
Table 1: Characteristic clinical and laboratory findings in the different subtypes of autoimmune hepatitis.
FINAL DIAGNOSIS: AUTOIMMUNE HEPATITIS, TYPE I
DISCUSSION:
Clinical presentation
Autoimmune hepatitis (AIH) is a relatively uncommon disorder, which can lead to a potentially fatal liver dysfunction. Although AIH shows prominent predilection towards young women, it can affect males and females in all ages. The median age of diagnosis is 39 year in man and 49 years in women (1). In the majority of cases the disease follows an insidious, fluctuating course, and presents with non-specific clinical symptoms such as malaise, anorexia, jaundice and arthralgias. Especially in older patients, well established liver cirrhosis is often present at the time of diagnosis. In smaller group of cases the initial presentation is dominated by symptoms of acute or fulminant hepatitis (2).
Concomitant extrahepatic autoimmune disorders are found in approximately 13% of the AIH cases. These are most prevalent in the pediatric and in elderly patient groups (2). The list of rheumatic conditions frequently observed in AIH includes rheumatoid arthritis, Sj?gren's syndrome, autoimmune pericarditis, mononeuritis multiplex and systemic lupus erythematosus. Felty's syndrome, defined by the classical triad of neutropenia, splenomegaly, and rheumatoid arthritis can also be associated with AIH (3).
Autoimmune hepatitis is detected in 10-20% of patients with the Autoimmune-Endocrinopathy-Candidiasis-Ectodermal Dystrophy (APECED) syndrome. APECED is an autosomal recessive disorder, which is caused by the mutation of the immune response modulator gene AIRE (4).
Diagnostic criteria
Laboratory tests in AIH are usually consistent with a chronic active liver injury pattern. Marked elevation of liver transaminases and moderate hyperbilirubinemia are commonly detected in the active phase of the disease. Elevated serum IgG immunoglobulins as well as various circulating autoantibodies are characteristically seen in this immune response mediate process. Positive Coombs test in the AIH patients is often associated with autoimmune hemolytic anemia. False positive VDRL reactivity could also be occasionally detected (5).
Typical histological findings in AIH consist of prominent periportal lymphoplasmacytic infiltrate, interface hepatitis and lobular hepatocyte necrosis/dropout. In a long standing process a cirrhotic pattern can be present. While the picture of extensive hepatocyte dropout with mild inflammatory infiltrate is more suggestive of an adverse drug reaction mediated liver injury, negative infectious and drug history with a prominent plasma cell infiltrate favors AIH. Although the above described microscopic findings are not specific, in the appropriate clinical setting they strongly support the diagnosis of AIH. Moreover, liver biopsy continues to remain the "gold standard" for grading and staging disease activity (6).
The diagnosis of AIH primarily relies on the scoring system which was established by the International Autoimmune Hepatitis Group in 1993, and was revised in 1999 (7). This highly complex scoring system incorporates several clinical and histochemical criteria including sex, medication history, liver histology, transaminase levels and autoantibody titers. For definitive diagnosis of AIH a cumulative score greater than 15 in pre-treatment and greater than 17 in post-treatment patients is required. The scoring system is highly sensitive (89%) in detecting AIH patients. Since the introduction of the revised criteria, the system can better differentiate between cholestatic and hepatocytic disorders, and therefore its specificity (89.5%) has also significantly improved (8).
Subclassification and autoantibody patterns
Based on the differences in clinical, serological and genetic characteristics AIH can be divided into at least two major subtypes (TABLE 1). Type 1 disease is characterized by the presence of circulating anti smooth muscle antibodies (anti-SMA). However, positive anti-SMA serology in itself is not diagnostic of AIH, as it can be seen in other inflammatory liver diseases as well as in various rheumatoid conditions. The anti-SMA antibodies react with various cytoskeletal antigens, among which F-actin, especially in a polymerized form, is thought to be the most specific for AIH. While other anti-SMA antibodies are often detected in HBV and HCV hepatitis, they usually do not react with the F-actin epitopes. On rodent kidney sections indirect immunoflourescence staining of vessels, glomeruli, and tubules corresponds to the distribution of F-actin, and therefore it is indicative of Type 1 AIH. The serum level of F-actin antibodies can also be measured with ELISA based tests (9).

Table 1: Characteristic clinical and laboratory findings in the different subtypes of autoimmune hepatitis.
Three types of anti-liver-kidney microsomal (anti-LKM) antibodies have been described in inflammatory liver diseases. The anti-LKM-1 antibody is a serologic marker of Type 2 AIH (TABLE 2). The target of the anti-LKM-1 antibodies is the cytochrome 450 2D6 oxidase (CYP2D6), which can be localized to hepatocytes and to proximal renal tubular cells. Due to their similar staining patterns, anti-LKM antibodies can be occasionally confused with anti-mitochondrial antibodies (AMA) on indirect immunoflourescence stains. However, the anti-LKM-1 pattern lacks reactivity to distal renal tubules and to stomach parietal cells. Anti-LKM-3 antibodies are directed against the UGT1A microsomal glucuronosyltransferase, and can be only seen in 10% of Type 2 AIH patients (10).
