
DIAGNOSIS: SPORADIC CREUTZFELDT-JAKOB DISEASE
DISCUSSION:
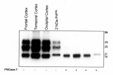
The clinical phenotype of sporadic Creutzfeldt-Jakob disease is heterogeneous both in term of clinical signs and symptoms at onset as well as the course and duration of the disease. According to established criteria a diagnosis of sCJD may be entertained in patients who have progressive dementia of less than two years' duration and at least two of the following clinical signs: myoclonus, visual or cerebellar symptoms, pyramidal or extrapyramidal signs, and akinetic mutism; "probable" or "possible" sCJD is diagnosed in the presence or absence of periodic sharp waves on EEG, respectively (1). Between 5 and 10% of patients have, however, a course of more than 2 years, and, similarly to the present patient, a combined absence of periodic EEG activity and myoclonus (2). In these subjects, validation of the diagnosis relays on neuropathological examination and demonstration of PrPSc by Western blot or immunohistochemistry. In the present case, immunostaining revealed widespread dot-like and plaque-like prion protein deposition in the outer and deeper layers of the cerebral cortex (Fig. 4A), hippocampus (Fig. 4B), striatum (Fig. 4C) and cerebellar cortex (Fig. 4D). Direct sequencing of the prion protein gene (PRNP) coding sequence, performed on genomic DNA extracted from frozen brain tissues, excluded expansions in the octarepeat region and missense mutations. The patient was methionine/valine (M/V) at the polymorphic codon 129. Immunoblot analysis for proteinase K-resistant prion protein (PrPSc) revealed the presence of a prevalent monoglycosylated PrPSc with an unglycosylated fragment size of 19 kDa (Fig. 5, lanes 1-3 and 5-8; lanes 4 and 8: frontal cortex from a classical sporadic Creutzfeldt-Jakob disease). Taken together, immunohistochemical and molecular analyses allowed a definite diagnosis of sporadic Creutzfeldt-Jakob disease.
Atypical disease presentation in sCJD includes isolated ataxia, a combination of dementia, ataxia and extrapyramidal signs, or, less frequently, neuropsychiatric symptoms/behavioral changes, which may remain stable for months or years before the onset of neurological signs. In degenerative dementia, neuropsychiatric symptoms are usually related to pathological changes in frontal and temporal lobes, and in the present case an early involvement of the frontal areas was suggested by imaging studies and focal EEG abnormalities.
Recent work has clarified that the disease phenotype in sCJD is influenced by the interaction between two different conformers of the PrPSc (type 1 with a proteinase K-resistant fragment of 21 kDa, and type 2 with a 19 kDa fragment) and the genotype at polymorphic codon 129 of the PRNP (3). Remarkably, subjects valine homozygous with either type 1 (VV1) or type 2 (VV2) and heterozygous with type 2 PrPSc (MV2) have a younger age at onset than the other patients; in addition, MV2 subjects have a significantly longer disease duration than other molecular phenotypes. Therefore, the young age at onset and the unusually long duration in the present case may have a molecular explanation.
Finally, the marked involvement of the white matter observed in this case is consistent with the panencephalopathic type of sCJD (4). Although white matter lesions were accompanied by gemistocytic glial cells proliferation, a change considered a marker of primary involvement (5), we suggest, in keeping with previous studies (6), that this may represent an end-stage condition in cases of long duration.
REFERENCES:
![]() Contributed by Gianluigi Zanusso, MD, PhD, Sergio Ferrari, MD, Stefania Conte, MD, Vittorio Mellina, MD, Vittorio Sacchi, MD, Nicola Rizzuto, MD, Salvatore Monaco, MD
Contributed by Gianluigi Zanusso, MD, PhD, Sergio Ferrari, MD, Stefania Conte, MD, Vittorio Mellina, MD, Vittorio Sacchi, MD, Nicola Rizzuto, MD, Salvatore Monaco, MD
 International Society of Neuropathology
International Society of Neuropathology