Brain Pathology Case of the Month - January 2009
 Contributed by Benedetta Ludovica Pettorini MD, Federica Novegno, MD, Alessandro Cianfoni*, MD,
Contributed by Benedetta Ludovica Pettorini MD, Federica Novegno, MD, Alessandro Cianfoni*, MD,
Luca Massimi, MD, Pasquale De Bonis, MD, Giuseppe Esposito, MD, Massimo Caldarelli, MD, Gianpiero Tamburrini, MD,
Concezio Di Rocco, MD, Felice Giangaspero, MD§, Libero Lauriola, MD^
 Institute of Neurosurgery, Division of Paediatric Neurosurgery, Catholic University of Rome, Italy
Institute of Neurosurgery, Division of Paediatric Neurosurgery, Catholic University of Rome, Italy
*Department of Bio-images and Radiological Sciences, Catholic University Medical School, Rome, Italy
§Department of Experimental Medicine and Pathology, University "La Sapienza", Rome, and IRCCS NEUROMED, Pozzilli (IS), Italy
^Institute of Pathology, Catholic University of Rome, Italy
CLINICAL HISTORY
This 5-year-old boy was admitted to our Department after a one month history of intracranial hypertension followed by the occurence of neurological deficits. Symptoms started with asthenia, headache, nausea and irritability. Later, right eye ptosis and deficit of lateral ocular movements appeared.
NEURORADIOLOGICAL FINDINGS
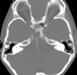
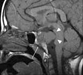
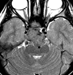
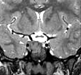
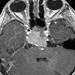
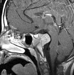
Neuroimaging showed an osteolytic lesion involving the clivus below the sella turcica plane with a large soft tissue component expanding into the intracranial compartment. The solid, lobulated mass was homogenous and enhancing, with a relatively low T2-signal suggesting high cellularity. A non-enhanced CT (Figure 1) showed the large clival osteolysis and a lesion centered in the clivus (arrow) without bone or chondroid matrix. Magnetic resonance imaging (MRI) scans showed that the mass displayed a homogeneous signal, isointense on non-enhanced T1-weighted images (sagittal and axial, Figures 2 and 3 respectively), and hypointense on T2-weighted images (coronal, Figure 4). The lesion enhanced homogeneously (axial and sagittal T1, Figures 5 and 6 respectively). MRI scans further demonstrated that the lobulated, solid mass replaced the normal high-signal intensity of the fatty bone marrow of the clivus (arrow in Figure 2) around the spheno-occipital synchondrosis, and expanded dorsally in the prepontine cistern, compressing the pons (arrowheads in Figure 2), and invading the right cavernous sinus with partial carotid artery encasement (arrowhead in Figure 3 and 4).
SURGICAL TREATMENT AND POSTOPERATIVE COURSE
An endoscopic transnasal transphenoidal resection of the lesion was performed. The approach consisted of a bilateral endoscopic transnasal posterior ethmoidotomy and sphenoidotomy, carried out to expose the superior third of the clivus. After removal of the right portion of the clivus, the tumor was reached and portions removed until the basilar artery trunk and ventral brainstem were visualized. The lesion was mainly composed of soft, elastic and fairly vascular tissues, except for some portions that were hard and poorly vascularized (similar to cartilagineous tissue). Only a partial resection was achieved due to the narrow operating field and the risk of damage to the basilar artery. The postoperative course was uneventful. The preoperative symptoms quickly disappeared and the preoperative deficits progressively improved. No cerebrospinal fluid leak was noted. A careful metastatic workup did not reveal evidence of primary extracranial neoplasms.
MICROSCOPIC PATHOLOGY

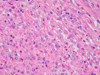
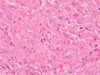





Histopathological examination revealed neoplastic spindled and rhabdoid cells with abundant eosinophilic cytoplasm, rounded nuclei and prominent nucleoli as well as numerous mitoses (Figure 7, 8, 9). The tumor cells formed nodular aggregates separated by a fibro-inflammatory stroma. Several areas of geographic necrosis were present (Figure 7). By immunohistochemistry, neoplastic cells immunostained for vimentin (Figure 10), cytokeratin 8/18, cytokeratin AE1/AE3 (Figure 11), and epithelial membrane antigen (EMA) (Figure 12). No immunostaining was observed for glial fibrillary associated protein (GFAP), S-100, placental alkaline phosphatase, α-fetoprotein, CD-117, CD-34, and CD-31. Immunohistochemistry with the BAF-47 antibody (INI1 inactivation) failed to stain neoplastic nuclei, while inflammatory and fibroblastic cell nuclei were appropriately immunostained (Figure 13). Proliferative fraction assessed by the Ki67 antibody exceeded 40% (Figure 14).
FINAL DIAGNOSIS














 International Society of Neuropathology
International Society of Neuropathology