
![]() Contributed by Yujung Jung, MD and Sheldon Bastacky, MD
Contributed by Yujung Jung, MD and Sheldon Bastacky, MD
CLINICAL HISTORY
The patient was a man in his 60s with new detection of hypertension and chronic kidney disease presenting with nephrotic range proteinuria, and peripheral edema. The patient was a former smoker (50 pack years) and had used NSAID (Celebrex and Ibuprofen) for many years for his chronic back pain, but discontinued 3 months prior to kidney biopsy after he was found to have an elevated serum creatinine(Table 1) and additional pertinent labs (Table 2) include:
Urinalysis demonstrated the following:
GROSS EXAMINATION
Six cores of renal tissue measuring 0.2, 0.5, 0.5, 0.7, 0.7 and 1.2 cm in length, each measuring approximately 0.1 cm in diameter were received. A 0.5 cm core and a 1.2 cm core were submitted for immunofluorescence microscopy. A 0.5 cm core and a 0.7 cm core were submitted for electron microscopy (Karnofsky's fixative). The remainder of the tissue (a 0.2 cm core and a 0.7 cm core) was placed in the fresh formalin fixative and processed for light microscopy.
LIGHT MICROSCOPIC EXAMINATION
The tissue examined by light microscopy consists of one core of renal cortex with attached fibrous capsule. The profiles of approximately 29 glomeruli are identified in the paraffin (9 glomeruli), frozen (15 glomeruli), and plastic (5 glomeruli) sections, of which 4 (14%) are globally sclerotic. The non-obsolescent glomeruli are normocellular and normal-sized, exhibiting non-nodular, PAS-moderately positive, Congo red - negative mesangial matrix expansion and focal glomerular capillary wall thickening. Jones stain demonstrates evidence of focal glomerular basement membrane remodeling with occasional small spikes and double GBM contours. There are no proliferative lesions, necrotizing lesions, crescents, increased circulating white blood cells, hyaline thrombi, hyalinosis lesions or glomerular basement membrane breaks (H&E, PAS, Jones and trichrome stains). There is mild, patchy, chronic tubular atrophy, corresponding to 15-20% of the cortical tubular profiles. There is no tubular epithelial cell necrosis or tubulitis. No polarizable intratubular luminal crystals are identified. Jones stain reveals occasional tubular epithelial cell protein resorption droplets. The interstitium contains sparse small lymphocytes. Trichrome stain demonstrates mild to focally moderate interstitial fibrosis. Approximately five small intrarenal arteries are present in the paraffin (2 arteries), frozen (2 arteries) and plastic (1 artery) sections, exhibiting up to moderate arterial sclerosis. There is no evidence of active vasculitis, thromboemboli or thrombotic microangiopathy in the small number of extraglomerular blood vessels examined. Congo red stain is negative for amyloid.
Figure1. Light Microscopic Findings
IMMUNOFLUORESCENCE
The renal tissue examined by immunofluorescence microscopy consists of one small core of renal cortex containing 14 non-sclerotic glomeruli with non-nodular mesangial matrix expansion, 1 sclerotic glomerulus, 2 small arteries with up to moderate fibroelastic intimal thickening and approximately 5 arterioles. Chronic tubular atrophy comprises approximately 15% of the cortical tubular profiles. Direct immunofluorescence is performed using a panel of 10 antisera.
The findings included smudgy mesangial and glomerular basement membrane glomerular staining for IgG, IgA, Kappa, Lambda: 4+; C3: 2-3+; Properdin, Fibrinogen: 1-2+; IgM: trace-1+, arterial and arteriolosclerosis with associated vascular staining for complement, and nonspecific staining of hyaline casts without light chain restriction.
ELECTRON MICROSCOPY
The ultrastructural findings are based on the examination of two normocellular normal-sized glomeruli with non-nodular mesangial matrix expansion and glomerular capillary wall thickening visible on the toluidine blue-stained plastic section. Focal electron-dense hyaline material is present in Bowman's capsule. The podocytes exhibit widespread moderately severe foot process effacement. A few podocytes contain lipoprotein resorption droplets. The mesangial areas are variably expanded by increased matrix containing non-branching, haphazardly arranged fibrillary material ranging in thickness from 8.41 to 20.67 nm (mean +/- standard deviation = 15.7 +/- 5.5 nm; n = 13 measurements). The glomerular basement membrane is thickened by similar fibrillary material, and is associated with variable remodeling with associated new irregular layers of lamina densa. The glomerular capillaries are patent, containing a few circulating red blood cells and a rare circulating lymphocyte. The endothelial cells range from normal with preserved fenestrations to swollen with loss of fenestrations. No endothelial cell cytoplasmic tubuloreticular inclusions are identified. The few tubules have epithelial cells with focal cytoplasmic vacuolization. The tubular basement membranes are otherwise unremarkable. Two arterioles exhibit hyaline arteriolar sclerosis. No extraglomerular fibrillary material is identified in the tissue examined by EM.
Figure 2. Electron Microscopic Findings:
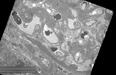
B. Non-branching, haphazardly arranged fibrillary material in expanded mesangium, (fibril diameters ranging from 15.7Ý5.5 nm)

C. Patent glomerular capillaries with circulating red blood cells and a lymphocyte
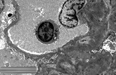
D. Tubular epithelial cells with focal cytoplasmic vacuolization

ANCILLARY STUDIES
Immunohistochemical staining for DNA-JB9 was performed, which was strongly positive in the mesangial matrix and GBMs (Figure 3).
Figure 3. Immunohistochemical staining for DNA-JB9