
![]() Contributed by Edward C. Klatt MD, Department of Pathology, University of Utah Health Sciences Center
Contributed by Edward C. Klatt MD, Department of Pathology, University of Utah Health Sciences Center
![]() Published on line in June 2000
Published on line in June 2000
PATIENT HISTORY:
A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Prior to leaving on that trip, she had had a workup two months earlier that included an abdominal ultrasound which had shown only gallstones and a chemistry panel which showed only a very slightly elevated GGT at 59 U/L. A chemistry panel a year prior had shown normal findings except for a slightly elevated alkaline phosphatase at 169 U/L and a slightly elevated GGT at 64 U/L.
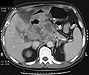 She was hospitalized, and an abdominal CT scan revealed a tumor mass involving the head of the pancreas. Sphincterotomy with bile duct drainage by placement of two stents was performed by endoscopic retrograde pancreatography (ERCP) because of high grade stenosis of the distal common bile duct. An exploratory laparotomy was performed and an inoperable mass was found in the head of the pancreas. A cholecystectomy was also performed, and the gallbladder showed acute phlegmonous cholecystitis and pericholecystitis. Chemotherapy with one cycle of 1500 mg Gemcytabine was given. Two months later repeat ERCP was performed with placement of two additional stents. Despite placement of several stents, the patient's bilirubin remained elevated and followup examination showed that the intrahepatic biliary ducts remained dilated. Abdominal CT two months later showed a large mass (Fig 1). She arranged to have hospice care. Over the next several weeks she developed intermittent nausea and vomiting, which was not associated with eating. She noted increasing jaundice. Weight loss of 5 kg in four weeks was noted. Emesis at that time was heme positive. She experienced several episodes of dyspnea and chest pain. She continued to deteriorate and died at home six months following the appearance of her initial symptoms.
She was hospitalized, and an abdominal CT scan revealed a tumor mass involving the head of the pancreas. Sphincterotomy with bile duct drainage by placement of two stents was performed by endoscopic retrograde pancreatography (ERCP) because of high grade stenosis of the distal common bile duct. An exploratory laparotomy was performed and an inoperable mass was found in the head of the pancreas. A cholecystectomy was also performed, and the gallbladder showed acute phlegmonous cholecystitis and pericholecystitis. Chemotherapy with one cycle of 1500 mg Gemcytabine was given. Two months later repeat ERCP was performed with placement of two additional stents. Despite placement of several stents, the patient's bilirubin remained elevated and followup examination showed that the intrahepatic biliary ducts remained dilated. Abdominal CT two months later showed a large mass (Fig 1). She arranged to have hospice care. Over the next several weeks she developed intermittent nausea and vomiting, which was not associated with eating. She noted increasing jaundice. Weight loss of 5 kg in four weeks was noted. Emesis at that time was heme positive. She experienced several episodes of dyspnea and chest pain. She continued to deteriorate and died at home six months following the appearance of her initial symptoms.
LABORATORY FINDINGS:
| Analyte | Value | Reference Range | Units |
|---|---|---|---|
| Sodium | 137 | 136-144 | mmol/L |
| Chloride | 100 | 101-111 | mmol/L |
| Potassium | 4.1 | 3.7-5.2 | mmol/L |
| Bicarbonate | 29 | 20-29 | mmol/L |
| Creatinine | 0.6 | 0.7-1.1 | mg/dL |
| Total Protein | 7.2 | 6.3-7.9 | g/dL |
| Calcium | 8.5 | 8.5-10.3 | mg/dL |
| Bilirubin, total | 10.5 | 0.2-1.3 | mg/dL |
| AST | 62 | 10-34 | U/L |
| ALT | 44 | 5-59 | U/L |
| LDH | 219 | 105-205 | U/L |
| Alkaline Phosphatase | 391 | 45-150 | U/L |
| Gamma-GT | 51 | 0-33 | U/L |
| Amylase | 48 | 23-85 | U/L |
| Lipase | 48 | 30-190 | U/L |
| CEA | 170 | 0-3 | ng/mL |
| CA 19-9 | 16011 | 0-37 | U/mL |