



FINAL DIAGNOSIS:
ASYMPTOMATIC PULMONARY CAVITARY LESION SECONDARY TO CHRONIC COCCIDIOIDES IMMITIS INFECTION
DISCUSSION:
Infection by Coccidioides immitis (Coccidioidomycosis) can manifest itself in several different ways as illustrated by the multiple historical names it has received (Coccidial Granuloma, Valley Fever, Desert Rheumatism, Posada's Disease, California Disease, etc.). This fungus has an interesting history which reportedly begins in 1891 with an Argentinian soldier who presented with unusual "skin tumors" thought to be mycosis fungoides. Tissue biopsies from this patient, however, revealed several round sac-like structures with internal "spores" resembling the protozoan Coccidia. The soldier was subsequently followed for 11 years by a medical student, Alejandro Posada (the origin of Posada's Disease), and ultimately died with ongoing skin disease. The first North American clinical cases were subsequently described in 1894, and in 1896 Dr. Rixford in San Francisco began attempts at subculturing the identified "parasite," but repeatedly discarded the culture plates secondary to what was believed to be a contaminating "mold." In 1900, Dr. Ophuls and Dr. Moffitt described the "dimorphic life cycle" of the fungus with a mold phase in vitro, and a tissue phase "spherule" containing mature sporangia that was previously mistaken for the protozoan Coccidia. These investigators also concluded the lung as the primary entry site, suggesting inhalation of the infectious agent was the initial insult.
Up until 1929, almost all reported cases showed extensive granulomatous dissemination to multiple organs, and/or extensive skin disease with erythema nodosum and erythema multiforme. However, in that same year, the first mild case with complete resolution of pulmonary symptoms occurred in a student E. Dickson from an accidental lab exposure. Dr. Dickson was later credited in 1937 with the modern term for all stages of the disease known as Coccidioidomycosis. The first coccidial skin test utilizing extracts from Coccidioides cultures was developed in 1927, and would later provide the basis for establishing the epidemiologic characteristics of this disease. The recovery of the organism from soil in the San Jaoquin Valley in 1932, paralleled these skin test developments. Armed with the ability to identify the fungus in the environment, in the 1940's and 1950's researchers began large scale skin testing and epidemiologic tracking. The largest regions studied in the US occurred within many Southwestern U.S. military sites as they were being constructed. Results of these studies showed the endemic regions to be the desert Southwest US along the Rio Grande river, Northern Mexico, Guatemala, Honduras, Colombia, Venezuela, Bolivia, Argentina, and Paraguay. These regions all share low rainfall, hot summers, and mild winters in common along with similar bush, cacti, and rodent populations.
Our modern understanding of Coccidioidomycosis is essentially unchanged with a recognized primary and disseminated form of the disease. There is no sex, race, or gender predilection for susceptibility to the disease within endemic areas; however, an increased incidence of dissemination exists within the African American and Filipino populations when compared to Asian, Mexican, American Indian, and Caucasian groups. As expected, it occurs most commonly in those persons with increased exposure to the soil in endemic areas: construction workers, farm workers, archaeologists and archaeology students, telephone post-hole diggers, and occasionally laboratory personnel. The primary form usually begins with fever and pleuritic chest pain within 2 weeks, and is associated with both a productive and non-productive cough. 40% of those with positive skin tests will experience symptoms, however; suggesting that the majority of patients suffer mild or subclinical infections. The primary infection is also associated with fine, diffuse rashes mistaken for Scarlet Fever or measles, erythema nodosum over the lower extremities and buttocks, and erythema multiforme manifesting as macules/papules over the upper torso and face. The pulmonary sequelae include pneumonitis, granulomatous infiltrates ("coccidiomas"), and cavitary lesions as seen in the current case. These coccidiomas are occasionally thought to represent a cavitating neoplasm, and are sometimes surgically removed since cultures are infrequently positive ( IMAGE 8 ). Most cavities remain asymptomatic, however, and may spontaneously resolve. 23% of patients develop hemoptysis, and many develop a secondary bacterial infection within the cavity. The disseminated form usually occurs via a hematogenous route, and can frequently be fatal. Many cases are thought to be secondary to "re-activation" of a subclinical infection during a newly developed immunosuppressed state. Progression of the dissemination is quite variable with occurrence immediately after the primary infection or sometimes months later in the course. Disseminated disease manifests itself at with diffuse lymphadenitis, similar skin lesions, abscesses, draining sinuses, osteolytic bone lesions (20%), arthritis at neighboring joints ("Desert Rheumatism"), indolent chronic meningitis (33-50%), and granulomatous lesions in the liver, kidneys, adrenal glands, and multiple other organs.
The laboratory diagnosis of Coccidioides immitis revolves around differentiation of the fungus from other species that produce arthrospores by hyphal segmentation. These include most notably Malbranchea, Geotrichum candidum, Oospora, and Gymnoascaceae species. Malbranchea, considered a non-pathogen, is a principal "look-alike" that also shares a monosaccharide antigenic moiety of 3-O-methylmannose with Coccidioides. This sugar is found within an alkali-soluble extract called "Ag2," and is found only in these two fungi. Coccidioides will grow on a number of mycologic media, with mold phase growth usually within 3-5 days at 25-37 C on Sabouraud dextrose agar. The colonies are usually moist-grey initially, then white-cottony as the aerial mycelium develop, and later the larger colonies will turn brown-tan. Due to the exposure risk with aeration, Coccidioides should never be grown on Petri dishes, only tube methods; and specimen handling should always take place within a ventilation hood. The fungal morphology shows coarse, septate, branched hyphae that are thinner than the corresponding arthroconidia ( IMAGE 5). Mature arthroconidia usually are "barrel-shaped", and develop through hyphal segmentation accomplished by unique alternating "dysjunctor cells" or "degenerating intervening cells." ( IMAGE 6, and IMAGE 7 ) Young cultures may show "racquet hyphae." Malbranchea morphology shows same size hyphae and arthroconidia in contrast to Coccidioides, and also does not show the characteristic "barrel-shaped" arthroconidia of Coccidioides ( IMAGE 9). The degenerating cells also provide the characteristic four sails or wings on the free infectious Coccidioides arthroconidia, with these sails absent in Malbranchea arthroconidia.
