Final Diagnosis -- Atypical myxoid tumor of the vulva
FINAL DIAGNOSIS: ATYPICAL MYXOID TUMOR: FAVOR ATYPICAL MYXOID LEIOMYOMA OF THE VULVA
DISCUSSION:
The microscopic pattern of interlacing fascicles of spindle cells with areas of epithelioid cells with prominent eosinophilic cytoplasm is most suggestive of a mixed spindled and epithelioid leiomyoma. The immunohistochemical staining profile shows some smooth muscle differentiation. The areas of cellular atypia with low mitotic rate are characteristic of an atypical leiomyoma and the prominent myxoid matrix has been described in vulvar smooth muscle tumors.
A myxoid leiomyoma is a rare type of smooth muscle tumor of the vulva that presents in reproductive age females. Myxoid leiomyomata were first described in 1979 by Tavassoli and Norris who initially reported 10 cases of leiomyomata with myxoid change, seven of whom were pregnant.1 In the current literature there have been less than twenty-five case reports of benign/atypical smooth muscle tumors of the vulva exhibiting myxoid change (Table). Besides this case, there has been only one other atypical myxoid leiomyoma of the vulva described in the literature.2
Smooth muscle tumors with myxoid change are rare tumors but are more frequently observed in the vulva than elsewhere in the body.3 Unlike other smooth muscle tumors of the female genital tract, those of the vulva are prone to myxoid change, creating a diagnostic dilemma with other soft tissue tumors such as aggressive angiomyxoma, angiomyofibroblastoma, and inflammatory myofibroblastic tumor. Accurate classification of these tumors is important for proper surgical management and clinical follow-up.
Much of the histological confusion in distinguishing vulvar tumors is based on the presence of myxoid stroma seen in these neoplasms. Cases in which a myxoid leiomyoma was initially diagnosed as an aggressive angiomyxoma on biopsy have occurred both at our institution along with a case report in the literature.3
Aggressive angiomyxoma of the vulva displays an extensive, uniform myxoid stroma with a bland, paucicellular population of spindle-stellate cells.4 It typically has an infiltrative border and show immunohistochemical distinction in their propensity to stain for CD34.5
Angiomyofibroblastoma is another rare tumor of the vulva that is well circumscribed, displaying similar histologic features of a myxoid leiomyoma with a myxoid stroma in the background of plump epithelioid to spindle cells with minimal to rare cytologic atypia. However, angiomyofibroblastoma displays distinctive hypo and hypercellular areas with a classic perivascular accentuation of the stromal cells, which is not seen in a myxoid leiomyoma. While it shares a similar immunohistochemical profile staining for desmin, vimentin, and frequent ER/PR positivity, it is typically smooth muscle actin negative.6,7,8
Inflammatory myofibroblastic tumor is another entity that these tumors can be confused with, which displays a myxoid stroma with spindle cells admixed with an inflammatory infiltrate. As seen both at our institution and in a case report of a myxoid leiomyoma of the vulva,9 smooth muscle tumors of the vulva may display foci of inflammatory infiltrates with eosinophils and foreign body giant cell reactions. However, in contrast to an inflammatory myofibroblastic tumor, a myxoid leiomyoma will not demonstrate a marked lymphoplasmacytic infiltrate nor will display an irregular, sparse arrangement of spindle cells with granulation tissue type blood vessels.4 Immunohistochemical staining of spindle cells in an inflammatory myofibroblastic tumor may be smooth muscle actin and desmin positive, but the distinctive histologic picture of an inflammatory infiltrate rich in plasma cells intermixed in a myxoid stroma diagnostic. It has been suggested that the foreign body giant cell reaction seen in a myxoid leiomyoma is likely from the myxoid material.9
Once a classification of smooth muscle origin is made, determining the malignant potential creates another diagnostic dilemma. The classification of benign, atypical, and malignant smooth muscle tumors of the vulva is a difficult task given their varied morphologies of spindle cell, epithelioid, and myxoid change. Distinguishing an atypical myxoid leiomyoma of the vulva from a myxoid leiomyosarcoma is based on criteria of size, mitotic count, tumor border configuration, and degree of atypia. Given the rare occurrence of an atypical myxoid leiomyoma, a practicing pathologist may erroneously use non-specific classifications based on uterine smooth muscle tumors (tumor necrosis, hemorrhage).10
Tavassoli and Norris first described three criteria for malignancy in a vulvar smooth muscle tumor: 1) size greater than 5 cm, 2) an infiltrative tumor contour, and 3) mitotic index ≥ 5 mitosis per 10 high power field (hpf). Displaying all three indicators was predictive of a leiomyosarcoma, while displaying only two was predictive of a "low grade" sarcoma.1 However, in 1996 in a case series review, Nielsen et al. revised the criteria for classifying benign, atypical, and malignant smooth muscle tumors of the vulva to include a fourth criteria of moderate to severe atypia.2 According to the Nielsen classification, a benign leiomyoma vulva has one of four criteria (1/4), an atypical leiomyoma has two of the four (2/4) criteria, while a leiomyosarcoma has three or four (3-4/4) criteria. Applying Nielsen's criteria, our case would be considered an atypical leiomyoma based on its original described size of 7 cm and severe cytologic atypia. Treatment of these tumors is conservative with wide local excision with negative margins. These tumors are thought to locally recur if not fully excised with negative margins.
