
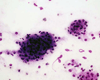


DIAGNOSIS: Supratentorial hemangioblastoma
DISCUSSION:
Supratentorial meningeal-based neoplasms are a frequent indication for intra-operative frozen sections. The differential diagnosis of such lesions includes meningioma, glioma and metastatic carcinoma, and rarely hemangioblastoma.
Hemangioblastomas of the central nervous system (CNS) are uncommon, capillary-rich neoplasms (1). They comprise approximately 1-3% of primary CNS tumors and 7-12% of primary posterior fossa tumors (2-4). The most common location is the cerebellum (83-95% of tumors): however, they can also arise in the pons, medulla (2%) and spinal cord (3-13%). Supratentorial lesions are rare (6, 7).
Hemangioblastomas may be sporadic or may be associated with Von Hippel-Lindau (VHL) disease (2, 8, 9). They occur particularly in the third to fifth decades, with some predilection for men (2, 4, 8, 9). VHL disease-associated cases occur in younger patients, and are often multiple (4, 10). Pial, pericytic, glial and endothelial origins have been proposed for these tumors (3, 11) but their histogenesis remains unclear (10, 12).
Radiologically, hemangioblastomas are highly vascular, contrast-enhancing lesions (6). Approximately 70% of infratentorial cases and 50% of supratentorial cases are cystic, and may show a contrast-enhancing mural nodule (2, 4, 8, 13).
Supratentorial hemangioblastomas were first described by Bielschowsky in 1902 (3, 14). They are rare and comprise 2-3% of all hemangioblastoma (1). Over 85% arise in the cerebral hemispheres (frontal, parietal and temporal lobes), 7% in the ventricles, 6% in the meninges and very rarely in sellar and parasellar locations (1, 3-5, 13, 15). The pathologic features of supratentorial hemangioblastoma are identical to those of the more common cerebellar tumors. Macroscopically, the tumors appear as well circumscribed, highly vascular nodules, often in the wall of a cyst, which may abut the meninges. The cut surface is spongy and hemorrhagic, with yellow areas corresponding to lipid-laden stromal cell-rich areas (6, 10). The histopathological features of hemangioblastomas are well-documented. They show variable cellularity and consist of two major components: vascular channels and intervascular tumor cells (also known as stromal or interstitial cells). (6, 8-10) The relative proportions of the two components vary: the stromal cells predominate in the cellular variant, while the vascular component predominates in the reticular variant (6, 10). Many of the vascular channels are small capillaries which may be round or compressed; larger feeding and draining vessels are also present (6). These channels are lined by bland, plump endothelial cells. The stromal cells, which represent the neoplastic component of the tumor, are rounded or polygonal in shape and possess pale, eosinophilic cytoplasm. The cytoplasm may appear foamy or clear due to the presence of intracytoplasmic lipid and/or glycogen (8-10, 12). The stromal cells may be interspersed with the vascular channels or may aggregate to form large cellular lobules; the latter is a feature of the cellular variant (6). The round or oval nuclei are centrally located within the cells. The nuclei may be uniform or may show significant pleomorphism, including karyomegaly, nuclear membrane irregularities and hyperchromasia (8, 9, 12). Mitoses are uncommon (Ki-67 index is less than 1) and the presence of occasional mitoses has no bearing on the behavior of the tumor. Cystic changes are common but necrosis is usually absent. Intratumoral hemorrhage may occur (6, 10). Mast cells are frequent and are readily seen using metachromatic stains such as toluidine blue. Foci of extramedullary hematopoiesis, reflecting erythropoietin production by the tumor, may be seen (6). Trichrome and reticulin stains show compartmentalization of the tumor by thin strands of connective tissue and highlight the complex arborizing vascular pattern (6, 9) Oil red O stain demonstrates cytoplasmic lipid in the stromal cells (9). The cyst wall around the tumor shows dense reactive gliosis, featuring prominent Rosenthal fibers (6)
The stromal cells are negative for vascular markers such as factor VIII-related antigen, Ulex europaeus antigen, CD34 and CD31. Although they are generally negative for glial fibrillary acidic protein (GFAP), occasional cases show focal GFAP positivity in the stromal cells. The stromal cells are negative for neurofilament but show positive staining with neuron-specific enolase (NSE) and other neuroendocrine markers. They are negative for epithelial markers such as epithelial membrane antigen (EMA) and cytokeratin (6, 10, 11). Some authors have reported immunohistochemical staining for alpha-1-antitrypsin, alpha-1-antichymotrypsin and/or S-100 in the stromal cells (11) Factor VIII-related antigen and other vascular markers are positive in the endothelial cells. Vimentin stains the stromal cells, but not the endothelial cells (9, 10). Ultrastructurally, the stromal cells are large and lack specific organelles or intercellular attachments. The electron-lucent cytoplasm contains variable numbers of glycogen particles and lipid droplets (6, 9, 10) Some cases have shown Weibel-Palade-like bodies and neurosecretory granule-like structures in the stromal cell cytoplasm (9, 10).
