
![]() Contributed by Andrew Freeman, MD and Kenichi Tamama, MD, PhD
Contributed by Andrew Freeman, MD and Kenichi Tamama, MD, PhD
CLINICAL HISTORY
The patient is an adult female who presents to the emergency department with complaints of nausea over the past few days and one day of non-bloody, non-bilious emesis. The patient was recently pregnant and delivered a baby girl a few months ago. Although she has been having difficulty keeping food and fluids down, she is continuing to breast feed her daughter. The patient endorses having a cold about a week ago, but denies any new foods, recent travel, sick contacts, diarrhea, illicit drug use, or toxic ingestions. Physical exam is notable for dry mucous membranes and tachycardia. The patient is otherwise afebrile, with a blood pressure of 120/80 mmHg, heart rate of 126 beats per minute, respiratory rate of 16 breaths per minute, and an oxygen saturation of 100% on room air.
Initial labs in the emergency department were notable for hyperkalemia, decreased total CO2, and an elevated white blood cell count (Tables 1 and 2). A urinalysis was notable for elevated ketones, 1+ leukocyte esterase, negative urine nitrite, 2+ protein, 79 WBCs, 4 RBCs, 13 squamous epithelial cells, and 3+ bacteria. Initially a venous blood gas was obtained, with follow up arterial blood gases during the patient's hospital stay (Table 3). Blood and urine cultures were drawn. Salicylate and acetaminophen levels, urine drug screen, volatile alcohol panel, and urine organic acids were ordered.
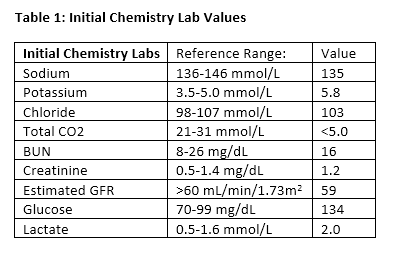
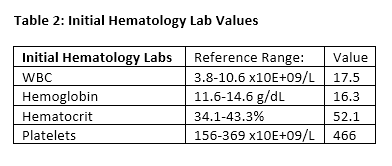
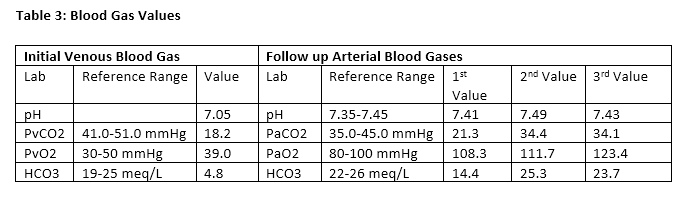
The patient was initially started on antibiotics for concern of a potential UTI (vs. contaminated urinalysis) in the setting of an elevated anion gap metabolic acidosis. The patient was additionally given IV fluids, calcium gluconate, insulin, dextrose, bicarbonate, ondansetron, and thiamine. Because of the concern for a potential toxic alcohol/diol poisoning with an elevated anion gap metabolic acidosis, and a mildly decreased eGFR with high-normal creatinine suggestive of a mild AKI, the patient was given one dose of fomepizole while toxicology labs were pending.
The patient was transferred to the ICU for further management of her severe metabolic acidosis. The following day, her condition improved. Serum/plasma toxicology labs were negative for propylene glycol, ethylene glycol, salicylate, or acetaminophen. The initial immunoassay urine drug screen was negative and no illicit substances were found on urine comprehensive drug screen by gas chromatography/mass spectrometry. A volatile alcohol panel by gas chromatography-headspace showed no detectable amounts of ethanol, isopropanol, or methanol, but was positive for acetone at 30 mg/dL. Beta-hydroxybutyrate levels were elevated at 6.88 mmol/L (RR: <0.28 mmol/L). Repeat lactic acid remained elevated at 2.1 mmol/L. Follow up arterial blood gas labs showed an improvement in the patient's elevated anion gap metabolic acidosis (Table 3). The patient's potassium levels responded to treatment after initially rising to a peak of 6.4 mEq/L, falling to a low of 2.9 mEq/L, and eventually reaching 4.0 mEq/L. The patient's mild AKI improved with repeat creatinine of 0.7 mg/dL and an improved eGFR. Random urine organic acid testing by gas chromatography/mass spectrometry showed a severe lactic aciduria with ketonuria. Blood and urine cultures were negative and antibiotics were discontinued. The patient noted that she was feeling better and was able to eat food. Her physical exam had also improved. She was transferred out of the ICU and later discharged in stable condition.