www.cytojournal.com
FINAL DIAGNOSIS
DISCUSSION:
The first report of thyroid metastasis from a primary renal carcinoma was by Leva in 1891.1 The incidence of metastasis to the thyroid gland in autopsy studies varies from 1.25% in unselected autopsy series to 24% in patients with widespread malignancy. In most autopsy series, breast and lung are the most common primary sites.2 Clinically, metastases to the thyroid are only rarely recognized, and renal cell carcinoma tends to occur most frequently.3 In one series of 43 patients with metastatic thyroid tumor, renal cell carcinoma was the primary site in 33% of cases,2 and in another it occurred in 4/15 patients with metastases to the thyroid.4 Although renal cell carcinoma is the most frequently detected primary site for metastasis to the thyroid, its overall occurrence is rare. In a review of cases from the AFIP from 1959 to 1998, 36 cases of metastatic renal cell carcinoma to the thyroid were identified among 37,158 benign and malignant thyroid neoplasms.5 Our case illustrates many of the typical features of metastatic renal cell carcinoma to the thyroid, as well as some of the difficulties that may be encountered in reaching the correct diagnosis.
Preoperative distinction between a primary versus secondary thyroid neoplasm is often impossible. Various thyroid malignancies, as well as benign conditions, may present with non-specific symptoms, including diffuse enlargement or a solitary nodule. These same thyroid changes may be found incidentally by CT scan or ultrasound in an asymptomatic patient. There are no characteristic radiographic differences among neoplasms, and, as in our patient, findings on ultrasound or CT scan may suggest a benign process such as multinodular goiter.5,6 Further contributing to the diagnostic difficulty, identification of renal cell carcinoma metastasis to the thyroid may occur years after the diagnosis of the primary malignancy. The longest reported interval has been 26 years. Alternatively, involvement of the thyroid has been the presenting sign in several cases.7
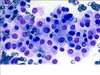
Fine needle aspiration is often helpful in establishing the correct preoperative diagnosis, but, occasionally, it is difficult to distinguish metastatic renal cell carcinoma from primary lesions of the thyroid, such as anaplastic carcinoma or the clear cell variant of follicular carcinoma.4 Clear cell change may be prominent in some oncocytic follicular carcinomas, as well.8 Clear cell change itself may be difficult to identify on FNA, and it may require repeat FNAs before the cells of interest are correctly identified. On initial FNA, in at least three reported cases, there were only findings consistent with nodular hyperplasia or follicular lesion.7,9,10 In contrast with tissue, the cytoplasm is not always optically clear in cytology specimens. In Papanicolaou, it tends to be wispy or foamy with a gossamer blue tint. In Diff-Quick, clear cells contain numerous small vacuoles sharply outlined against the intervening densely stained cytoplasm. In either case, the size and number of vacuoles may vary.11 These features are evident in the FNA sample from our patient. Similar characteristics may occur in Hürthle cells (image 17) or histiocytes, which may add to the challenge of identifying the "true" clear cells in a sample.
The difficulty of distinguishing clear cell renal cell carcinoma from other conditions which show clear cell features, may persist on histological evaluation. In these cases, immunohistochemical stains have proven to be extremely helpful. Thyroglobulin and/or TTF-1 are positive in the majority of primary thyroid lesions, while renal cell carcinoma is negative for these markers and more likely to show expression of CD10, vimentin, epithelial membrane antigen, and renal cell carcinoma immunostain.
One detail we left out of our patient's history is that he also had metastases to the pancreas, detected in 2003. Similar to thyroid, the pancreas is an unusual site for metastatic tumor of any origin.12 A review of clinical series demonstrates that metastatic tumors comprise about 3% of pancreatic tumors.13 However, also similar to thyroid, in clinical studies, renal carcinoma is the most common primary site for metastases to the pancreas.14 Up to 40% of patients with renal cell carcinoma have undiagnosed distant metastases at the time of initial presentation,15 with the most frequent sites being lung, liver, and bone. However, renal cell carcinoma is notorious for its tendency to metastasize to unusual sites,16 and, though infrequent, a few cases of simultaneous or metachronous metastases to the thyroid and pancreas, have been previously reported.17
In our patient, as previously noted, a total thyroidectomy was performed. The pancreatic metastases were also surgically resected with a spleen-preserving and pylorus-preserving total pancreatectomy. Surgical resection of metastatic renal cell carcinoma, if it occurs as a solitary metastasis in either pancreas or thyroid, may prolong survival. One study reported 60% of patients with isolated thyroid metastases were still alive after thyroidectomy with a median follow-up period of 5.2 years.18 A 5-year survival rate of up to 81% after pancreatic resection of renal cell carcinoma has been reported.12 However, it is unclear whether any survival benefit is derived from surgical treatment when metastases are widespread.
REFERENCES
![]() Contributed by Siobhan O'Connor, MD, Leon Barnes, MD and Karen Schoedel, MD
Contributed by Siobhan O'Connor, MD, Leon Barnes, MD and Karen Schoedel, MD