Brain Pathology Case of the Month - June 2015
 Contributed by Kara Leigh Krajewski, MD1, Jakob Matschke, MD2, Niklas Humke, MD1, Wolfgang Börm, MD3, Manfred Westpha, MDl1, Nils Ole Schmidt, MD1
Contributed by Kara Leigh Krajewski, MD1, Jakob Matschke, MD2, Niklas Humke, MD1, Wolfgang Börm, MD3, Manfred Westpha, MDl1, Nils Ole Schmidt, MD1
1Department of Neurosurgery, 2Institute of Neuropathology, University Medical Center Hamburg-Eppendorf, Martinistr. 52, 20246 Hamburg, Germany
3Department of Neurosurgery, Ev.-Luth. Diakonissenanstalt zu Flensburg, Zentrum für Gesundheit und Diakonie, Knuthstr. 1, 24939 Flensburg, Germany
CLINICAL HISTORY AND NEUROIMAGING
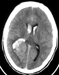
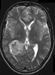
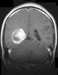
A 19-year-old male presented with an acute episode of headache, nausea and neck stiffness. The patient displayed a GCS of 15 with a mild left-sided hemiparesis. CCT revealed a mass in the right ventricular trigone with hemorrhage into the ventricle (Fig 1). An MRI showed contrast enhancement of the lesion (Fig 2; T2 axial view and Fig 3; T1 contrast-enhanced coronal view).



Microsurgical resection of the tumor was performed via a right-sided temporo-parieto-occipital approach with ultrasound-assisted transcortical entry into the right ventricle where the tumor had contact with the choroid plexus. Gross total resection could be achieved. Postoperatively, the patient had no neurological deficits. Postoperatively, fractionated radiation therapy was initiated and well-tolerated. Follow-up cranial MRIs at regular intervals confirmed gross total resection with no recurrent tumor.


Five months postoperatively, the patient complained of right-sided neck and arm pain, hemihypesthesias, gait unsteadiness and right-sided hand weakness. An emergency CCT showed no hemorrhage, new lesions or tumor progression while the patient experienced an acute exacerbation with a progressive tetraparesis. Spinal MRI showed intra- and extramedullary lesions at C5/6 (Fig 9), T2/3, L1 and L4 (Fig 10). An emergency cervicothoracic laminectomy at C5-7 and T2-4 with partial resection of the spinal tumors was performed to relieve the spinal cord compression. Histological analysis showed a tumor which was morphologically and immunohistochemically indistinguishable from the first tumor. Postoperatively, the patient initially experienced a steady improvement. However, a few days later the patient experienced an acute headache and loss of consciousness requiring intubation due to subarachnoid and intraventricular hemorrhage causing occlusive hydrocephalus and global brain edema. Minimal supportive therapy measures were initiated and he died 10 days later due to respiratory failure.
MICROSCOPIC FINDINGS
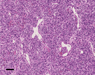
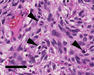
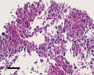
Histology revealed a highly cellular tumor with a swirling or jumbled appearance and numerous thin-walled hyalinized vessels of characteristic "staghorn-pattern" (Fig 4; H&E) featuring necrosis and significantly elevated mitotic activity (>5/10 high-power fields; arrowheads Fig 5; H&E).. The tumor cells were plump or spindle-shaped and haphazardly arranged. Nuclei were oval to round featuring small nucleoli and finely dispersed chromatin. Reticulin staining highlights the delicate fiber network surrounding individual tumor cells (Fig 6; Gomori´s stain). Immunohistochemically, the tumor cells showed strong positivity for vimentin and CD177, and only focally moderate staining for CD34 (Fig 7; arrows, arrowheads show tumor vessels; immunohistochemistry for CD34); epithelial membrane antigen (EMA), S100, keratin, actin, desmin, CD99 and GFAP were negative. Very high proliferative activity is seen with roughly 30% Ki67-positive tumor cell nuclei (Fig 8; arrow: mitotic figure; immunohistochemistry for Ki67). A fragment of the recurrent tumor shows identical morphological features (Fig 11; H&E). What is your diagnosis?
FINAL DIAGNOSIS











 International Society of Neuropathology
International Society of Neuropathology