
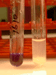

FINAL DIAGNOSIS:
Listeria Monocytogenes brain abscess, sensitive to Ampicillin and Trimethoprim/Sulfa.
DISCUSSION:
Microbiology and Pathogenesis:
Listeria monocytogenes is the only Listeria species that infects humans. It is an aerobic and facultatively anaerobic, motile, beta hemolytic, non-spore-forming, short, gram-positive rod that exhibits characteristic tumbling motility by light microscopy. Can occur in short chains or may resemble pneumococci or diphtheroids. It also can be gram variable and confused with Hemophiles species.
Listeria produces a characteristic appearance on blood agar with small zones of clear beta-hemolysis around each colony. Listeria is capable of slow growth at refrigeration temperatures (4°to 10°C).
Listeria is a facultative intracellular bacterium. It is catalase positive, fermentative producing acid from glucose. It lacks H2S production and grows in the presence of 40% bile and hydrolyzes esculin (Fig. 12). It shows positive hippurate hydrolysis (Fig. 13) and CAMP tests (Fig. 14). Most Listeria infections in adults are thought to result from oral ingestion and subsequent intestinal mucosal penetration and systemic infection.
Immunity to Listeria relies mainly on T-cell lymphokine activation of macrophages, which clear Listeria from the blood. Interleukin (IL)-18 appears to play a role in protection against Listeria by enhancing bacterial clearance.
Listeria can initially enter cells by a mechanism that may involve binding of a bacterial protein (internalin) to E-cadherin (CDH1) on the host cell. The organism then uses a unique mechanism of spreading from cell-to-cell, without exposing itself to an extracellular environment. It accomplishes this by subverting the actin-based cellular contractile mechanism; propulsion within the cytoplasm of infected host cells and cell-to-cell spread are thought to be driven by actin polymerization at the bacterial cell surface and the formation of a comet tail. Both protein components in the host cell cytoplasm (particularly profilin, a host actin monomer-binding protein) and a bacterial surface protein (called ActA) are required for actin assembly by Listeria.
The primary habitat of Listeria is the soil and decaying vegetable matter. It also can be found in water, sewage, and as a part of the fecal flora of a wide variety of animals.
Listeria has a predilection for the placenta and central nervous system. How this occurs is not well understood. Listeria crosses the placenta during maternal bacteremia and infects the fetus.
Epidemiology and predisposing factors:
In the United States, the estimated annual incidence of Listeria meningitis is 9.7 cases per 100,000 people.
Among foodborne infections in the United States, Listeria has the second highest mortality rate (approximately 20 percent compared to 39 percent with Vibrio vulnificus) and accounts for approximately 28 percent of all deaths from foodborne infection (ref. 4). Listeriosis is more often a sporadic illness than an illness that occurs in outbreaks.
Most systemic, invasive listerial infections occur in individuals with one or more predisposing conditions. These include pregnancy, corticosteroid therapy, other immunocompromised hosts, and age. Corticosteroid therapy is the most important predisposing factor in nonpregnant patients. Other immunosuppressive medications, organ transplantation and collagen vascular diseases are risk factors for Listeria infection. Listeria is the most common cause of bacterial meningitis in patients with underlying neoplastic disease, especially lymphoma, in organ transplant recipients, and in those receiving corticosteroids for any reason. Pregnant women, especially in the third trimester, are particularly susceptible to Listeria and account for up to one-third of reported cases. Listeria infection in pregnant women can lead to fetal death, premature birth, or infected newborns.
Clinical Manifestations and Diagnosis:
Clinical manifestations include meningitis, meningoencephalitis, or bacteremia in immunosuppressed patients, individuals at the extremes of age including neonates and the elderly and pregnant women. However, Listeria is also a cause of self-limited febrile gastroenteritis in normal hosts who ingest high numbers of organisms. The incubation period ranges from 6 hours to 90 days.
A nonspecific flu-like illness with fever and chills is the most common presentation of Listeriosis in pregnant women and CNS invasion is uncommon. Listerial infection in pregnant women can lead to fetal death, premature birth, or infected newborns.
Sepsis of unknown origin typically presents with fever and chills, primarily in patients who are immunocompromised or elderly. The diagnosis is established by blood cultures.
The most common central nervous system manifestation of listerial infection is meningoencephalitis. Cerebritis, which infrequently progresses to brain abscess, and rhombencephalitis (brain stem encephalitis) are less common.
