Brain Pathology Case of the Month - February 2019
 Contributed by Sergio Cavalheiro1, MD, PhD, Marcos Devanir Silva da Costa1, MD, MSc, Cristina Góes Schaurich1, MD, Andrea Maria Cappellano2, MD
Contributed by Sergio Cavalheiro1, MD, PhD, Marcos Devanir Silva da Costa1, MD, MSc, Cristina Góes Schaurich1, MD, Andrea Maria Cappellano2, MD
Nasjla Saba-Silva2, MD, Maria Teresa de Seixas Alves3, MD, PhD, Joăo Norberto Stavale3, MD, PhD
 1 Department of Neurosurgery, Federal University of Sao Paulo, Sao Paulo, Brazil
1 Department of Neurosurgery, Federal University of Sao Paulo, Sao Paulo, Brazil
2 Pediatric Oncology Institute/GRAACC, Department of Pediatrics, Federal University of Sao Paulo, Sao Paulo, Brazil
3 Department of Pathology, Federal University of Sao Paulo, Sao Paulo, Brazil
CLINICAL HISTORY
An eight-year-old female patient, who was previously healthy, presented with episodes of a headache followed by recurrent bilateral eyelid movements described as a "heartbeat" that lasts few seconds following by spontaneous remission without loss of consciousness. These symptoms were experienced periodically for about 30 days. On physical examination, the patient showed no motor, sensory, or cognitive deficits. A CT brain scan revealed a left thalamic mass lesion without contrast enhancement. MRI revealed an extensive left thalamic tumor that was hypointense/isointense on T1-weighted MRI, hyperintense on T2-weighted MRI. The sagittal (Figure 1a) and coronal (Figure 1b) views of a T1- weighted MRI after gadolinium injection evidenced no-enhancement of a large anterodorsal left thalamic tumor compressing the third ventricle. While the axial view of a FLAIR MRI showed the hyperintensity of a large tumor in the left thalamus (Figure 1c). A transcranial EEG showed no abnormalities.
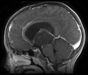
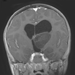
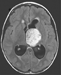
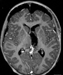
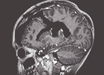
The patient underwent microsurgery to resect the tumor using a left frontal transcortical approach that was performed with the aid of surgical microscope and intraoperative electrophysiological monitoring of somatosensory evoked potentials. The patient achieved gross total resection of the tumor (Figures 1d, 1e), and experienced no postoperative deficits or any episodes of blepharospasm even from the first postoperative day. The patient remains on outpatient follow-up after 15 months without adjuvant treatment, and the most recent brain MRI revealed no recurrence of the injury.
GROSS AND MICROSCOPIC PATHOLOGY
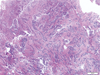
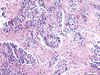


Examination of the resected tissue showed bipolar cells that were elongated and homomorphous with moderate cellularity (Figure 1f). The tumors cells have spindle-cell morphology, displayed in angiocentric patterns and perivascular rosettes (Figure 1g). No mitotic activity is appreciated. No vascular proliferation or necrosis present. The tumor is immunoreactive for GFAP (Figure 1h). A stain to neurofilament demonstrates the infiltrative nature of the lesion. The tumor demonstrates dot-like perinuclear immunoreactivity for EMA. The frequency of Ki67/Mib-1 immunolabeling in the tumor cells is very low (Figure 1i). MYB rearrangement was detected by iFISH in the tumor samples. What is your diagnosis?
FINAL DIAGNOSIS









 International Society of Neuropathology
International Society of Neuropathology