The recognition of hemangioblastoma on frozen sections is difficult due to its morphologic similarities with metastatic carcinoma and glioma, and is rendered even more challenging when the tumor is dural-based and occurs in a rare supratentorial location (where the entities in the differential diagnosis occur more commonly). These difficulties are compounded by the artifactual cytomorphologic changes in the tumor as a result of freezing (6, 8, 12). The vascular component becomes inconspicuous and the characteristic foamy nature of the stromal cell cytoplasm is often lost, (8, 12) as in our case. Also fibrillarity and nuclear pleomorphism are enhanced by freezing effect, leading to confusion with astrocytic neoplasms. Thus, definitive diagnosis of hemangioblastoma and differential diagnosis from its mimics based on frozen sections is fraught with difficulty (6, 12).
Cytologic evaluation of smears of fresh tumor tissue is superior to frozen section in the intraoperative diagnosis of hemangioblastoma and in its distinction from other tumors in the differential diagnosis (12). Smears have the dual advantages of requiring only minimal amounts of tissue and of providing excellent cytologic detail (which is often compromised in a frozen section).8 Smears of hemangioblastomas are quite cohesive, the tissue smearing as a few large clumps with little cellular dissociation from the clumps (8). Often, little cytologic detail can be gleaned from the thick centres of cell clumps, although a complex meshwork of capillaries and stromal cells may be focally apparent (8, 12). At the edges of the cell clumps, small, vaguely club-shaped clusters of stromal cells, sometimes associated with fusiform endothelial cells, extend outward. These cells possess pale, lace-like, granular or foamy cytoplasm, and contain oval or reniform, hyperchromatic nuclei with evenly distributed, speckled chromatin (8, 9, 11, 12). The cell borders are indistinct and somewhat frayed due to fragility of the cytoplasm. The characteristic cytoplasmic vacuolation of the stromal cells is best appreciated in air-dried, Diff-Quik-stained smears. As with frozen sections, this feature is lost in wet-fixed, hematoxylin & eosin-stained smears (12). Mild to moderate nuclear pleomorphism may be seen, but nucleoli are small or inconspicuous (8, 9, 11, 12) Hemosiderin is invariably present within the cell clumps (8). A few bare nuclei may be seen in the background, which contains numerous erythrocytes (8, 9, 11). Some groups of delicate, branching channels and bland spindle-shaped endothelial cells are seen, with fine, evenly distributed nuclear chromatin (9). The background comprises fresh blood and proteinaceous fluid, and fragments of cytoplasm and free vacuoles, a result of the marked cytoplasmic fragility of the stromal cell (12).
