

FINAL DIAGNOSIS:
PART I: THYROID, TOTAL THYROIDECTOMY (11.7 GRAMS)
PART II: LYMPH NODES, CENTRAL COMPARTMENT, BIOPSY
DISCUSSION:
Hyalinizing trabecular tumor (HTT) of the thyroid gland is a rare neoplasm first described by Carney et al in 1987 as hyalinizing trabecular adenoma. It is also known as paraganglioma-like adenoma.
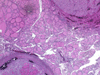
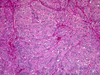
HTT usually occurs in middle-aged patients with a mean age of 47 years, and rarely occurs under the age of the 30. It has a female predilection and association with prior radiation exposure. There is a single report of HTT in a patient with Familial Adenomatous Polyposes. However, the etiology is unknown. Grossly, HTTs resemble typical adenomas. They are usually well-circumscribed, yellow tan, solid, and encapsulated with a thin fibrous capsule (Fig, 16).
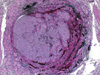
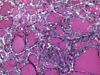
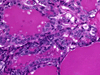
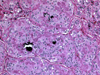
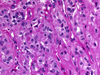
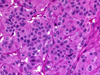
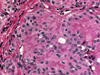
HTT is a follicular-derived neoplasm composed of medium to large cells with a prominent trabecular and nesting growth pattern. Hyalin material is present and represents perivascular collagen deposition and intracellular accumulation of intermediate fillaments, which can be mistaken for amyloid on FNA (Fig. 17). Microcysts and large cystic spaces may be seen. Colloid is scant or absent and psammoma bodies may be present. The cytoplasm is usually pale and eosinophilic. It also displays a distinctive morphologic feature so-called the "yellow body". The "yellow body" is a round pale with slight yellow tinge cytoplasmic paranuclear inclusion body with a refractile quality, and surrounded by a clear space. Ultrastructurally it has been shown to represent giant lysosomes. The nuclei are round to oval and more frequently elongated with fine chromatin and some degree of pleomorphism may be noted. Nuclear pseudo inclusion and grooves are frequent findings, making it difficult to distinguish from papillary carcinoma especially on cytological preparations (Fig. 18).
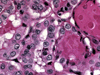
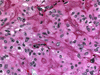
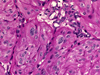
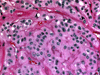
The differential diagnosis includes papillary thyroid carcinoma, medullary carcinoma (Fig. 19), paraganglioma, and follicular adenoma with trabecular pattern. Immunostains are helpful, as HTT is positive for thyroglobulin (Fig. 20) and TTF1, and negative for calcitonin, while medullary carcinoma will be calcitonin positive. HTT cells also show a distinct membranous and cytoplasmic MIB-1 (Ki-67) staining pattern, and are immunoreactive with type IV collagen.
Molecular studies have shown RET/PTC1 gene rearrangement in HTT, which is also the most common rearrangement associated with papillary carcinoma.
Lobectomy is the treatment of choice for hyalinizing trabecular tumor.
Considerable controversy has arisen as to whether HTT is a distinct entity or a growth pattern that can be present in variety of thyroid lesions, since a similar growth pattern and nuclear cytology along with hyalinization can be observed in chronic lymphocytic thyroiditis, colloid nodule, and papillary carcinoma.
The nature of HTT has not been fully understood and a malignant variant with capsular and/or vascular invasion has been reported.. Some authors have also suggested that HTT should not be categorized as a distinct thyroid tumor but as a variant of PTC. The link with PTC manifests itself by frequent merging or coexistence of HTT and PTC, occasional occurrence of cervical lymph node metastasis of PTC having an HTT-like pattern, the similar cytological features (nuclear grooves, pseudoinclusions, psammoma bodies), and similarities in their immunohistochemical profile such as high molecular-weight cytokeratin. Moreover, the detection of RET/PTC mutations similar to or even higher than that seen in papillary carcinoma, has been used as further evidence that HTT is a variant of PTC.
However, from a practical standpoint, tumors that show the classic features of hyalinizing trabecular tumor and lack capsular invasion and papillary growth features should still be considered as benign since none, to date, have behaved in a malignant fashion.
Follow up:
Patient is on Synthroid therapy, feels well since her surgery and has had no complications.
Acknowledgment:
Nicole Esposito, M.D.
REFERENCES:
![]() Contributed by Amer Heider, MD and Robert Peel, MD
Contributed by Amer Heider, MD and Robert Peel, MD