Case 1048 - A 21-Year Old Male with One-Month Histolry of Vomiting

 Contributed by Takahiro Aoki, MD1, Hiroshi Kishimoto, MD2, Junko Hirato, MD, PhD3, Yonehiro Kanemura, MD, PhD4, Makiko Mori, MD1, Yuki Arakawa, MD1, Jun Kurihara, MD5, Eiji Oguma, MD6, Katsuyoshi Koh, MD1
Contributed by Takahiro Aoki, MD1, Hiroshi Kishimoto, MD2, Junko Hirato, MD, PhD3, Yonehiro Kanemura, MD, PhD4, Makiko Mori, MD1, Yuki Arakawa, MD1, Jun Kurihara, MD5, Eiji Oguma, MD6, Katsuyoshi Koh, MD1
 1Department of Hematology/Oncology, Saitama Children's Medical Center,
1Department of Hematology/Oncology, Saitama Children's Medical Center,
2Department of Clinical Laboratory, Saitama Children's Medical Center,
3Department of Pathology, Gunma University Hospital,
4Division of Regenerative Medicine, Institute for Clinical Research, Osaka National Hospital, National Hospital Organization,
5Department of Neurosurgery, Saitama Children's Medical Center, 6Department of Radiology, Saitama Children's Medical Center
CLINICAL HISTORY

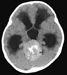
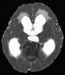
A previously healthy 21-month-old male presented with a 1-month history of vomiting, gait disturbance, and abnormal ocular alignment. He had papilledema, but no convulsions or abnormal consciousness. A CT scan revealed hydrocephalus (Figure 1a) and a cerebellar tumor measuring 4 cm in diameter (Figure 1b). Apparent diffusion coefficient map demonstrated strong restricted diffusion in the tumor (Figure 1c). The tumor was totally resected on the day after admission, and had not spread into his cerebrospinal fluid at surgery; however, the tumor progression was very aggressive. Only two weeks after surgery, and prior to any chemotherapy, the tumor had spread to his spinal cord leptomeninges, causing neoplastic meningitis. Moreover, although he was in remission after a cycle of chemotherapy (cyclophosphamide, cisplatin, vincristine, etoposide, and intrathecal methotrexate), the tumor relapsed quickly during additional chemotherapy. We prescribed an anthracycline-containing regimen and irradiation sequentially; however, the tumor did not regress. He survived only seven months after his diagnosis.
MICROSCOPIC PATHOLOGY


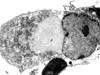



H&E staining showed that the tumor mainly had densely packed small undifferentiated cells, including large cells with prominent nuclei (Figure 1d), and partially had different cells with an eosinophilic globular cytoplasmic inclusion (Figure 1e). The inclusion body was also detected on electronic microscopy (Figure 1f). Immunohistochemistry showed that both tumor lesions were positive for INI1, (Figure 1g), Brahma-related gene 1 (BRG1, Figure 1h), synaptophysin (Figure 1i), nestin, neurofilament protein, and desmin. Small undifferentiated cells were negative for alpha smooth muscle actin (a-SMA), EMA, and cytokeratin (CAM5.2), and the other cells were negative for CAM5.2 and weakly positive for a-SMA and EMA. The Ki-67 index was up to 90% in both lesions. What is your diagnosis?
FINAL DIAGNOSIS