The main tumors that fall into the differential diagnosis of supratentorial hemangioblastoma are meningioma (particularly in the case of dural-based neoplasms), renal cell carcinoma and anaplastic astrocytoma (8,9)
In the past, the distinction between hemangioblastoma and meningioma relied on the absence or the presence (respectively) of a dural attachment (8,14). However, supratentorial hemangioblastomas with dural attachment are well documented; some of these cases arise predominantly from the dura, while others represent secondary involvement of the dura by intracerebral hemangioblastoma (8,13). EMA immunostaining can help distinguish the two on paraffin sections (meningioma being EMA-positive and hemangioblastoma being EMA-negative). However, the distinction at the time of frozen sections can be challenging, especially if scant tissue is available or there is significant freezing artefact. Smears can be very useful in the differential diagnosis. Smears of meningioma show small clusters of cells, often in a whorling pattern, (Fig. 3B) as well as numerous individual, dispersed cells (a feature not seen in hemangioblastoma) (Fig. 3A). Hemosiderin and nuclear grooves, which are seen in hemangioblastoma, are rare in meningioma, while calcifications are far more common in meningioma (8).
Histologically, hemangioblastoma may be difficult to distinguish from renal cell carcinoma. Both tumors are highly vascular and contain cells with pale cytoplasm. Both may show cells with nuclear grooves. Immunohistochemically, renal cell carcinomas stain positively for EMA while hemangioblastomas are EMA negative (8, 11). Cytoplasmic PAS-positive, diastase-resistant glycogen is far more common in renal cell carcinoma than in hemangioblastoma (9). Distinguishing these tumors on frozen section can be extremely difficult, and smears are helpful. Renal cell carcinoma shows cellular smears, often with a dirty, necrotic background. Cohesive three-dimensional clumps and sheets of cells and variable numbers of individual discohesive cells are present, (Fig 4A) the latter feature being uncommon in hemangioblastoma. The cells of well differentiated renal cell carcinoma often show distinct cytoplasmic borders (not seen in hemangioblastomas) and abundant eosinophilic, foamy or granular cytoplasm (8). The cells often show fewer cytoplasmic vacuoles than those of hemangioblastoma, and have better-defined cell borders (12). In contrast to hemangioblastoma, mitotic figures are common, the nuclear chromatin is often coarse and irregularly distributed and nucleoli may be prominent (8,12) (Fig 4B).
Given an adequate amount of tissue and paraffin sections, distinguishing hemangioblastoma and astrocytoma is generally easy. Special stains such as oil red O (which stains the cytoplasmic lipid in hemangioblastoma) and GFAP (positive in astrocytoma, but not hemangioblastoma) are of use. However, given the very different prognosis and treatment of these tumors, one may be called upon to make the distinction on frozen section, a task that can prove difficult, particularly in the case of higher grade astrocytomas which may show variable degrees of nuclear pleomorphism. Smears again are very helpful; smears of hemangioblastoma are far more cohesive than those of astrocytoma and lack the fibrillary background characteristic of astrocytic tumors (8). Neuropil is prominent at the edges of the tissue fragments in astrocytomas, unlike those of hemangioblastoma. The frayed cytoplasmic borders of stromal cells may resemble cytoplasmic extensions seen in astrocytic cells, but the latter, unlike the former, show numerous, delicate, interwoven cytoplasmic processes (12) (Fig 5A & 5B). Anaplastic astrocytomas show greater nuclear pleomorphism and coarseness and irregularity of the nuclear chromatin. Nuclear grooves and hemosiderin, which are often seen in hemangioblastomas, are uncommon in astrocytoma (8). Glioblastomas show prominent nuclear pleomorphism, as well as necro-hemorrhagic background diathesis and prominent mitotic figures (12) (Figs 5C and 5D).
In conclusion, hemangioblastomas in supratentorial locations are rare tumors, but their importance lies in the fact that they, along with meningioma, metastatic carcinoma and astrocytoma, comprise the differential diagnosis of supratentorial meningeal-based neoplasms. Cytologic evaluation of smear preparations, particularly air-dried smears stained with Diff-Quik, is extremely useful (more so than frozen sections) in the intraoperative diagnosis of hemangioblastoma and in its distinction from other tumors in the differential diagnosis.
REFERENCES:
![]() Contributed by Rajmohan Murali, Wayne I. Jones, Jenny Ma Wyatt
Contributed by Rajmohan Murali, Wayne I. Jones, Jenny Ma Wyatt