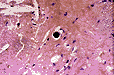
A special synthetic media (Converse liquid media) can be used to enhance the formation of the Coccidioidal spherules when the fungus culture is grown at 37-40 C in an increased CO2 environment. The spherules, 30-60 um in size, can also be visualized in fluid exudates, sputum samples (most common), and skin biopsies using potassium hydroxide, Calcofluor white, or Pap stains preparations. On tissue sections, the spherule can be demonstrated on routine hematoxylin and eosin staining ( IMAGE 10 ), and occasionally only the spherule sac itself ( IMAGE 11 ), or the intact spherule may be present ( IMAGE 12 ) on modified Gomori methenamine silver staining (Grocott stain).
Confirmatory tests of historical importance now include animal inoculation studies in mice and guinea pigs looking for production of these diagnostic tissue spherules, and the Exoantigen test developed in 1978. This method uses a methiolate fungicide to extract antigens from 7-10 day old cultures for analysis with Coccidioides specific antisera in an immunodiffusion assay. The turn-around time for this method is roughly 3-4 days. Most modern laboratories, however, use commercially-available kits with specific DNA probes for a variety of fungi. The reported sensitivity of these assays is 98.8%, and specificity is 100%. The majority of these assays use a sonication method to extract fungal ribosomal RNA (rRNA) from colonies as small as 1-2 mm-squared. An acridinium-based chemiluminescent DNA probe that is fungi specific, is then hybridized with the rRNA, followed by lysis of any unbound acridinium probe. The amount of DNA:rRNA hybrid formed is then quantitated in relative light units via a luminometer. One study evaluated the Coccidioides probe with a reported sensitivity of 99.2% (121/122 cases) and a specificity of 100% (0/164 non-Coccidioides cases). Three of the 122 cases were also tissue spherule specimens, suggesting that the diagnosis may be made using tissue samples in addition to cultures. These DNA probe assays have been shown to be equivalent to the Exoantigen test, and with a turn-around time of approximately 2 hours, they have virtually replaced the Exoantigen test as the gold standard in confirmatory testing.
Future development of polymerase-chain reaction (PCR) assays may expand our ability to detect these fungal infections earlier. A number of ongoing studies are focusing on the development of "universal primers" for all of the pathogenic fungi. This theory involves the amplification a highly-conserved region in the fungal genome in all of the common pathogens, and the development of species specific probes for detection. A recent study described 21 such specific DNA probes that were developed at the Mayo Clinic for use on DNA/RNA recovered from sputum, bronchoalveolar lavage, cerebrospinal fluid, urine, and blood specimens. The authors report a specificity of 100% for a region amplified out of a portion of the 28S rRNA from fungi such as Aspergillus, Candida, Cryptococcus, Coccidioides, and Histoplasmosis. Another study used a 197-bp amplicon from the 18S rRNA to demonstrate both inter-species and intra-species variation by single-strand conformational polymorphism (SSCP). These research efforts and other methods will most likely be used during future outbreaks/epidemics to establish a new era of "Molecular Taxonomy," or what is now referred to as "Molecular Epidemiology."
Coccidioidomycosis is currently gaining increased recognition as an opportunistic infection in HIV/AIDS patients, transplant recipients, and other immunosuppressed populations. Currently, an estimated total of 100,000 cases are diagnosed annually in the US, mostly in the desert Southwest. The most recent epidemic occurred in 1992 in California, with fifteen times the number of annual cases at its peak. Fortunately, person-person transmission of infection is reported as extremely rare. However, a recent 1999 review of Coccidioidomycosis by Dr. Galgiani cites that 46% of Coccidioides cases detected in the HIV/AIDS population occurred outside of endemic areas, suggesting it is currently a disease of "emerging" national/international importance due to emigration patterns and the ease of travel. The current case is in part an example of this phenomenon, since as one resource states: "Because of the persistence of an asymptomatic cavity, the lesion is likely to be discovered after the patient has left the endemic area." (Medical Mycology, 1992) Therefore, there is a push from the clinical side of medicine for more rapid, earlier diagnostic methods, and preventative methods. One such area of intensive research currently is vaccine development for use in endemic areas in human and veterinary medicine. The first human trial of formalin-killed Coccidioidal spherule/whole cell vaccine occurred in 1993 in the San Jaoquin Valley, but it showed no significant protection when compared to placebo controls. Current studies are focusing on the development of recombinant protein and DNA vaccines from antigenic sites such as the previously mentioned "Ag2." In trials where mice are challenged with intraperitoneal injection of arthroconidia 4 weeks status post vaccination, both the protein and DNA vaccines showed equivalent amounts of protection, with decreased colony-forming units of Coccidioides recovered from the lungs of the vaccinated mice. These studies may one day lead to the inclusion of a "Coccidioides vaccine" in vaccination programs, or conceivably as a part of the traveler's vaccination protocol.
REFERENCES:
![]() Contributed by Douglas R. Johnson, MD, A. William Pasculle, ScD and John Sheaffer, MS
Contributed by Douglas R. Johnson, MD, A. William Pasculle, ScD and John Sheaffer, MS