Brain Pathology Case of the Month - July 2012
 Contributed by Marina Paola GARDIMAN1, Matteo FASSAN1, Enrico ORVIETO1, Loredana IARIA1, Milena CALDERONE2,
Contributed by Marina Paola GARDIMAN1, Matteo FASSAN1, Enrico ORVIETO1, Loredana IARIA1, Milena CALDERONE2,
Rodica MARDARI2, Domenico D'AVELLA3, Giorgio PERILONGO4
 1 Department of Medicine (DIMED), Surgical Pathology & Cytopathology Unit,
1 Department of Medicine (DIMED), Surgical Pathology & Cytopathology Unit,
University Hospital of Padua, 35100 Padua, Italy
2 Division of Neuroradiology, University Hospital of Padua, 35100 Padua, Italy
3 Department of Woman's and Child's Helath, Division of Pediatric Neurosurgery, University Hospital of Padua, 35100 Padua, Italy
4 Department of Woman's and Child's Helath, Division of Hematology-Oncology, University Hospital of Padua, 35100 Padua, Italy
CLINICAL HISTORY AND NEUROIMAGING
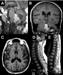
A 14-year-old girl with a recent history of sciatica and ataxic gait was admitted to the Pediatric Neurosurgery service. Brain and spine MRIs revealed a mildly heterogeneously contrast-enhancing mass with a cystic component in the 4th ventricle with caudal extension through the foramen of Magendie with compression of the medulla (Figure 1A). Another cystic mass with a large enhancing nodule was detected in the left cerebellar hemisphere (Figure 1B). The spinal MRI revealed an extensive septated syrinx as well as an intramedullary contrast-enhancing nodule at T4 (Figure 1D). Diffuse leptomeningeal enhancement with scattered nodules was visible in the suprasellar cistern, internal auditory canals, interpeduncular fossa, the ventral brainstem as well as the spinal cord. Moreover two solid, contrast-enhancing lesions were detected in the right temporal lobe (Figure 1C); and in the sacral spinal cord, a "drop" metastasis was detected within the thecal sac (Figure 1E). A specific radiological diagnosis was not achieved. Multiple biopsies of the cerebellar lesion and of the tissue in the thecal sac were performed.
MICROSCOPIC FINDINGS

Histologic examination of all biopsies showed a pleomorphic tumor mainly composed of spindle-shaped cells intermingled with multinucleated giant cells and large cells with a pleomorphic nuclei(Figure 2A). Many eosinophilic granular bodies were also present, whereas cytoplasmic vacuolization were rarely observed (Figure 2B). There was a widespread dense intercellular reticulin network as well as perivascular lymphocytic infiltrates. Neither necrosis nor microvascular proliferation were observed. Immunohistochemically, many tumor cells were positive for GFAP (Figure 2C). Isolated cells or focal clusters of cells were also positive for neurofilaments and NEU-N (Figure 2D). Furthermore, immunohistochemical analysis for CD34 revealed either a membranous pattern in some cells or a strong immunoreaction in a pericellular stromal pattern reminiscent of the reticulin network demonstrated by Gomori silver impregnation. Ki67 proliferative index did not exceed 2% and p53 was normal.
FINAL DIAGNOSIS


 International Society of Neuropathology
International Society of Neuropathology