Listeria meningoencephalitis most often occurs in neonates after three days of age and in immunocompromised and elderly adults. The clinical presentation of Listeria meningoencephalitis ranges from a mild illness with fever and mental status changes to a fulminant course with coma. Most adults have a subacute illness and 42 percent present without signs of meningeal irritation. Focal neurologic signs may be present, indicating an encephalitic component. These include cranial nerve abnormalities, ataxia, tremors, hemiplegia, and deafness. Seizures can occur and often begin later in the course. A subacute presentation with cranial nerve palsies, lymphocytic pleocytosis, elevated CSF protein and low glucose may mimic tuberculous or fungal meningitis. The CSF culture is usually positive for Listeria in such patients, but positive blood cultures rarely occur in the presence of negative CSF cultures.
Cerebritis results from direct hematogenous invasion of cerebral parenchyma, usually with little or no involvement of the meninges. However, the syndromes of meningitis and cerebritis can occur in the same patient. The clinical presentation of cerebritis ranges from fever and headache to hemiplegia, resembling a stroke. Progression to frank brain abscess is an uncommon complication. One case series reported five patients with listerial brain abscess, three of whom were cardiac transplant recipients. Focal neurologic symptoms were present in 87 percent of patients combining these five cases with a review of 34 previously published cases from 1966 to 2000.
Rhombencephalitis (brain stem encephalitis) is a rare manifestation of listerial infection.
Numerous focal manifestations of listeriosis have been described in case reports and small series. Most of these focal infections have no distinctive characteristics but tend to occur more commonly in immunocompromised patients.
There is no clinical way to separate Listeria infection from many other infectious diseases that can lead to fever and constitutional symptoms. As a result, the diagnosis can only be established by culture of the organism from the cerebrospinal fluid or blood. Patients with CNS manifestations other than meningitis have a higher rate of positive blood cultures than CNS cultures. CSF analysis reveals a pleocytosis that is typically associated with a moderate elevation in protein concentration and may be associated with a low glucose concentration. Listerial infection is the one cause of bacterial (nontuberculous) meningitis in which a substantial number of lymphocytes (>25 percent) is found in the CSF. Gram's stain is positive in only about one-third of patients and the organisms may resemble other species. The CSF analysis may be normal or show only mild abnormalities in patients with rhombencephalitis. Magnetic resonance imaging (MRI) is more sensitive than CT scan for the detection of Listeria lesions in the cerebellum, brain stem and cortex. High-signal lesions on T2-weighted images and enhancing lesions on T1-weighted images after the administration of intravenous contrast are seen in the cerebral parenchyma.
Molecular approaches to the identification of Listeria species have been developed. A highly sensitive and specific chemiluminescent DNA probe assay and spectrophotometric DNA probe assay are also available for rapid identification of L. monocytogenes form colonies grown on primary isolation media.
Treatment:
Listeria is sensitive to antimicrobial therapy and resistance to the most commonly used drugs appears to be rare. Ampicillin or Penicillin G are the drugs of choice. The dose and duration vary according to age.
However, these antibiotics demonstrate delayed in vitro bactericidal activity at concentrations attainable in the CSF. As a result, the bactericidal agent gentamicin is often added to achieve synergy for listerial CNS infections, endocarditis, and infections in immunocompromised patients. Penicillin-allergic patients can be skin tested and desensitized if necessary or treated with trimethoprim-sulfamethoxazole. An alternative is meropenem.
All patients with invasive listerial infection should be treated with antibiotics, since much higher mortality rates have been reported in untreated patients. Early diagnosis and initiation of appropriate antibiotic therapy are important.
Regimens without aminoglycosides may be preferable for patients who have impaired renal function or are taking other nephrotoxic drugs, such as cyclosporine. The response to therapy is monitored clinically and with.
Prognosis:
Patients with no underlying disease generally do well. In comparison, the mortality rate is high in patients with an underlying disease that predisposes to more serious infection (eg, malignancy, diabetes mellitus, or renal transplantation). CNS infection in immunocompromised patients carries a particularly high mortality. In addition, survivors of cerebritis (particularly cerebral abscess) or rhombencephalitis have a high rate of persistent neurologic sequelae.
Follow up:
Patient was treated with ampicillin drip for 6 to 8 weeks. Transesophageal and transthoracic echocardiography showed normal left ventricular size and function, trace tricuspid and mitral regurgitation with no vegetation. He was discharged to home in stable condition.
Recent MRI of brain shows significant improvement consistent with resolving abscess and post operative changes. There was a decrease in size of the lesion as well as decease in the peripheral enhancement pattern.
Acknowledgment: Geoffrey Murdoch, M.D., John Schaffer.
REFERENCES:
![]() Contributed by Amer Heider, M.D. and William Pasculle, SC.D.
Contributed by Amer Heider, M.D. and William Pasculle, SC.D.