![]() Contributed by Laetitia Lebrun, Marie Le Mercier, Barbara Melendez, Isabelle Salmon, Nicky D'Haene
Contributed by Laetitia Lebrun, Marie Le Mercier, Barbara Melendez, Isabelle Salmon, Nicky D'Haene
![]() Laboratory of Pathology, Erasme University Hospital, Free University of Brussels (ULB), Brussels, Belgium
Laboratory of Pathology, Erasme University Hospital, Free University of Brussels (ULB), Brussels, Belgium
CLINICAL AND RADIOLOGICAL FINDINGS
A 39-year-old man was admitted in 2009 following epileptic seizure associated with visual impairment. MRI revealed an expansive and infiltrative lesion in the right parieto-occipital lobe with a cortico-subcortical localization. This lesion was hypointense in T1-weighted images and showed no contrast enhancement after gadolinium injection. Methionine-positron emission tomography (MET-PET) revealed high methionine uptake in this lesion. Partial surgical resection of the lesion was performed. No adjuvant therapy was administered at this moment. MRI images showed progression of the lesion in 2014 but the patient refused surgical intervention and other therapies. In 2017, following painful headache associated with neurological deficit, the MRI suggested progressive neoplasm in the right parieto-occipital lobe (Figure 1) with areas of enhancement on post contrast MRI. MET-PET revealed heterogeneous increased metabolic uptake, suggesting progression of the disease. New surgery was performed.
PATHOLOGICAL FINDINGS
Histopathological examination of the 2009 surgical resection specimen revealed an infiltrating tumor of moderate cellularity, consisting of monomorphic cells with round nuclei and perinuclear haloes (Figure 2). Few mitoses were observed and there was no necrosis. Immunohistochemistry (IHC) revealed strong diffuse GFAP and TP53 staining (Figure 3), a low proliferation rate evaluated by Ki67 (1%) and no staining for IDH1 R132H. No 1p/19q co-deletion was detected by Fluorescence in Situ Hybridization (FISH) and Next Generation Sequencing (NGS) (Figure 4) (Supplementary data). Microscopic evaluation of the 2017 specimen revealed an infiltrating lesion of high cellularity with a tumor block of monomorphic round cells, similar to the 2009 sample (Figure 5), and other areas of infiltrating cells with hyperchromatic and more pleomorphic nuclei (Figure 6). Both morphological areas were associated with increased cellularity, mitoses and nuclear atypia. The tumor showed positive staining for GFAP, and negative staining for IDH1 R132H. However, differences were observed between the different morphological areas for other immunohistochemical stainings: the tumor block showed an increased Ki67 proliferation rate (10%), scarce positive TP53 nuclei staining (Figure 7), and diffuse ATRX staining (Figure 8). In contrast, the infiltrating areas showed diffuse intense TP53 staining (Figure 9) and lack of ATRX protein expression (Figure 10). FISH and NGS showed complete loss of 1p and 19q arms in the tumor block (Figure 11), while there was no 1p19q co-deletion in the infiltrating cells (Figure 12).
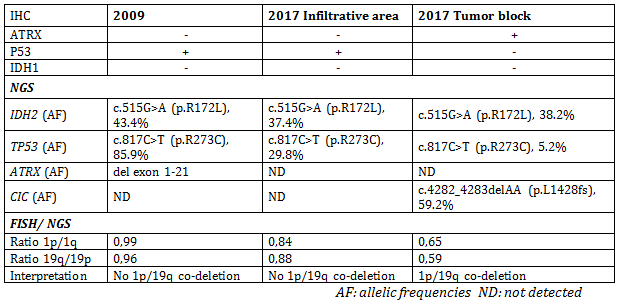
IHC, FISH and targeted NGS (Supplementary Data) analyses were performed in the 2009 sample and, separately, in both morphological areas of the 2017 sample. Here is a summary of these results:
What is your diagnosis?
 International Society of Neuropathology
International Society of Neuropathology