Serum antibodies to nuclear antigens (ANA) are present in 70% of Type 1 AIH patients. Most frequently a homogenous, sometimes a speckled ANA pattern is seen. The antigens recognized by ANA are highly heterogeneous. ANA antibodies can be directed against single and double stranded DNA (ss-, ds-DNA), centromere (ACA), histone, lamin, and chromatin epitopes. The ANA distribution pattern and antigens detected in AIH are different from those seen in primary biliary cirrhosis (PBC), but can overlap with drug induced, alcoholic, or HCV hepatitis. Although non-specific, ANA represent an important diagnostic criterion of AIH, which is also incorporated into the AIH scoring system. Neither the ANA patterns nor the ANA titers however, have been shown to correlate with disease progression, therapeutic response or need for transplantation.
Anti-soluble liver antigen (anti-SLA) antibodies can be detected in 10-50% of Type 1 AIH patients. Anti-SLA antibodies are directed against the UGA repressor serine t-RNA cytoplasmic antigen (11). While in adults anti-SLA is specific for Type 1 AIH, in children it could be associated with either Type 1 or Type 2 disease. High anti-SLA antibody titers are seen in severe AIH (12). Whether the elevated anti-SLA levels actively contribute to hepatocyte death, or they are simply induced by the release of more intracellular antigens, still needs to be determined. In cases when serology for anti-SMA, ANA, and anti-LKM is negative anti-SLA can help to establish the diagnosis. Some consider positive anti-SLA serology the hallmark of Type 3 AIH, but this category is not recognized by the official classification systems.
Antibodies to liver cytosol type 1 antigen (anti-LC1) are found in over 30% of Type 2 AIH patients. These antibodies directed against the 58 kD formiminotransferase cyclodeaminase (FTCD) protein. Anti-LC1 shows significant correlation with disease activity and could be used as a marker of residual inflammation (12). Anti-asialoglycoprotein receptor (ASGPR) antibodies are observed in a myriad of hepatic disorders including PBC, viral and drug induced hepatitis. Anti-ASGPR antibody levels have also been reported to correlate with the inflammatory activity and therapeutic response (13).
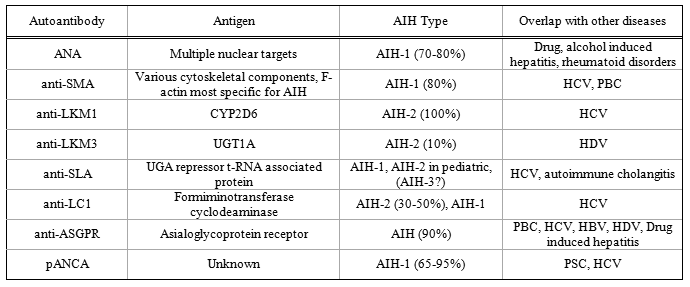
Table 2: Prevalence of commonly detected autoantibodies in autoimmune hepatitis. (ANA - antinuclear antibody, SMA - antismooth muscle antibody, LKM - liver-kidney microsomal antigen, SLA - soluble liver antigen, LC1 - liver cytosol type 1 antigen, ASGPR - asialoglycoprotein receptor, pANCA - perinuclear antineutrophil antibody, UGT1A - 1 uridine 5'-diphosphate glucuronosyltransferase, PBC - primary biliary cirrhosis, PSC - primary sclerosing cholangitis)
The hepatic "overlap syndromes" are entities where histological and serological parameters show an intermediate distribution between AIH and primary biliary cirrhosis (PBC) or primary sclerosing cholangitis (PSC) (5). These syndromes present with synchronous hepatocytic and cholangiocytic dysfunction. Not unusual that one component of the overlap syndrome precedes the other, and the second disorder only becomes apparent in a late stage of the disease. The AIH-PBC overlap is characterized by elevated transaminases, cholestatic markers as well as by increased IgG and IgM serum levels. On microscopic examination there is apparent interface hepatitis and bile duct destruction. The serological tests are positive for both anti-SMA and anti-mitochondrial antibodies (AMA). Positive serum ANA in these patients can be associated with either AIH of PBC specific antibodies (8).
Overlap between AIH and PSC is found in approximately 10% of adult patients diagnosed with either condition, however it is more frequent in children. The prevalence of PSC in pediatric AIH is 6-8 %. Interestingly, high immunoglobulin levels and interface hepatitis are observed in up to one third of children with PSC. The autoimmune serology profile in the AIH-PSC overlap syndromes is similar to AIH (5).
