DIAGNOSIS
Refractory hypokalemia due to Ectopic ACTH
Based on the findings of hypokalemia, metabolic alkalosis, normal serum aldosterone, makedly elevated ACTH and cortisol levels and a history of widespread metastatic prostate carcinoma, the patient was diagnosed as refractory hypokalemia due to Ectopic ACTH production. The generation of hypokalemia, metabolic alkalosis and hypertension were likely the result of sustained activation of mineralocorticoid receptors by high levels of circulating cortisol.
His anemia and thrombocytopenia were thought to be secondary to marrow involvement by metastatic prostate carcinoma.
DISCUSSION
The various causes of hypercorticolism (Cushing's syndrome) are:
The serum electrolyte abnormalities are more common in ectopic ACTH syndrome than other forms of Cushing's syndrome.
Patients with ectopic ACTH syndrome have excessively high cortisol and elevated ACTH levels, hypokalemia, metabolic alkalosis and glucose intolerance. Only one of three patients with classic Cushing's syndrome has hypokalemia and metabolic alkalosis.
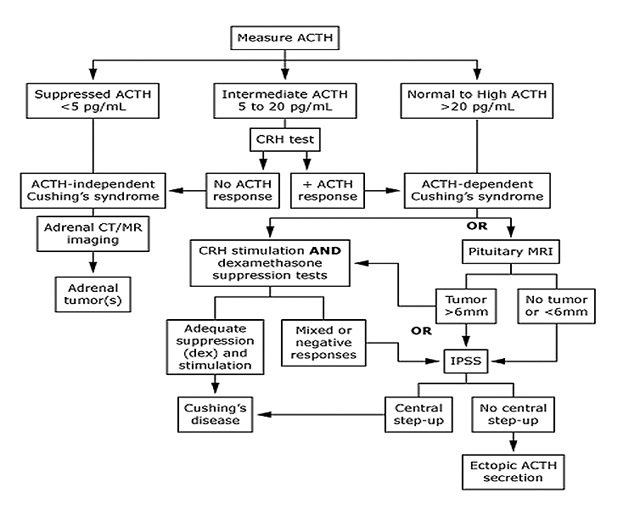
The approach to the diagnosis of various causes of hypercorticolism is shown below:

Etiology of Ectopic ACTH
Cushing's syndrome is caused by ectopic ACTH or corticotropin-releasing hormone (CRH) production in 10-20% of cases. The spectrum of non-pituitary tumors associated with ACTH production includes neuroendocrine tumors of respiratory and gastrointestinal tract, small cell lung cancer (SCLC), medullary thyroid carcinoma, and pheochromocytoma. Rarely prostatic tumors are associated with ectopic ACTH and/or CRH production.
Patient's with ectopic Cushing's syndrome secondary to carcinoma often lack the clinical manifestations associated with classic Cushing's syndrome. Presenting symptoms of ectopic ACTH can include rapid progressive weakness and weight loss.
Evidence suggests that ACTH levels correlate with the degree of metastasis or rapid tumor growth. Study by Coates et al in 18 tumors causing ectopic Cushing's syndrome found greatest ACTH levels in rapidly growing tumors with widespread metastasis.
Immunohistochemical staining of tumors for ACTH is insufficient evidence to rule out biosynthesis or activity of these hormones. It has been suggested that cells of highly malignant tumors causing Cushing's syndrome have a high secretion rate and do not store sufficient hormone for immunostaining.
Treatment of Ectopic ACTH
Surgical removal of the primary tumor is the treatment of choice for ectopic CS. However in as many as one third of patients surgery or radiation are not therapeutic options.
Medical interventions include potassium replacement and spironolactone and steroid biosynthesis inhibitors (ketoconazole, metyrapone, etomidate and mitotane).
Prognosis of patient's with ectopic ACTH is correlated with the histology of tumor and severity of hypercorticolism.
REFERENCES
![]() Contributed by Shveta Hooda MD and Mohamed A.Virji MD, PhD
Contributed by Shveta Hooda MD and Mohamed A.Virji MD, PhD