In summary, an atypical myxoid leiomyoma of the vulva is a difficult tumor to diagnose given its overlapping histological appearance to other soft tissue tumors of the vulva. Given its rarity, it is important for the clinician to be aware of this entity that often masquerades as a Bartholin gland cyst or abscess, which may continue to recur if not completely excised, despite its benign natural history. In addition, once a smooth muscle origin is established, classifying the malignant potential of these neoplasms can cause confusion. The classic features of malignancy seen in smooth muscle tumors of the female genital tract are less prognostic in vulvar smooth muscle tumors (i.e. hemorrhage and tumor cell necrosis). In addition, an atypical myxoid leiomyoma is a rare variant that can only be diagnosed with strict adherence to established criteria of malignancy set forth for these smooth muscle tumors of the vulva.
Myxoid smooth muscle tumors of the vulva
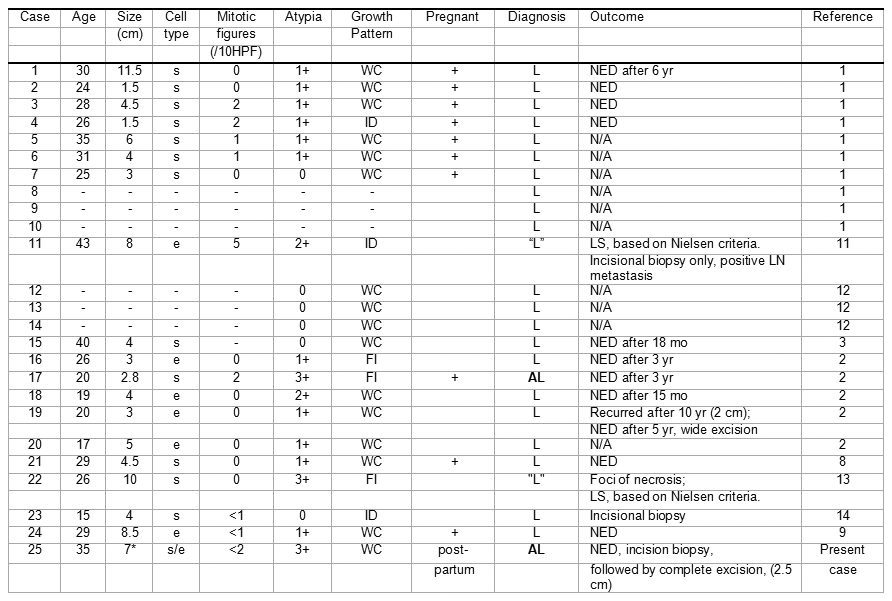
Cell types: s, spindled; e, epithelioid. Atypia: 1+ mild; 2+ moderate; 3+ severe. Tumor border growth pattern: WC, well circumscribed; ID, indeterminate; FI, focally infiltrative. Pregnant at the time of diagnosis: +. L, typical leiomyoma; AL, atypical leiomyoma; LS, leiomyosarcoma. NED=No evidence of disease. N/A=Not available. LN=Lymph node. *Original mass measurement; follow-up complete excisional mass measurement was 2.5 cm in greatest dimension.
REFERENCES:
- Tavassoli FA and Norris HJ. Smooth muscle tumors of the vulva. Obstet Gynecol. 1979;53:213-217.
- Nielsen GP, Rosenberg AE, Koerner SF, et al. Smooth-muscle tumors of the vulva: a clinicopathological study of 25 cases and review of the literature. Am J Surg Pathol. 1996;20:779-793.
- Nemoto T, Shinoda M, Komatsuzaki K, et al. Myxoid leiomyoma of the vulva mimicking aggressive angiomyxoma. Pathology International. 1994;44:454-459.
- Shea CR, Stevens A, Dalziel, KL, et al. The vulva: cysts, neoplasms and related lesions. In: Robboy, Anderson, and Russell eds. Pathology of the Female Genital Tract. Edinburgh: Churchill Livingstone; 2002:62-63.
- Fetsch JF, Laskin WB, Lefkowitz M, et al. Aggressive angiomyxoma: a clinicopathologic study of 29 female patients. Cancer. 1996;78:79-90.
- Nielsen GP and Young RH. Mesenchymal tumors and tumor-like lesions of the female genital tract: a selective review with emphasis on recently described entities. Int J Gynecol Pathol. 2001;20:105-127.
- Weiss and Enzinger. Benign soft tissue tumors and pseudotumors of the miscellaneous type. In: Enzinger and Weiss eds. Soft tissue tumors. St. Louis, MO: Mosby Inc; 1982:1444-1452.
- Kajiwara H, Yasuda M, Yahata G, et al. Myxoid leiomyoma of the vulva: a case report. Tokai J Exp Clin Med. 2002;27:57-64.
- Zhou J, Ha BK, Schubeck D, et al. Myxoid epithelioid leiomyoma of the vulva: A case report. Gyn Oncol. 2006;103:342-345.
- Zaloudek C and Hendrickson MR. Mesenchymal tumors of the uterus. In: Kurman, RJ, ed. Blaustein's Pathology of the Female Genital Tract. New York, NY: Springer-Verlag New York Inc; 2002:570-574.
- Chen KTK, Hafez R, and Gilbert EF. Myxoid variant of epithelioid smooth muscle tumor. Am J Clin Pathol. 1980;74:350-353.
- Newman PL and Fletcher CD. Smooth muscle tumors of the external genitalia: clinicopathologic analysis of a series. Histopathology. 1991;18(6):523-529.
- Topolovec Z, Mrcela M, Milojkovic M, et al. Pleomorphic vulvar leiomyoma with local invasive behavior. Coll Antropol. 2002;26(2):571-575.
- Azzam MA, Orrell JM, Vasey DP. Vulvar leiomyoma with myxoid hyaline stroma. J Obstet Gynaecol. 2004;24(8):936.
 Contributed by Jennifer Picarsic, MD and Mamatha Chivukula, MD, FASC, FCAP
Contributed by Jennifer Picarsic, MD and Mamatha Chivukula, MD, FASC, FCAP