Pathogenesis models
Over three quarters of AIH cases arise in patients with a well characterized genetic predisposition. In the Caucasian population presence of the HLA-DRB1*0301 and HLA-DRB1*0401 haplotypes confers a significantly increased risk of AIH. Moreover, the DRB1*0301 allele was found to be associated with earlier disease onset and higher frequency of treatment failure (14). Another allele, HLADRB1*1301 could be detected in 45% of North-American AIH patients, who were negative for both DR3 and DR4 (15). On the other hand, patients with an HLA-B8 allele tend to have a more aggressive disease course. In the Italian population HLA-B8-DR3-DQ2, in Japan HLA-DRB1*0405 are the most frequent AIH associated haplotypes (12).
The most popular models of AIH pathogenesis are built around the "molecular mimicry" hypothesis. Molecular mimicry describes the phenomena when antibodies directed against foreign antigens cross-react with self-antigens resulting in an autoimmune disorder. The structural similarities found between the epitopes of CYP2D6 and herpes simplex virus as well as between FTCD and herpes virus type 6 indicate that antigen cross-reactions may have a significant role in AIH pathogenesis. Interestingly, anti-LKM antibodies seen in Type 2 AIH are also found in HCV infection, and sometimes anti-LKM-1 positive patients cross-react with the NS3 and NS5a viral proteins (16). Another intriguing evidence in favor of the "molecular mimicry hypothesis is that immunization of mice with the human CYP2D6 and FTCD alloantigens can be successfully used to generate murine models of AIH (17).
Activated self-reactive lymphocytes are more likely to be trapped in liver sinusoids than in other organs, as liver sinusoidal cells express various cell adhesion molecules including ICAM-1 and VCAM-1 capable binding to leukocytes surface proteins. The liver infiltrating lymphocyte population in AIH is predominantly composed of CD4+ Th1 cells, suggesting that self-antigen recognizing T-cells could contribute to AIH pathogenesis. Autoreactive CD8+ T-cells are also found in AIH. They are able to recognize antigens on the hepatocyte surface, and may trigger apoptosis through activation of the TNF- , Fas/FasL pathways. Finally, the immune mediated destruction of hepatocytes, either through soluble or cellular factors, may lead to unmasking of further intracellular autoantigens resulting in a self-enhancing cycle of events (18).
Treatment and prognosis:
The majority of AIH patients show excellent response to immunosuppressive therapy with corticosteroids. The preferred treatment for AIH is prednisone in combination with azathioprine. Long term control of AIH is achieved with administration of low dose corticosteroids and azathioprine either alone or in combination. Azathioprine is a genotoxic alkylating agent. Prolonged use of azathioprine is associated with increased risk of malignancy. The azathioprine doses used in AIH are typically lower than those used to treat rheumatoid arthritis or inflammatory bowel diseases, and usually do not exceed 150 mg daily. Still, because of the numerous adverse reactions associated with long term steroid and azathioprine therapy alternative treatment modalities are highly sought after. Mycophenolate mofetil, budesonide, rapamycin and 6-thioguanin nucleotides have demonstrated success as replacements to the conventional corticosteroid based protocols. Multiple recombinant immune response modifying agents are currently under development, and in the future they also could represent viable therapeutic alternatives (19).
Therapeutic success in AIH is marked by the disappearance of serum ANA and SMA antibodies, as well as by resolution of clinical and histological findings. In significant number of cases reversal of hepatic cirrhosis can also be observed (19). Survival rates of responders are similar to the healthy counterparts from the same population. In 10-20% of the cases however, AIH progresses into liver cirrhosis, eventually requiring liver transplantation. Interestingly, according to Al-Chalabi et al. men appear to have higher relapse rate and younger disease onset than females. Still, females are more likely to die from liver transplantation and have a significantly lower long-term survival rate (1). Older data show that without appropriate immunosuppressive therapy AIH has a very poor prognosis with 10-year survival rates as low as 10% (5).
Conclusions:
Following assessment of the clinical symptoms the patient's AIH score was calculated. The AIH score of 18 together with the positive anti-SMA serology substantiated the diagnosis of Type 1 AIH. Once diagnosis had been established immunosuppressive therapy with 10 mg prednisone and 50 mg azathioprine daily was initiated. The patient showed good initial response with normalization of liver function tests and improvement of clinical symptoms. However, a month into therapy she experienced an episode of relapse with sharp elevation of liver enzymes. Therefore, tapering doses of corticosteroids starting from 50 mg per day were administered, and the maintenance dose of azathioprine was increased to 75 mg. This brought the patient's symptoms under long term control.
In summary, autoimmune hepatitis is a relatively uncommon disorder associated with chronic hepatic inflammation. Occurring in patients with a well characterized genetic background, the diagnosis of AIH is greatly facilitated by the international AIH scoring system. Immunosuppressive corticosteroid therapy generally controls disease progression effectively.
REFERENCES:
![]() Contributed by Pal Kaposi-Novak, MD, PhD, Mordechai Rabinovitz, MD and Bruce Rabin MD, PhD
Contributed by Pal Kaposi-Novak, MD, PhD, Mordechai Rabinovitz, MD and Bruce Rabin MD, PhD