
FINAL DIAGNOSIS: -- HOMOZYGOUS FACTOR VII DEFICIENCY. Ten days after admission, permission was obtained for compassionate use of recombinant activated Factor VIIa (rFVIIa). This product was administered at a dose of 15 ug/kg every 3 hours for 14 days. With therapy, the PT corrected to the desired goal of 14 seconds. The patient's hematuria and heme-positive stools resolved completely with therapy. On day 35 of life, the patient was discharged into foster care with no clinical bleeding. Close followup in the outpatient coagulation clinic was planned.
DISCUSSION
This child has homozygous Factor VII deficiency manifesting clinically as severe intracranial hemorrhage, hematuria, heme-positive stools, easy bruising, and oozing from his circumcision site. A Factor VII assay revealed an activity of 0.07 U/ml while receiving fresh frozen plasma, only 10% of the lower normal limit. The combination of a difficult vaginal delivery and exposure to cocaine in utero may have resulted in increased intracranial pressure with subsequent hemorrhage. In the face of nearly undetectable Factor VII activity, hemostasis was difficult to achieve, even with frequent administration of fresh frozen plasma (FFP). Permission for compassionate use of recombinant activated Factor VII (rFVIIa, Novo Nordisk Pharmaceuticals, Princeton, New Jersey) was obtained, with temporary correction of the patient's PT and adequate hemostasis (1).
Hereditary Factor VII deficiency is a rare (1/500,000 individuals) autosomal recessive condition associated with decreased factor activity (2). The Factor VII protein may be either absent (Type I Factor VII deficiency) or present in a functionally defective state (Type II Factor VII deficiency) (3). Functional Factor VII protein is required for adequate activity of the extrinsic arm of the coagulation cascade (see diagram 01). In precursor form, Factor VII has no activity. However, upon binding to tissue factor (TF) exposed by vascular injury, Factor VII protein is readily cleaved to its active form, Factor VIIa. The tissue factor/Factor VIIa complex then goes on to function as a protease and activates Factors IX and X, as well as Factor VII. Factor VII has the shortest half-life (3-5 hours) of the known coagulation proteins, and Vitamin K is required for its synthesis.
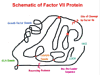
The gene for Factor VII is located at chromosome 13q34, approximately 2.8 kilobases upstream from the Factor X gene (4). The human Factor VII gene is expressed in liver, but steady state levels of messenger RNA are low (5,6). A schematic diagram of the primary sequence of the Factor VII protein is shown in (diagram 02). A pre-pro-leader sequence is cleaved during protein synthesis (7). Activation of the protein requires: 1) binding of the growth factor domain to the "growth-factor-like" receptor site present in tissue factor produced by injured vessels and 2) subsequent cleavage at amino acid 152 by tissue factor or Factor Xa (see diagram 02). The two cleaved portions remain covalently linked by a disulfide bond. The carboxy portion of the protein contains a typical serine protease domain, with three highly conserved histidine, aspartate and serine residues. The majority of individuals with Factor VII deficiency have a disparity between functional protein activity and presence of antigen (7). That is, Factor VII activity can be virtually absent, yet Factor VII antibodies detect normal levels of protein. Such is not the case for hemophilia A (Factor VIII deficiency) and hemophilia B (Factor IX deficiency), where there tends to be stronger agreement between activity and protein levels. This observation suggests that 1) the tertiary structure of the Factor VII protein is extremely important for function, i.e., the growth factor and catalytic domains must be in the proper conformation, and 2) single point mutations in critical areas of the gene sequence may yield a nonfunctional protein. Approximately 150 cases of Factor VII deficiency have been reported in the world literature (2). Of those cases studied at the molecular level (approximately 44) 24 different lesions were identified: Twenty single base-pair substitutions, three single base-pair deletions, and one deletion of 17 base pairs. Of the 40 cases with single base-pair substitutions, the base pairs encoding amino acids 304 and 310 were most often involved (9/40 and 5/40, respectively) (2). Both of these amino acids are located within the serine protease catalytic domain.
The accepted current therapy for Factor VII deficiency in the United States and Canada is frequent administration of FFP in order to partially correct the PT and to prevent bleeding (2). The frequency of FFP transfusion can often be decreased as the individual approaches adolescence and can protect his or her body from injury. An alternative therapy is prothrombin complex , which is comprised of Factors II, VII, IX, and X. These therapies are not ideal for several reasons: 1) frequent administration of these products can result in significant volume overload; 2) the risk of infectious disease transmission is significant; and 3) adequate correction of the PT cannot always be maintained due to the short half-life (3 - 5 hours) of Factor VII. In addition, administration of prothrombin complex results in high levels of Factors II, IX, and X, which have appreciably longer half-lives than Factor VII. An excess of these factors presents an increased risk for thrombosis (8). FFP transfusion works well for those individuals with a mild Factor VII deficiency but is not sufficient to treat patients with severe deficiency. An appreciable number of infants with severe Factor VII insufficiency present with devastating intracranial bleeds (9). Recombinant activated Factor VII has not been associated with transmission of any infectious diseases (2). However, the recombinant form is not FDA approved for prophylactic use in the United States; it is available only for compassionate use and use in clinical trials.
Permission was obtained to treat this child with a 14-day course of recombinant activated Factor VII. He experienced excellent correction of his PT, and his bleeding diathesis stopped for the course of the therapy. The child was discharged into foster care but was rehospitalized one week later with heme-positive stools. His twin brother has been tested and does not have Factor VII deficiency. As of this writing, the patient is two months old and remains hospitalized, requiring daily infusions of FFP. The child feeds well, responds to sounds, and follows with his eyes. However, the permanent neurologic injury caused by the intracranial hemorrhage remains to be fully appreciated.
REFERENCES
![]() Contributed by Karen K. Deal, M.D. Ph.D., Ileana Lopez-Plaza M.D. and Margaret V. Ragni, M.D., M.P.H.
Contributed by Karen K. Deal, M.D. Ph.D., Ileana Lopez-Plaza M.D. and Margaret V. Ragni, M.D., M.P.H.