
DISCUSSION:
Dyshormonogenetic goiter (DG) is a rare disorder that affects 1 in 30,000 to 50,000 live births. Males are affected as commonly as females and most patients are discovered before age 20 (1). Patients typically present at birth or shortly thereafter with hypothyroidism, goiter or growth retardation (cretinism). The hypothyroidism is due to enzymatic block at various sites in T3/T4 pathway that result in any of the following:
The mutations responsible for these defects are currently being studied. Inheritance is usually autosomal recessive and may be associated with congenital deaf mutism in a condition called Pendred's syndrome (1).
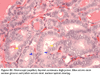
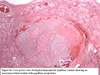
Grossly the DG thyroid gland is asymmetrically enlarged and multinodular. The histology is thought to vary depending on site of enzymatic block (3). The most commonly seen pattern is that of hypercellular nodules with mixed solid and microfollicular patterns or sometimes insular and simple papillary formations. Microfollicles commonly contain minimal or no pale staining colloid (4). The hypercellularity is due to follicular cell stimulation by TSH, which is overproduced by the pituitary gland as a result of persistent low thyroid hormone levels. In some cases mitoses, bizarre and giant hyperchromatic nuclei found between hyperplastic nodules, and fibrosis with irregularities that may mimic capsular invasion are found. These three features should not be mistaken for malignancy (4).
Clinically the differential diagnosis for congenital hypothyroidism includes aplastic or hypoplastic thyroid and autoimmune thyroiditis. In this case, although autoimmune thyroiditis was suspected clinically, the lack of a lymphocytic infiltrate made autoimmune thyroiditis very unlikely. The microscopic features of DG are similar to those seen in iatrogenic goiters in infants following systemic administration of radioactive iodine (4).
Without treatment patients die at birth, otherwise prognosis is excellent with thyroid hormone supplementation (1). Follicular adenoma can occur in thyroids with DG (5). Although rare, follicular carcinoma and papillary thyroid carcinoma have also been reported in patients with dyshormonogenetic goiters (6 and 7).
FOLLOW UP:
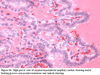
A follow up completion thyroidectomy was performed and showed another follicular adenoma, amicroscopic papillary thyroid carcinoma (Figs. 8a and 8b), and an atypical hyperplastic papillary nodule (Figs. 9a and 9b).
This case presented here illustrates the tumorigenic potential of a dyshormonogenetic thyroid gland.
REFERENCES:
![]() Contributed by by Kudakwashe Chikwava MB ChB. and Csaba Galambos MD.
Contributed by by Kudakwashe Chikwava MB ChB. and Csaba Galambos MD.