Case 368 -- Congenital Brain Tumor

 |
Contributed by L. F. Bleggi-Torres 1,2,3, M.D., PhD, MIAC, L. Z. B. Pope 1, M.D., A. Koerbel 4, M.D., C. V. Grande 4, M.D., J. C. Araújo 4, M.D. |
| |
- Department of Pathology (Neuropathology), Universidade Federal do Paraná, Curitiba, Brasil.
- Laboratory of Pathology, Hospital Nossa Senhora das Graças (HNSG),Curitiba, Brazil
- Laboratory of Experimental Pathology, PUC-PR, Curitiba, Brazil
- Neurosurgical Unit, HNSG, Curitiba, Brazil
|
 |
Published on line in November 2003 |
CLINICAL HISTORY:
A pregnant female patient in her early 30s was admitted to hospital with a history of 32 weeks gestation. There were signs of severe fetal suffering and an unusually large fetal skull was detected in ultrasound examination. A cesarean section was performed and a baby girl was delivered with cyanosis, vomiting and irritability. After basic neonatal procedures, neurosurgical evaluation revealed a large skull with congested and prominent superficial vasculature, prominent eyes, and a bulging anterior fontanel with wide open sutures. CT scan showed a large partially cystic mass that occupied approximately half of the intracranial space. Marked hydrocephalus was also noted. A neurosurgical procedure was performed and several fragments of the tumor were submitted for neuropathological examination. The baby expired at age 2 months and an autopsy examination was not performed.
MICROSCOPIC DESCRIPTION:


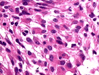


Histologic sections showed a tumor composed by a uniform population of large cells with minimal cell-to-cell variability immersed in a fibrillary background (Figure 1). The cells showed glassy, eosinophilic cytoplasm (Figure 2). Nuclei were usually eccentric with small nucleoli (Figure 3). Mitotic figures, necrosis, vascular proliferation, and perivascular lymphocyte cuffing were not seen. Immunohistochemical staining for GFAP (Figure 4) and vimentin (Figure 5) were strongly and diffusely positive. Immunostains for EMA, actin (HHF-35) and cytokeratin were negative.
FINAL DIAGNOSIS









