FINAL DIAGNOSIS
Fetal and neonatal allo-immune thrombocytopenia (FNAIT)
DISCUSSION
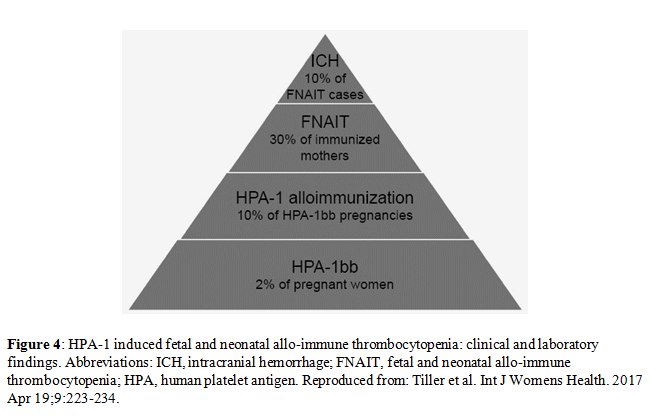
Fetal and neonatal allo-immune thrombocytopenia (FNAIT) is a condition in which the mother makes antibodies directed against an antigen on fetal/ neonatal platelets, which she lacks. The most commonly implicated antigens are human platelet antigens (HPA) followed by class I human leukocyte antigens (HLA). The frequency varies by source, but may be as high as 1 in 1500 neonates, although most cases are asymptomatic or are associated with mild to moderate thrombocytopenia with little clinical sequelae. The most common etiology is a mother with a HPA-1b/1b genotype carrying a fetus with an HPA-1a/1a genotype. In this case, the fetal platelets possess the HPA-1a antigen inherited from the father. The mother forms IgG antibodies against HPA-1a, which then cross the placenta and bind to the fetal platelets. The clearance of the antibody-coated platelets results in fetal and neonatal thrombocytopenia, which can be severe with intracranial hemorrhage occurring in 10% of FNAIT cases. Unlike the sensitization process which is required to form antibodies against antigens in the RH red cell antigen system, antibodies directed against human platelet antigens can occur in the first pregnancy and in all subsequent pregnancies if the platelet antigen which the mother lacks is present in the fetus.


For neonates with thrombocytopenia requiring transfusion, the mainstays of therapy are IVIg and platelets. IVIg blocks the reticuloendothelial system increasing platelet survival in the neonate's circulation. The typical dose administered is 1 g/kg/d for 2 consecutive days or 400 mg/kg per day over 5 days. Ideally, platelets for transfusion should be negative for the antigen to which the mother has made an antibody, although in practice this is rarely available. Random donor platelets are usually transfused initially as a temporizing measure. Random platelets adsorb the maternal antibody from the neonate's circulation so with repeated transfusions (re-equilibration of IgG from the extravascular compartment occurs after each transfusion), the platelet count usually starts increasing after approximately two weeks. There is an 80-90% response rate to IVIg and random donor platelets. Some blood centers keep HPA-1a and HPA-5a negative platelets in inventory or have a database of HPA-1a and HPA-5a negative donors. These platelets should lead to adequate increments in 95% of cases of FNAIT. If the neonate fails to respond to IVIg and random donor platelets and antigen negative platelets are unavailable, washed or plasma-volume reduced maternal platelets (to remove the anti-platelet antibody) collect by apheresis can be used.
In the postpartum workup, screening the maternal serum for HPA antibodies must be performed to determine whether the mother has specific antibodies directed against the antigen missing from her platelets. Testing can include a crossmatch between maternal serum and paternal platelet glycoprotein (GP) IIb/IIIa, which is most commonly implicated in FNAIT. A modified antigen capture enzyme-linked immunosorbent assay (MACE) or Monoclonal Antibody-specific Immobilization of Platelet Antigen (MAIPA) assay can be used to evaluate for the presence of antibodies in maternal serum directed against paternal platelet glycoproteins. Maternal serum is also evaluated for the presence of antibodies against class I human leukocyte antigens (HLA), which are an infrequent cause of FNAIT. Genotyping of the maternal and paternal (or neonatal) platelets in cases of suspected FNAIT should be done as quickly as possible. Maternal genotyping is also appropriate for women with a personal pregnancy history which suggests FNAIT or who have a sister whose child was affected by FNAIT.
For women at risk of having a pregnancy impacted by FNAIT, there are several important interventions which can be implemented to reduce the risk of morbidity. This includes the administration of IVIg during pregnancy, which is given as IVIg 2 g/kg/week or IVIg 1 g/kg/week with prednisone 0.5 mg/kg/day starting at 20 weeks followed by IVIg at 2 g/kg/week with prednisone 0.5 mg/kg/day starting at 32 weeks. Cesarean section at 37 to 38 weeks is recommended to reduce the risk of intracranial hemorrhage and fetal trauma. For women who are deemed to be at extremely high risk, such as those who had a prior neonate with intracranial hemorrhage, IVIg can be initiated earlier in the pregnancy (12 weeks), and these women should be followed with increased vigilance.
REFERENCES
![]() Contributed by Jansen N Seheult, MB BCh BAO and Alesia Kaplan, MD
Contributed by Jansen N Seheult, MB BCh BAO and Alesia Kaplan, MD