




MICROSCOPIC DESCRIPTION:
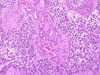
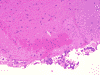
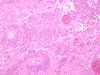
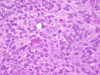
The H&E stained sections revealed a densely cellular neoplasm with prominent branching vasculature and extensive endothelial proliferation in some areas (Figures 9, 10). The neoplasm showed a well-demarcated border (Figure 11). The tumor cells had scant to moderate cytoplasm. In areas of lower cellularity, a vague perivascular pseudorosetting pattern was noted (Figure 12), but this pattern was not present in large areas of the neoplasm. Mitotic activity was prominent, and there was abundant necrosis (Figure 13). The hyperchromatic nuclei were often grooved or folded. Rare pseudoinclusions were identified (Figure 13). Focally, there were regions showing rounded nuclei and cytoplasmic clearing (Figure 14). In other areas, the vessels were thick and hyalinized. Immunohistochemical stains for CAM 5.2, S100, HMB45, desmin, neurofilament proteins and synaptophysin were negative within the neoplasm (Figure 15). Ki67 immunohistochemical stain highlighted nuclei of many tumor cells (Figure 16). The perivascular hypocellular areas were uniformly immunoreactive for GFAP (Figure 17), with focal staining of some tumor cells. The diagnostic impression was anaplastic ependymoma, although anaplastic oligodendroglioma could not be excluded. In order to further classify this tumor, electron microscopic and molecular genetic studies were performed.
MOLECULAR STUDIES:
Molecular genotyping was non-contributory. Loss of heterozygosity at markers for P16 and PTEN was present, consistent with anaplastic grade. However, no loss of heterozygosity at 1p/19q was demonstrated. Analysis at 22q was limited by non-informative markers.
ELECTRON MICROSCOPIC EXAMINATION:
Electron microscopic examination revealed that the neoplastic cells had numerous microvilli and rare intercellular junctions, indicative of ependymal rather than oligodendroglial differentiation (Figure 18, 19). In addition, a definitive cilium with basal bodies was identified (Figure 20), further supporting the final histologic diagnosis of anaplastic ependymoma.