Brain Pathology Case of the Month - January 2010
 Contributed by Luca Massimi, MD, Massimo Caldarelli, MD, Quintino Giorgio D’Alessandris, MD, Massimo Rollo, MD1, Libero Lauriola, MD2, Felice Giangaspero, MD3, Concezio Di Rocco, MD
Contributed by Luca Massimi, MD, Massimo Caldarelli, MD, Quintino Giorgio D’Alessandris, MD, Massimo Rollo, MD1, Libero Lauriola, MD2, Felice Giangaspero, MD3, Concezio Di Rocco, MD
 Institute of Neurosurgery, Division of Pediatric Neurosurgery, Catholic University of Rome, Italy
Institute of Neurosurgery, Division of Pediatric Neurosurgery, Catholic University of Rome, Italy
1 Department of Bio-images and Radiological Sciences, Catholic University Medical School, Rome, Italy
2 Institute of Pathology, Catholic University of Rome, Italy
3 Department of Experimental Medicine and Pathology, University "La Sapienza", Rome, Italy and IRCCS NEUROMED, Pozzilli, Italy
PART 1
Clinical history-1
This 12-year-old boy presented with a one-month history of intracranial raised pressure syndrome, characterized by headache and vomiting, followed by nuchal pain and torticollis. Physical and neurological examinations were normal except for papilledema. No hereditary syndromes were disclosed.
Neuroradiological findings-1
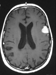
Brain MRI showed a 35 x 30 x 26 mm a grossly round, irregularly shaped tumor mass of the posterior cranial fossa, hypo/isointense on T1, iso/hyperintense on T2 and FLAIR, and heterogeneously enhanced by contrast medium (Figure 1). The tumor originated from the cerebellar vermis, extended into the paramedian region of the left cerebellar hemisphere, and compressed the fourth ventricle, causing triventricular hydrocephalus. Both spinal, infratentorial and supratentorial leptomeningeal tumor seeding were evident (Figures 2, 3). Moreover, within the left frontal lobe was present a strongly contrast-enhanced lesion considered as a possible metastasis (Figure 2).
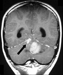
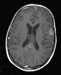



Surgical treatment and postoperative course-1
The patient underwent the excision of the vermian tumor and the treatment of the hydrocephalus (March 2007) with resolution of the preoperative clinical picture. The tumor macroscopically appeared as a reddish, soft, friable and richly vascularized mass.
Microscopic pathology-1
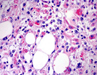
Tumor cells showed marked nuclear pleomorphism, with hyperchromatic nuclei and high mitotic activity; apoptosis was prominent (Figure 4). Immunohistochemical labeling for synaptophysin (Figure 5), chromogranin and neurofilaments was present, while no GFAP-staining was observed. Proliferation index assessed by Ki67 antibody exceeded 60%. Immunohistochemical staining expression of INI1 protein, performed with BAF47 antibody, showed nuclear expression of the protein. The total body radiological workup did not reveal evidence of primary extracranial neoplasms. What is the diagnosis of #1?
PART 2
Clinical history-2
The young boy underwent fractionated radiotherapy on the craniospinal axis plus a boost on the posterior cranial fossa followed, after a 6 weeks rest period, by 4 cycles of high-dose chemotherapy, each cycle being integrated by stem-cells rescue. Radiotherapy was carried out from April to May 2007 and consisted on craniospinal irradiation (total dose: 36 Gys) plus a conformal boost on the tumor bed (total dose: 54 Gys). Chemotherapy started on July 2007 and was completed on December 2007. Cisplatin, vincristine and cyclophosphamide were administered. All the scheduled treatment was concluded and well tolerated except for the appearance of iatrogenic Cushing disease.
Neuroradiological findings-2
The first post-treatment MRI (January 2008) showed the reduction of the leptomeningeal enhancement and the absence of local recurrences, but no changes of the left frontal mass. Such a lesion even appeared slightly increased in size at the following MRI (March 2008) (Figure 6).

Surgical treatment and postoperative course-2
The surgical removal of this mass was realized (March 2008). The tumor nodule appeared as a fatty, bloodless mass, with a little infiltration of the surrounding brain tissue. The postoperative course was uneventful.
Microscopic pathology-2
The tumor consisted of a population of pleomorphic astrocytic cells, some of them containing small hyaline eosinophilic bodies. Among them, vacuolated cells with adipocyte-like appearance were present (Figure 7). Mitoses and vascular proliferation were absent. By immunohistochemistry, the cells showed strong GFAP positivity (Figure 8). Synaptophysin and neurofilaments were negative. Ki67 proliferative index did not exceed 2% and p53 was not expressed. What is the diagnosis of #2?
PART 3
Clinical history-3
The patient underwent maintenance chemotherapy (temozolomide).
Neuroradiological findings-3
At follow-up MRIs, two progressively enlarging nodules were appreciable, the first located within the upper cerebellar vermis, close to the tentorial notch, and the second lying in the left lateral aspect of the surgical field (Figure 9).
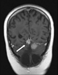


Surgical treatment and postoperative course-3
The patient was re-admitted on September 2008 because of recurrent vomiting and treated by surgical excision of these two cerebellar masses, both infiltrating and quite vascularized. The patient is currently going on with adjuvant chemotherapy.
Microscopic pathology-3
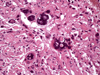
The tumor was composed of compact elongated piloid cells with occasional Rosenthal fibers (Figure 10). In some areas, the cells had bizarre appearance with large hyperchromatic nuclei. Numerous monstrous multinucleated cells were present (Figure 11). In these areas, numerous eosinophilic granular bodies and abundant Rosenthal fibers were present. No mitotic activity was observed. Infiltration of the subarachnoid space was observed in the regions were residual cerebellar tissue was present (Figure 12). By immunohistochemistry, neoplastic cells were positive for GFAP and negative for neuronal markers such as synaptophysin and neurofilaments. The Ki-67 labeling index did not exceed 3%. What is diagnosis #3?
DIAGNOSES AND DISCUSSION












 International Society of Neuropathology
International Society of Neuropathology